Dental Implant Material Types

Are you looking to restore your smile despite missing teeth? Dental implants offer a reliable solution, blending seamlessly with your natural teeth.
The key to their success lies in materials like titanium, zirconia, or ceramics.
Each material has unique advantages and disadvantages, so discussing your options with your dentist to determine which is best for you is essential.
Recommended Reading: Dental Implants | The Ultimate Guide
Types of Dental Implants
When it comes to dental implants, there are several types available.
Need Dental Advice? It’s FREE!
Each type is designed to meet specific needs, and your dentist will help you determine which type is best for you. Here are a few of the most common types of dental implants:
Endosteal Implants
Endosteal implants, the most prevalent dental implant type, are placed directly into the jawbone and crafted from titanium or zirconia.
They’re perfect for patients with healthy jawbones seeking a durable solution for missing teeth, offering a favored alternative to removable dentures or bridgework.
A recent study found that the overall 1-, 5-, and 10-year survival rates of all implants were 96.6%, 96.6%, and 86.9%, respectively.
Subperiosteal Implants
Though less common, subperiosteal implants provide a viable option for certain patients.
Positioned atop the jawbone but beneath gum tissue, these implants cater to those without sufficient healthy jawbone to support endosteal implants.
All-on-4
The All-on-4 dental implant system is designed for patients missing most or all of their teeth.
It uses four implants to anchor an entire arch of replacement teeth, providing a more affordable option than traditional dentures.
Recommended Reading: Throbbing Pain After Dental Implant Crown (Common Reasons)
While the procedure may be more invasive, the All-on-4 system offers patients the advantage of having a permanent, non-removable denture immediately after surgery, resulting in a complete and quick tooth restoration.
The success rate of the All-on-4 dental implant technique is very high, with over 97% success rate, according to one source.
Mini Dental Implants
Mini dental implants are a smaller version of traditional dental implants.
These implants are ideal for patients who do not have enough jawbone to support a larger implant. Mini dental implants are also an excellent option for patients looking for a less invasive and more affordable alternative to traditional implants.
A retrospective analysis of 5640 mini dental implants found an overall survival rate of 92.1%
Dental Implant Material Types
Regarding dental implants, several materials are used in their construction.
The most common materials used in dental implants are titanium, zirconia, and ceramic. Each material has its advantages and disadvantages. In this section, we’ll discuss each of these materials in detail.
Recommended Reading: 7 Symptoms of Perforated Sinus After Dental Implant
