Gingivitis vs Periodontitis (What’s the Difference?)

Have you recently visited your dentist and been informed you have gingivitis or gum disease?
What’s shocking is the harmful bacteria that cause these diseases can enter your bloodstream and affect your brain and other organs.
Fortunately, you’re not alone, as almost half (47.2%) of American adults suffer from gum disease.
However, as a dentist, I recommend treating these diseases ASAP to prevent irreversible damage.
Need Dental Advice? It’s FREE!
Recommended Reading: Gingivitis | The Ultimate Guide
Gingivitis vs. Periodontitis (What’s the Difference?)
Gingivitis and periodontitis are severe dental diseases that wreak havoc on your oral health.
Gingivitis consists of gum inflammation caused by harmful bacteria above and below the gum line. In addition, gingivitis is reversible and requires routine dental cleanings and adjunctive services.
In contrast, periodontitis (gum disease) is irreversible and consists of gum inflammation with bone loss.
Gingivitis will commonly precede periodontitis unless the harmful bacteria is removed and eradicated.
Did you know that according to the NIH, periodontal disease is the leading cause of tooth loss in adults?
Teeth are housed in a boney structure that requires health and homeostasis to prevent teeth from shifting. Periodontal disease wages war against healthy gums and bone.
The significant difference between these gum diseases is gingivitis is reversible, whereas periodontal disease is not.
Recommended Reading: What is Gingivitis? Causes, Symptoms & Treatment 2026
What Is Gingivitis?
Gingivitis is inflammation of the gums caused by harmful bacteria.
If your dentist or hygienist does not remove harmful bacteria, the bacteria will congregate and multiply into advanced gum disease. The bacteria that infects the gums lead to swollen, red and puffy gums.
Gingivitis is a common gum issue and a clear warning sign that we must be more proactive about our oral health; however, oral hygiene improvements can help prevent this ailment.
Recommended Reading: 14 Gingivitis Home Remedies That Work! (Dentist Recommended)
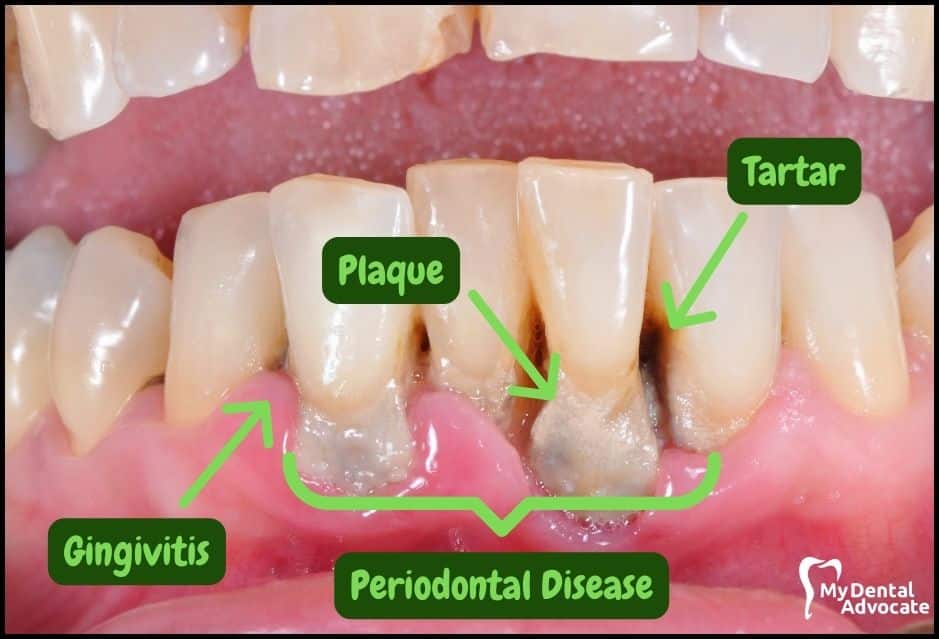
What Is Periodontitis? (Gum Disease)
Periodontitis, also known as periodontal disease, requires immediate action from your dentist or periodontitis.
Below the gumline is home to the most aggressive bacteria in your mouth.
They embed deep into the gum tissue and adhere to the root surface if they’re not removed.
Initially, they assemble into a sticky solution known as plaque, and over time they form “rock-like” crystals known as calculus or tartar.
Bacteria become extremely difficult to remove, similar to a barnacle on the back of a seashell.
The only way to remove this harmful bacteria deep below the gum line is with scaling and root planing treatment.
Our immune system is constantly under attack.
