What Are Dental Implants?
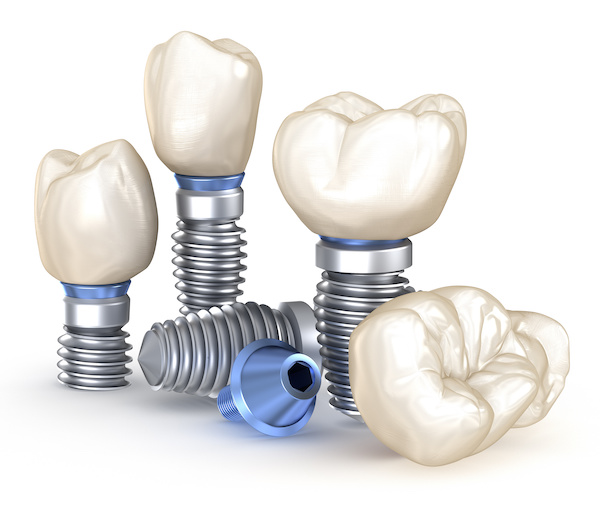
Replacing a permanent tooth is not new; our ancestors had to contend with it for generations, with some creative solutions.
Implant technology has dramatically advanced over the past 50 years and has shown great promise for predictable longevity.
There are multiple implant companies today, and most use bioactive titanium-coated implants that assimilate with the jaw bone.
Oral surgeons and periodontists place most implants.
However, many general dentists have completed advanced training and are also competent.
Implant Information
There are two types of implant techniques: immediate and delayed implants.
Immediate implants occur immediately after the extraction and require adequate bone for retention and engagement of the implant.
Premolars and anterior teeth are the most common sites for immediate implants. On the other hand, delayed implants occur four months after extraction and are considered less risky for implant failure.
Recommended Reading: Top 5 Brushing Habits to Break in 2026
Why Do Implants Fail?
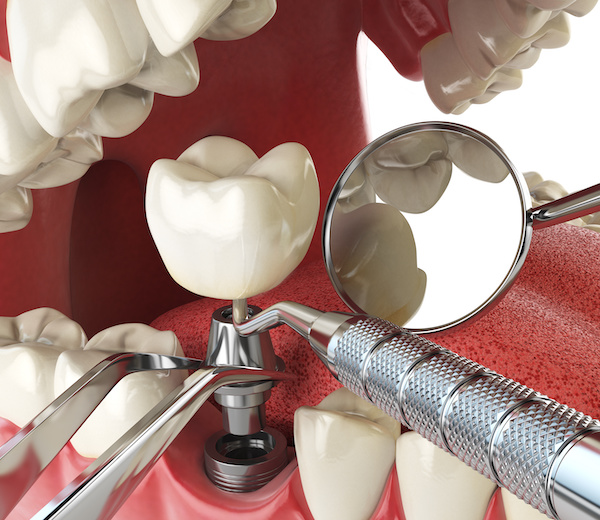
According to multiple retrospective studies, dental implants have a 98% success rate.
Although rare, implants can fail, and the most common reasons are poor oral hygiene, medical issues with delayed healing (diabetes), smoking, and poor surgical technique.
The gum tissue is sutured closed after the implant is placed, and the healing begins.
If the surgical site is not cared for or cleaned properly, bacteria can congregate and penetrate the vulnerable tissues, impeding healing.
Like smoking, failure will occur if contaminants interfere with the healing process.
If a failure occurs, it often occurs soon after the implant is placed.
If the patient has diabetes or other medical conditions that inhibit healing, it may affect the success rate of dental implants. Having your primary care physician verify that your physical health is stable and controlled for a predictable outcome.
Lastly, the surgical technique can affect the success rate of dental implants.
If contamination occurs during the placement process or the implant is torqued too quickly, the bone tissue may be altered, leading to poor osseointegration and implant failure.
Therefore, it’s paramount that the clinician is well-trained and competent in the placement of dental implants.
Implant Bite (Occlusion)
After the final crown is secured to the implant, ideal occlusion is required for the implant’s long-term success.
Preserving the bone structure that houses the implant is done by limiting excess occlusal forces, limiting excursive chewing forces, and limiting bacteria buildup around the implant.