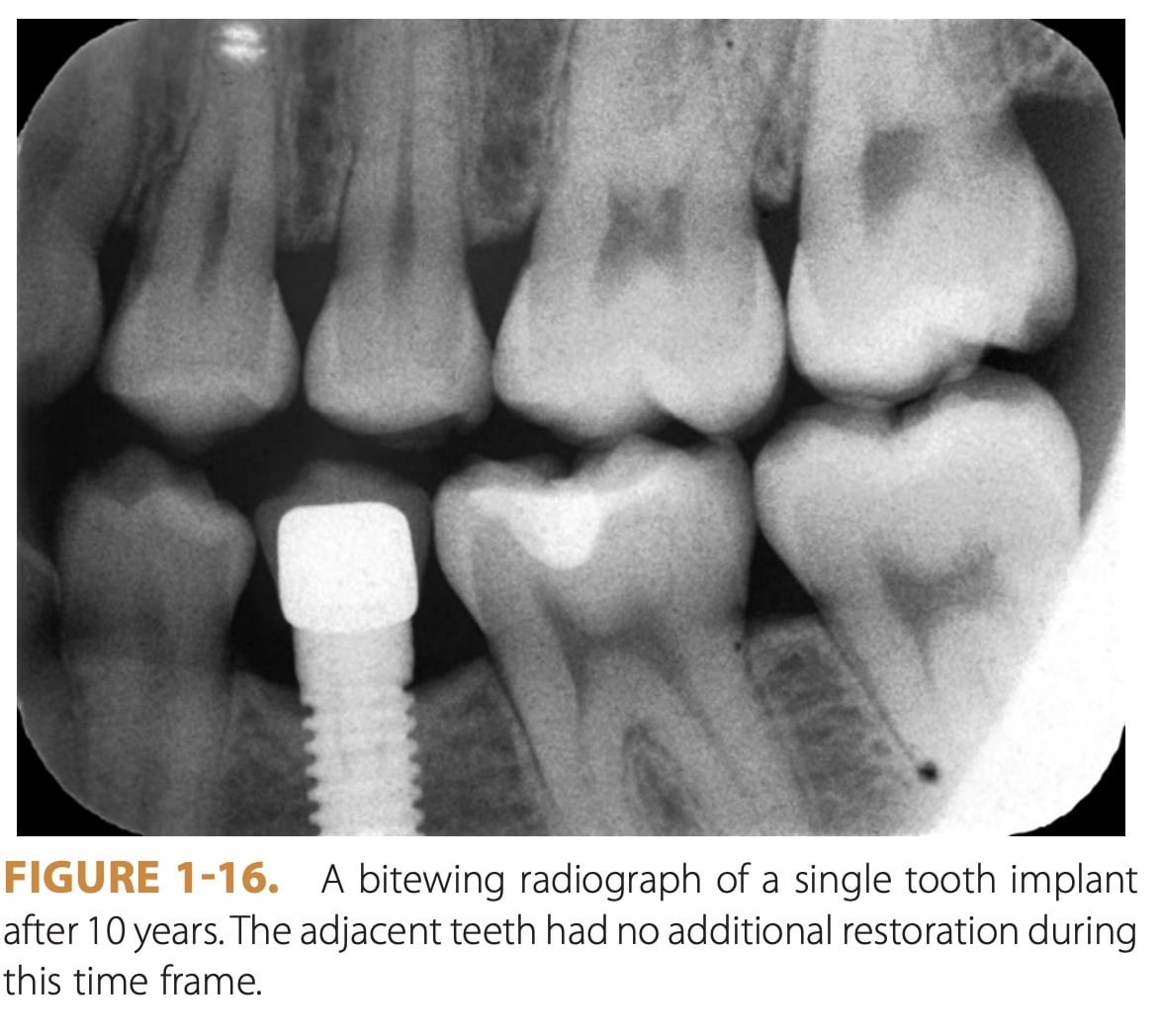
Titanium Implants
Titanium implants are the most common type of dental implant used today. Titanium is a solid and durable metal that provides excellent stability to implanted teeth.
Most people can tolerate titanium or an alloy well without developing an allergic reaction to the metal.
Titanium implants are also biocompatible, meaning they can fuse with the jawbone, providing a solid foundation for the implant.
Zirconia Implants
Zirconia implants are made from zirconium oxide, a white, ceramic-like material. Unlike titanium, zirconia is white.
Zirconia abutments are a popular replacement for metal abutments that may exhibit a gray hue under the dental crown.
Zirconia implants are also biocompatible and can fuse with the jawbone, providing a strong foundation for the implant. However, zirconia implants are less robust than titanium implants and more prone to fracture.
Recommended Reading: 12 Best Dental Implant Brands 2023 (Dentist’s Perspective)
Ceramic Implants
Ceramic implants have recently gained popularity as an attractive, biocompatible option for dental restorations. Made from high-quality alumina or zirconia ceramics, these implants offer patients a tooth-colored solution that blends seamlessly with their natural teeth.
Ceramic and zirconia implants are interchangeable and analogous when it comes to implants. Additionally, they exhibit low plaque affinity, which can help reduce the risk of gum disease and inflammation around the implant site.
Implant Placement & Surgery
Dental implant surgery is a process that involves the placement of a dental implant into the jawbone to replace a missing tooth or teeth.
The implant placement process involves several steps, including tooth extraction (if necessary), bone grafting, implant placement, osseointegration and abutment/crown delivery.
The procedure’s success depends on the implant material, the surgeon’s skill, and the patient’s oral health.
Implant Placement Process
The implant placement process begins with thoroughly evaluating the patient’s oral health. Next, the dentist will take x-rays of the patient’s teeth to determine the best location for the implant.
The implant placement procedure is typically performed in two stages, with a healing period in between.
During the first stage, the surgeon will incision the gum tissue and drill a small hole in the jawbone. Next, the implant is placed into the hole and covered with a protective cap.
The gum tissue is then stitched closed, and the patient is sent home to heal.
Bone Grafting
To ensure the success of the implant, the bone surrounding the implant must be healthy and strong. If the bone is too thin or weak, the surgeon may need to perform a bone graft to strengthen the area.
This involves taking bone from another part of the patient’s body or using synthetic bone material (most common) to build up the jawbone.