For example, the toxins and poisons produced by the bacteria in plaque overpower our immune response leading to infection, bone loss and gum tissue damage.
Recommended Reading: Is Gingivitis & Gum Disease Contagious? (What the Research Says)
As Crest reports, 24 million Americans have lost 6-plus teeth to decay, or gum disease and 12 million have lost all of their teeth to decay or gum disease.
Causes of Gingivitis & Periodontitis
Harmful bacteria in the mouth infect gum tissue surrounding the tooth.
Soft and hard tissue (bone) become inflamed leading to periodontal disease. When bacteria stay on the teeth for an extended period, they form a sticky film called plaque, which eventually hardens to tartar, also called calculus.
Tartar build-up typically occurs above the gums however it can spread below the gum line, which makes the teeth more challenging to clean. When the bacteria progress below the gum line it invades sensitive space around the teeth.
The bone and gums physically move away from the “harmful agent” (bacteria).
Common Causes
- Poor oral hygiene – If regular brushing and flossing habits are not maintained, dental plaque will form on teeth, causing gum inflammation. However, improved oral hygiene and regular visits to the dentist for routine cleanings aid in the removal of dental plaque. A more severe gum disease (periodontal disease) will occur if left untreated.
- Poor nutrition – Harmful bacteria rely on sugars and carbohydrates to multiply. The bacteria begin to proliferate (increase in number) after it congregates – brushing, flossing and routine cleanings prevent harmful bacteria from forming above and below the gum tissue. Foods high in sugars and carbohydrates are sticky and desirable for oral bacteria.
- Dental plaque – Occurs when food debris is not removed, most commonly along the tooth and gum margin. It may feel a bit “fuzzy” when you run your tongue over it. Dental plaque is composed of bacteria that “eat” sugars. Acid formation and other byproducts form, leading to gum inflammation. To limit dental plaque, brush twice daily and floss nightly.
- Tartar – Plaque that stays on your teeth can harden under your gumline into tartar (calculus), which invites more bacteria formation. Tartar protects plaque from breaking down, creating a protective shield for bacteria. In addition, tartar formation causes gum irritation and inflammation. Unlike plaque, tartar cannot be removed at home and requires a dental cleaning to remove it.
Recommended Reading: 6 Best Mouthwashes for Gingivitis & Gum Disease 2026
Symptoms of Gingivitis vs. Periodontitis
It’s possible to have gingivitis and periodontitis without any symptoms.
However, in mild cases of gingivitis, there may be no discomfort or noticeable symptoms. Often, it remains undetected for quite some time. The symptoms of gingivitis are somewhat non-specific. Additionally, the pink-salmon coloring and stippling in the gum tissue will often disappear.
Also, the gums may appear shiny as the gum tissue becomes inflamed and stretched over the tissue surface.
Gingivitis
- Red & purple gums
- Swollen & puffy gums
- Gum inflammation & discoloration
- Gum separation & recession
- Bleeding gums
- Halitosis (bad breath)
- Tender gums
Periodontitis
- Red & purple gums
- Swollen & puffy gums
- Gum inflammation & discoloration
- Gum separation & recession
- Bleeding gums
- Halitosis (bad breath)
- Tender gums
- Pain when chewing
- Sensitive teeth & gums
- Bone loss
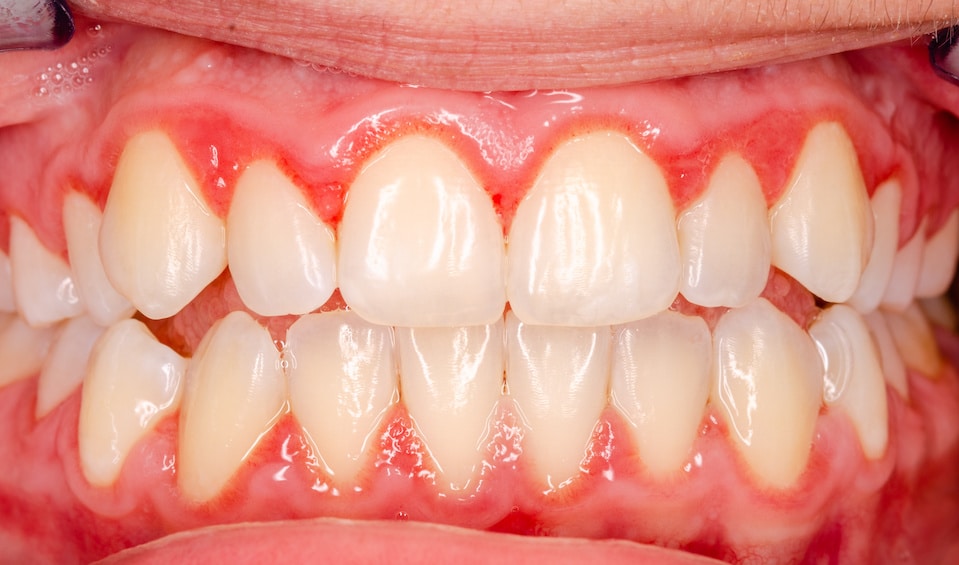
Recommended Reading:Acute Necrotizing Ulcerative Gingivitis (ANUG) “Trench Mouth”
When the gums are swollen, the lining becomes ulcerated, and the gums are prone to bleed even with gentle brushing and flossing.