Natural teeth have a ligament around the tooth known as the periodontal ligament (PDL), which acts as a shock absorber when chewing.
Unfortunately, dental implants lack this, so the occlusal contacts should compensate for this. This means the impact with the opposing tooth should be light when your teeth come together and are non-existent in an excursive or side-to-side movement.
If contacts are present when you chew side to side, the forces will negatively affect bone integration and may lead to implant failure. A nightguard is highly recommended to prevent unnecessary force if you grind your teeth.
Related: Learn more about Crowns
Implant Care & Maintenance
An implant’s ” waist ” is narrower than a natural tooth, so it’s essential to floss well below the gum line to remove plaque on the metal abutment. The abutment connects the crown to the implant post, inserted into the bone.
Also, because the “waist” is narrower, food impaction around the implant is possible, as the gum tissue cannot fill the space between the implant and the adjacent natural tooth.
As a result, over time, the bone around the implant may slowly resorb away from the top of the implant, causing the gum tissue to recede and expose a gap between the teeth, known as a “black triangle.”
This can be unsightly, especially between your front teeth, so it’s essential to limit plaque build-up that could accelerate the formation of “black triangles.”
When your implants are being cleaned, your hygienist will use a rubber-tipped ultrasonic scaler or a titanium hand scaler to carefully clean away plaque and tartar without damaging the implant surface.
Like natural teeth, the gum tissue will attach to the abutment to seal and prevent bacteria from penetrating the bone.
If bacteria begins to formulate along the gum line, it can damage this attachment and potentially lead to bone loss and implant failure.
Related: Best MDA Recommended Products
My Experience & Expertise
Dental implants are expensive and require months of healing.
Therefore, it’s essential to understand the pros and cons of your dental implant options and how to maintain them for long-term success.
Have you recently been diagnosed with needing an implant? Do you understand your alternative options?
My Dental Advocate’s team of board-certified dentists can provide a second opinion on your planned treatment. We look forward to bringing you peace of mind by verifying your treatment plan, suggesting an alternative, or answering your questions.
Need a second opinion? We can help! Learn more. Knowledge is power when cultivating healthy dental habits. The more informed you are, the better positioned you’ll be to prevent avoidable and potentially costly dental procedures for you and your family. Watch for future blog posts, where we’ll continue sharing important information, product reviews and practical advice!

About the Author
Dr. Matthew Hannan is a board-certified dentist on a mission to provide accurate dental patient education. He attended Baylor University before completing dental school at UT Health San Antonio School of Dentistry. He now lives in Arizona with his beautiful wife and 4 kids. Dr. Hannan believes everyone should access easy-to-read dental resources with relevant, up-to-date dental research and insight to improve their oral health.

Connect with Dr. Hannan!
-
Best Toothbrush for Gum Disease (Full Review)
Are you experiencing gum disease? If so, you’re not alone. Gum disease affects 42% of adults over 30 and 70% of adults over 65. Fortunately, there are steps you can take to prevent and treat gum disease, including using an electric toothbrush.
-
Sonicare 1100 Toothbrush (Full Review)
If you’re in the market for an electric toothbrush that delivers a deep clean for an affordable price, the Philips Sonicare 1100 Electric Toothbrush is definitely worth checking out. Its simple design, sonic technology…
-
Best Affordable Electric Toothbrush 2026
Looking for an electric toothbrush that’s easy on your wallet yet delivers exceptional results? You’ve come to the perfect spot! As a dentist who’s reviewed 200+ dental products, I know the significance of discovering an economical…
Gain Clarity with Our FREE Second Opinion Guide
FREE online second opinion within 48 hours. No joke!
Product Reviews
Our 300+ dental product reviews (and counting), curated by an experienced dentist, are the most comprehensive online.
Toothbrush Genie
State-of-the-art chatbot designed to help you discover your perfect toothbrush in just a few simple steps!
Cavity Risk Assessment
Cutting-edge digital tool designed to evaluate your individual cavity risk based on your responses to a series of questions.
Gum Disease Assessment
Discover your gum disease risk with our quick and engaging 6-question assessment!