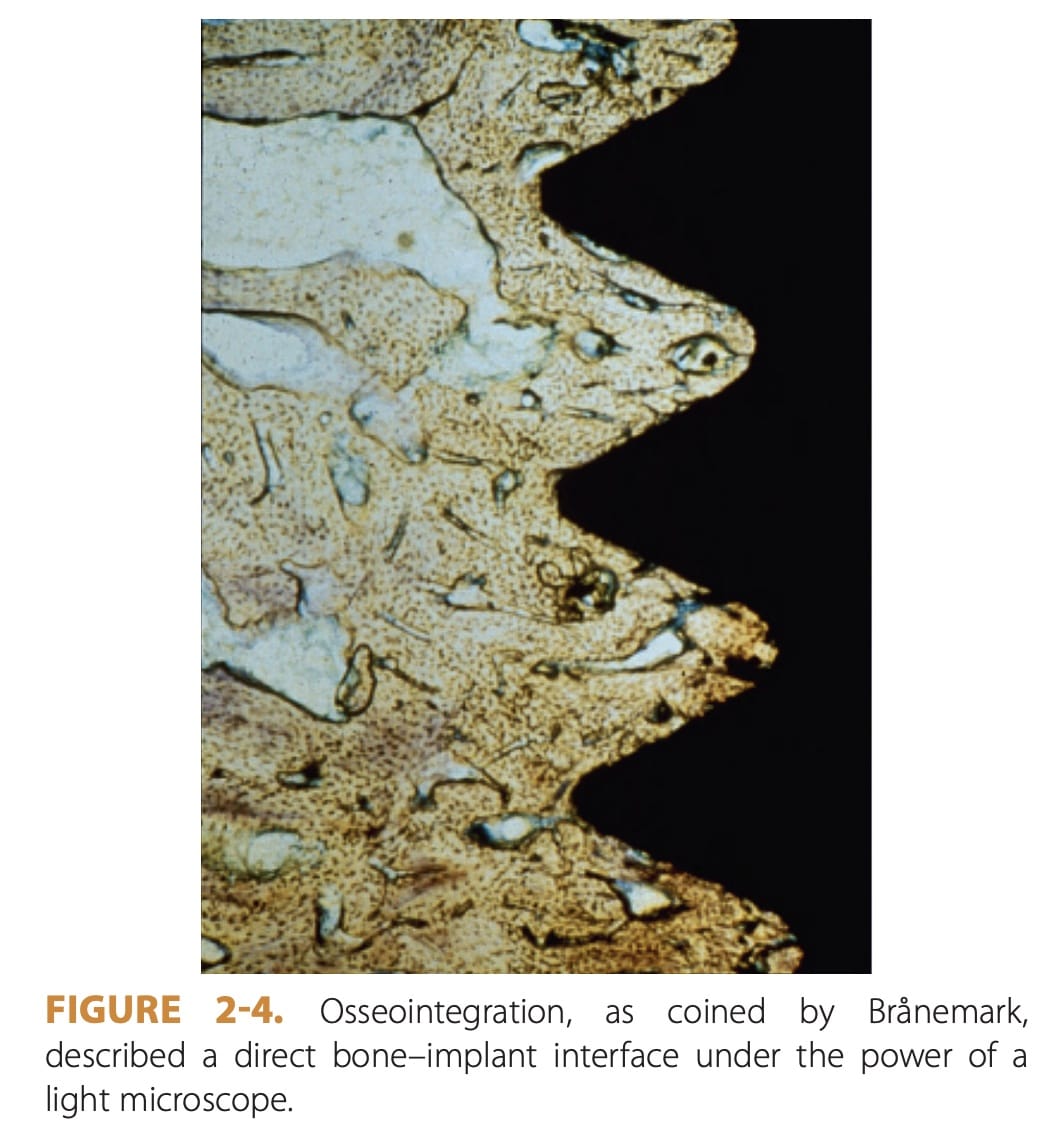
Healing & Osseointegration
After the abutment is placed, the patient will need to allow time for the implant to heal and osseointegrate, which means the implant will fuse with the jawbone.
This process can take several months, during which the patient must follow a strict oral hygiene routine to ensure the implant’s success.
During the healing period, the dentist will monitor the patient’s progress and may take additional X-rays to ensure the implant integrates appropriately.
Once the implant has fully fused with the jawbone, the final crown or bridge can be attached to the abutment, completing the dental implant process.
Abutment Placement
Once the healing process is complete, the protective cap is removed, and the abutment is affixed to the implant.
The abutment is a small connector that links the implant to the crown or bridge placed on top of it.
The abutment placement procedure is typically performed under local anesthesia and is relatively quick. Generally, the abutment is positioned on the same day as the implant crown delivery.
However, it may be placed during the day of the impression to ensure the dental lab can create an accurate dental crown.
Crown Delivery
The crown delivery process involves the dentist securing the abutment into the implant using a hand instrument.
Cotton is then placed inside the abutment to prevent cement from adhering to the screw, and finally, the dental crown is cemented to the implant.
Dental implant crowns can be either “screw-retained” or “cement-retained.” Screw-retained crowns combine the abutment and crown into a single unit, which is then screwed into place.