In addition, if the gums are inflamed, they may start pulling away from the neck of the tooth.
This causes gaps between the teeth and the gums, known as gum pockets (or periodontal pockets).
Similarly, many people aren’t aware that they have gum disease (periodontal disease). Periodontal disease, also known as periodontitis, can cause teeth to shift position, wobble or hurt when you chew.
In addition, periodontal disease will lead to irreversible bone loss.
Recommended Reading: What Does Gingivitis Look Like? (20 Gum Disease Pictures)
Periodontal disease is treated with scaling and root planing, also known as deep cleaning. If gum disease is not controlled, your dentist will refer you to a gum specialist known as a periodontist.
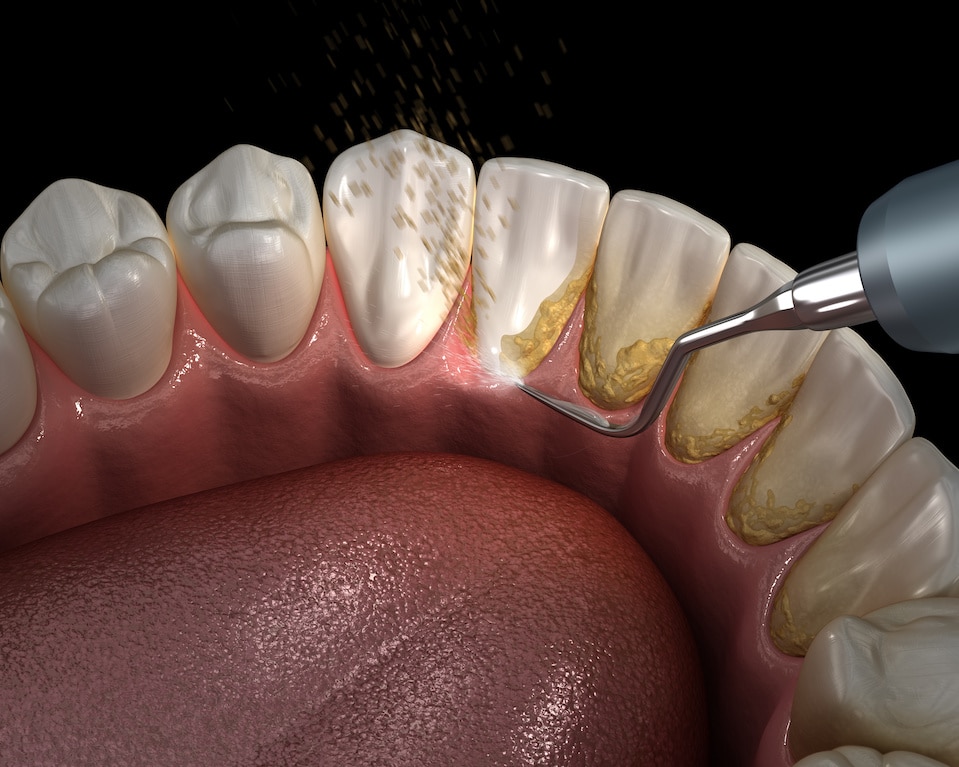
Treatment of Gingivitis vs. Periodontitis
Gingivitis
If you’re diagnosed with gingivitis, don’t panic.
Treatment is standard and includes a prophylaxis dental cleaning by your dentist or dental hygienist.
In addition, oral health improvements are necessary to prevent harmful bacteria from re-seeding on your teeth.
For example, brush twice daily, floss regularly and use mouthwash nightly. Suppose you have braces or more significant gaps between your teeth.
Use a water flosser. I recommend using BURST water flosser because of its portability, large water tank and replacement tips.