No dental cement is needed; however, dental composite is applied over the access hole to prevent food particles from entering.
In contrast, cement-retained crowns first involve screwing in the abutment, then cementing the dental crown to complete the restoration.
Bone Grafting & Ridge Augmentation
If you have experienced bone loss due to tooth decay or gum disease, your dentist may recommend a bone graft to help rebuild the bone in your jaw.
A bone graft involves taking bone from another part of your body or using synthetic material (the most common method) to create new bone in the affected area.
This new bone can then be used to support a dental implant.
Type of Bone Grafts
- Autografts: Bone tissue taken from your own body, typically from your chin, shin, or hip.
- Allografts: Bone tissue obtained from a human donor, usually cadaver bone, has undergone treatments to make it neutral to immune reactions and free of host diseases.
- Xenografts: Bone tissue obtained from another species, such as bovine or porcine bone.
After a bone graft, your dentist may also recommend ridge modification to help reshape the bone in your jaw. Ridge modification involves removing excess bone or tissue and reshaping the remaining bone to support a dental implant.
Ridge modification can be used to correct a variety of issues, including:
- Uneven jawbone
- Insufficient bone height
- Narrow jawbone
Ridge modification can significantly improve the appearance and function of dental implants, increasing the chances of successful implants that can last for years to come.
Complications & Risks
Dental implants are generally considered a safe and effective treatment to replace missing teeth.
However, as with any surgical procedure, there are some risks involved.
This section will discuss some of the most common complications and risks associated with dental implants.
Infection
Infection is a risk with any surgical procedure, including dental implant surgery. Signs of infection include redness, swelling, and pain around the implant site.
In some cases, the implant may need to be removed if the infection is severe. To reduce the risk of infection, your dentist may give you antibiotics before and after the procedure.
Nerve Damage
Nerve damage is a rare but severe complication of dental implant surgery. It can cause pain, numbness, or tingling in your natural teeth, gums, lips, or chin. In some cases, nerve damage can be permanent.
Therefore, your dentist will take special care to avoid damaging nerves during the procedure.
Implant Failure
Implant failure is another rare but severe complication of dental implant surgery.
It occurs when the implant does not fuse with the jawbone properly. This can happen for various reasons, including poor oral hygiene, smoking, and certain medical conditions.
If implant failure occurs, the implant may need to be removed and replaced.
The failure rate of dental implants varies depending on several factors. However, studies have shown that the failure rate ranges from 3.11% to 10%.
Aftercare and Maintenance
After your dental implant surgery, proper care and maintenance are crucial to ensure the longevity of your implant. Here are some essential things to keep in mind:
Oral Hygiene
Maintaining good oral hygiene is essential for the health of your dental implant. Brush your teeth twice daily with a soft-bristled brush and use an antimicrobial mouthwash to prevent infection.
Regular flossing is also important to remove plaque and food debris between your teeth and around your implant.
Chewing & Speech
Dental implants are designed to function like natural teeth, so you should be able to eat and speak normally. However, getting used to the implant may take some time, especially if it’s your first one.
Start with soft foods and gradually move to harder, chewier foods. If you experience any difficulty speaking or chewing, contact your dentist.
Appearance
Dental implants are designed to look and feel like natural teeth, so they should blend in seamlessly with your smile. However, keeping your implant clean and free of stains is vital to maintain its appearance.
Avoid smoking and limit your consumption of foods and drinks that can stain your teeth, such as coffee, tea, and red wine.
Dental Exams & Follow-up Care
Regular dental exams are important to monitor your implant’s health and ensure its functioning properly.
Your dentist will check the implant for any signs of infection or other issues and may recommend additional treatments or adjustments if necessary.
Follow-up care is also essential to ensure the long-term success of your implant.
In summary, proper care and maintenance are essential for the health and longevity of your dental implant.
By following these guidelines and working closely with your dentist, you can enjoy a healthy, functional smile for years.
Special Considerations
When considering dental implants, there are a few special considerations that you should keep in mind. These include sinus problems and augmentation, diabetes, and dental insurance.
Sinus Problems & Augmentation
If you have sinus problems or require sinus augmentation, discussing this with your dentist before dental implants is important.
Sinus problems can affect the success of dental implants, and sinus augmentation may be necessary to ensure enough bone to support the implant.
Diabetes & Implants
If you have diabetes, you may be concerned about the success of dental implants.
While diabetes can affect the healing process, it does not necessarily mean you are not a candidate for dental implants.
However, it’s important to discuss your diabetes with your dentist and follow a strict oral hygiene routine to ensure the success of your dental implants.
According to a systematic review and meta-analysis, dental implants in diabetic patients showed a 77.7% higher risk of failure than non-diabetic patients.
Dental Insurance
Dental insurance can be a concern for many people considering dental implants.
While some dental insurance plans may cover the cost of dental implants, others may not. Therefore, checking with your dental insurance provider to see what is covered and what is not is essential.
In some cases, dental insurance may cover the cost of the implant itself but not the crown or abutment. This is something to remember when considering the cost of dental implants.
Finding the Right Dental Professional
When it comes to dental implant surgery, it is important to choose the right dental professional with the necessary training and experience to perform the procedure safely and effectively.
Here are some types of dental professionals you may consider:
General Dentist
A general dentist can perform dental implant surgery, but they may not have the specialized training and experience of other dental professionals. Consider a specialist if you have a complex case, such as multiple missing teeth or significant bone loss.
Oral and Maxillofacial Surgeon
An oral and maxillofacial surgeon is a specialist who has completed four years of dental school and an additional four years of surgical residency training.
They have extensive knowledge and experience in surgical procedures of the mouth, jaw, and face, including dental implant surgery. They can also provide various types of anesthesia to ensure your comfort during the procedure.
Periodontist
A periodontist is a specialist who has completed three years of additional training after dental school in diagnosing and treating gum disease and placing dental implants.
In addition, they have expertise in preserving and enhancing the bone and gum tissue around the implant site to ensure long-term success.
Prosthodontist
A prosthodontist is a specialist who has completed three years of additional training after dental school in the restoration and replacement of teeth. They have expertise in designing and placing dental restorations that attach to dental implants, such as crowns, bridges, and dentures.
When choosing a dental professional for dental implant surgery, you should consider their training, experience, and reputation.
It is also essential to discuss the anesthesia used during the procedure and any potential risks, such as numbness or nerve damage. Therefore, the FDA recommends that dental implant surgery be performed in an outpatient setting to ensure safety and comfort.
Finding the right dental professional for your dental implant surgery can help ensure a successful outcome and a beautiful, functional dental restoration for your missing teeth.
My Experience & Expertise
As a dentist, I have worked with various dental implant materials.
Through my years of practice, I have gained extensive knowledge and expertise in the field, allowing me to provide my patients with the best possible treatment options.
I have found three main types of dental implant materials: titanium, zirconia, and ceramic. Each material has unique properties and benefits, and I always consider a patient’s specific needs and preferences when recommending a material.
Need a second opinion? We can help! Learn more. Knowledge is power when cultivating healthy dental habits. The more informed you are, the better positioned you’ll be to prevent avoidable and potentially costly dental procedures for you and your family. Watch for future blog posts, where we’ll continue sharing important information, product reviews and practical advice!

About the Author
Dr. Matthew Hannan is a board-certified dentist on a mission to provide accurate dental patient education. He attended Baylor University before completing dental school at UT Health San Antonio School of Dentistry. He now lives in Arizona with his beautiful wife and 4 kids. Dr. Hannan believes everyone should access easy-to-read dental resources with relevant, up-to-date dental research and insight to improve their oral health.

Connect with Dr. Hannan!
-
Dental Second Opinion | Ultimate Guide (Content Hub)
Dental second opinions are essential for expert oral health care, clarity and peace of mind. Are you considering a second opinion? My Dental Advocate can help! Read this ultimate guide to learn more…
-
BURST Pro vs. Sonic Toothbrush (Comparison Review)
When it comes to keeping our pearly whites, well, white, the Burst Pro Sonic and Burst Original Sonic electric toothbrushes both claim to be at the top of their game. But when these two contenders go head-to-head, which one will leave us with that just-left-the-dentist clean feeling, and which will fall short?
-
5 Best Electric Toothbrush for Gingivitis 2026 (Dentist-Recommended)
Ever wake up with swollen, tender gums, wincing as you brush your teeth in the morning? If so, you might be one of the millions of people battling gingivitis, a common gum disease that can be painful and, left untreated, can lead to more serious oral health issues.
Gain Clarity with Our FREE Second Opinion Guide
FREE online second opinion within 48 hours. No joke!
Product Reviews
Our 300+ dental product reviews (and counting), curated by an experienced dentist, are the most comprehensive online.
Toothbrush Genie
State-of-the-art chatbot designed to help you discover your perfect toothbrush in just a few simple steps!
Cavity Risk Assessment
Cutting-edge digital tool designed to evaluate your individual cavity risk based on your responses to a series of questions.
Gum Disease Assessment
Discover your gum disease risk with our quick and engaging 6-question assessment!