Recommended Reading: 5 Best Toothpastes for Gingivitis & Gum Disease 2026
Visit your dentist at least every 6 months for a dental check-up and routine dental cleaning.
Periodontitis
Compared to treating gingivitis, treating periodontitis generally takes more time and expertise.
For example, scaling and root planing are necessary to remove harmful bacteria above and below the gum line.
Adjunctive Procedures
- Chlorhexidine – According to a recent study, chlorhexidine mouth rinse reduces gingivitis. Chlorhexidine can be used in-office and at home (prescription only). However, Chlorhexidine can cause tooth staining if used for an extended period.
- Laser therapy – According to research, low-level laser therapy reduces gingival inflammation. Laser therapy + Chlorhexidine was more effective at removing gum inflammation. Laser therapy is commonly used to treat periodontal disease.
- Fluoride treatment – According to a recent study, stannous fluoride (0.45%) effectively reduced gingival bleeding. However, a more significant reduction is observed if stannous fluoride is used with prophylaxis cleaning.
- Arestin – Arestin (Minocycline HCl) microspheres, in conjunction with scaling and root planing (periodontal treatment), reduces overall pocket depths. This antibiotic is delivered below the gum line to kill the bacteria at the source.
If gum disease is not responding to non-surgical treatments, your dentist may refer you to a periodontist. Periodontists are trained to provide more complex treatments than general dentists, especially for severe cases. Advanced treatment includes bone grafts, tissue grafts and osseous surgery.
Risk Factors (Gingivitis & Periodontitis)
Specific risk factors increase the likelihood of developing gingivitis and periodontitis.
Certain medications, such as antiseizure and immunosuppressants, can lead to gingival hyperplasia (gum overgrowth).
Other Risk Factors
- Smoking or chewing tobacco
- Dry mouth
- Hormones
- Vitamin C deficiency
- Immunosuppressants
- Cardiovascular drugs
- Leukemia & HIV/AIDS
- Suppressed immunity
- Cancer
- Diabetes
- Pregnancy (hormones)
Recommended Reading:Pregnancy Gingivitis: Causes, Symptoms & Treatment 2026
My Experience & Expertise
Gingivitis consists of gum inflammation without the presence of bone loss. However, periodontitis (gum disease) features gum inflection with bone loss.
Gingivitis is reversible, whereas periodontal disease is irreversible. Understanding these significant differences will empower you for improved oral health.
Need a second opinion? We can help! Learn more. Knowledge is power when cultivating healthy dental habits. The more informed you are, the better positioned you’ll be to prevent avoidable and potentially costly dental procedures for you and your family. Watch for future blog posts, where we’ll continue sharing important information, product reviews and practical advice!

About the Author
Dr. Matthew Hannan, also known as “Dr. Advocate,” is a board-certified dentist on a mission to provide accurate dental patient education. He attended Baylor University before completing dental school at UT Health San Antonio School of Dentistry. He now lives in Arizona with his beautiful wife and 4 kids. Dr. Hannan believes everyone should access easy-to-read dental resources with relevant, up-to-date dental research and insight to improve their oral health.

Connect with Dr. Hannan!
-
How to Fix A Cavity
Cavities are a prevalent dental problem that can occur in any teeth – regardless of how well you take care of them. If you have a cavity, don’t worry – plenty of treatment solutions are available, and the cost will vary…
-
BURST Pro Sonic vs. Curve Sonic Electric Toothbrush Review 2026
In the dynamic world of dental hygiene, electric toothbrushes have evolved to offer more than just a standard clean. Among the top contenders in the market are BURST’s Pro Sonic and the Curve Sonic Electric Toothbrush. Deciding between these two can be challenging with varying features tailored to specific dental needs. This review dives deep into the features, benefits, and unique qualities of each, providing clarity to users and dental professionals alike.
-
What Is Magic Mouthwash?
Experiencing mouth sores, ulcers, or other oral irritations can be painful and distressing, impacting your daily life and challenging even simple tasks like eating, drinking, or speaking.
Gain Clarity with Our FREE Second Opinion Guide
FREE online second opinion within 48 hours. No joke!
Product Reviews
Our 300+ dental product reviews (and counting), curated by an experienced dentist, are the most comprehensive online.
Toothbrush Genie
State-of-the-art chatbot designed to help you discover your perfect toothbrush in just a few simple steps!
Cavity Risk Assessment
Cutting-edge digital tool designed to evaluate your individual cavity risk based on your responses to a series of questions.
Gum Disease Assessment
Discover your gum disease risk with our quick and engaging 6-question assessment!





