Impacted Wisdom Teeth (Managing Symptoms)
Are you suffering from impacted wisdom teeth? If yes, then you should read this article.
This condition is quite common and affects millions of people worldwide. Around 90% of us have at least one impacted wisdom tooth.
Understanding what’s involved with third molar removal and recovery will aid your healing after surgery.
Recommended Reading: Wisdom Teeth | The Ultimate Guide
What Are Impacted Wisdom Teeth?
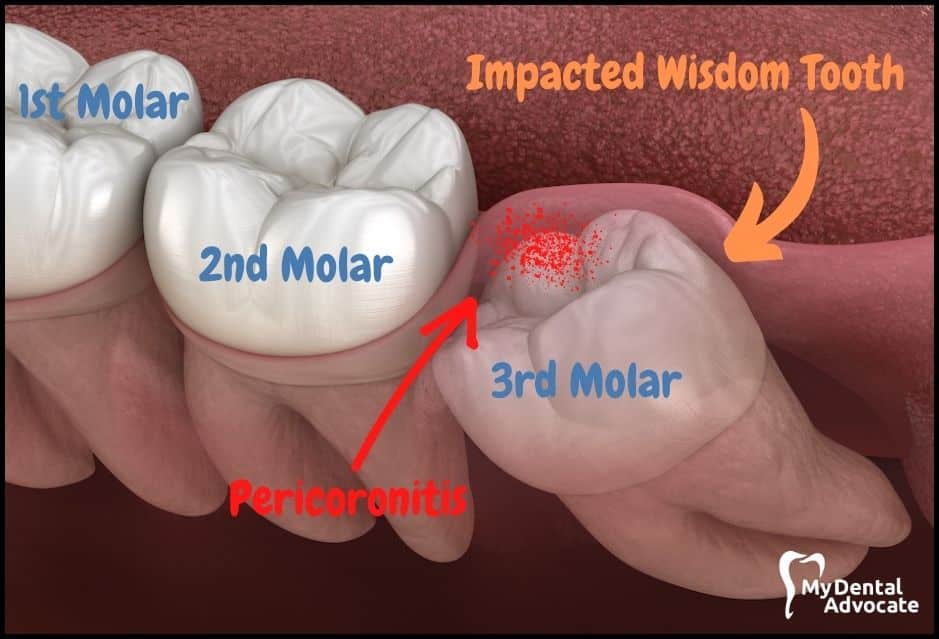
Impacted wisdom teeth occur when the third molar (wisdom tooth) fails to erupt into its proper position.
Need Dental Advice? It’s FREE!
The result is that the tooth gets stuck within the gums and jawbone. As time passes, the pressure caused by the growing bone and tooth pushes the tooth further down, causing pain and discomfort.
In addition, an impacted wisdom tooth may be partially visible (partially impacted) or never break through the gum line (fully impacted).
Wisdom teeth erupt between the ages of 15 and 25. Some people have no issues during this process, whereas others experience pain and discomfort. In addition, lack of adequate space is the most common reason tooth impaction occurs.
Impacted wisdom teeth can cause serious complications such as infection, abscesses, cysts, swelling, and even nerve damage. They also increase the risk of developing dental problems later in life.
Therefore, it is crucial to remove them as soon as possible.
Recommended Reading: 101 Foods to Eat After Dental Surgery, Implants or Wisdom Teeth Removal
Impacted Wisdom Teeth Symptoms
Impacted wisdom teeth can lead to many symptoms, including pain and swelling.
You must inform your dentist if you have any of the symptoms below. Early intervention offers the best chances of treatment success, so don’t put it off.
Sometimes unerupted wisdom teeth will have no symptoms and will be discovered by your dentist or orthodontist after a panoramic x-ray.

Common Symptoms
- Pain or swelling of your jaw or face
- Red, swollen or bleeding gums
- Unpleasant taste
- Bad breath (halitosis)
- Difficulty opening your mouth
- Jaw pain
- Earache or headache
- Fever
Recommended Reading: Wisdom Teeth Pain: Symptoms, Relief & Home Remedies (Helpful Tips)
What Causes Impacted Wisdom Teeth?
The causes of impacted wisdom teeth are variable.
However, the most common reason is due to lack of adequate space in the mouth. The second molar is the last visible tooth before the wisdom tooth erupts.
Therefore, people with small mouths won’t have enough room for the third molar to erupt, leading to tooth impaction.
Common Causes
- Limited Space: Wisdom teeth often lack room to emerge properly, especially in people with smaller statures or mouths.
- Tooth Angulation: Improperly angled teeth, like mesial impactions pointing towards the second molar, can block proper eruption.
- Genetics: Genetics influence tooth impaction. If your family has a history of missing wisdom teeth, you’re likely to experience the same.
Soft vs. Hard Tissue Impaction
Soft and hard tissue impaction classifications dictate how difficult wisdom tooth removal will be.
In addition, wisdom teeth can be impacted by the gums or the bone. Understanding the difference between them will help you better understand the surgical procedure.
- Soft Tissue Impaction: The wisdom tooth emerges through the bone but not the gum. It’s less invasive to extract than hard tissue impaction, often hindered by bone, tooth position, or the second molar.
- Hard Tissue Impaction: The tooth is completely encased in bone, making it the most common and invasive type. It’s classified as partial or complete bony impaction, requiring bone removal and tooth sectioning for extraction.
After the removal of impacted wisdom teeth, a large void in the bone will be left behind the second molar.
As a dentist, I recommend placing bone graft material in the tooth socket after the extraction if an inadequate amount of bone is left to support the second molar. Discuss bone graft options with your oral surgeon before treatment.
Bone graft is vital to replace lost bone after impacted wisdom teeth extractions.
Partial vs. Complete Bony Impaction
If the wisdom tooth is considered a hard tissue impaction, it’s further classified into partial or complete bony based on much bone is still covering the wisdom tooth.
For example, if the impacted wisdom tooth has broken through the bone level, it’s considered partial bony. However, if the bone fully encapsulates the wisdom tooth, it’s considered complete bony.
- Partial Bony Impaction: Here, part of the wisdom tooth is above the bone but under the gum. Removal might involve cutting the tooth into pieces.
- Complete Bony Impaction: The wisdom tooth is fully trapped, either by its angle or being encased in bone. This type is challenging to remove, often requiring significant bone removal and tooth sectioning.
Impacted Wisdom Teeth Classifications
Bony and tissue impaction isn’t the only method to classify impacted wisdom teeth.
Four types of impacted wisdom teeth classifications involve the positioning of the tooth. The type of impaction is vital for the surgeon to analyze on the panoramic x-ray before surgery.
Classifications
- Mesial Impaction: The most common type, where the wisdom tooth angles towards the front of your mouth.
- Distal Impaction: A rare form, with the wisdom tooth angled towards the back of your mouth.
- Vertical Impaction: The tooth is correctly positioned but trapped under the gums, often stuck under the second molar’s crown.
- Horizontal Impaction: The tooth lies sideways under the gums, causing pain by pressing on adjacent teeth and posing surgical removal challenges.
Why do Impacted Wisdom Teeth Need to be Removed?
Removing impacted wisdom teeth when you are younger (15 to 25) is crucial because you will heal quicker and recover faster, and the bone is thin.
In addition, removing wisdom teeth before they are fully grown allows for easier access and extraction for the oral surgeon.
Also, it will be challenging to brush and floss wisdom teeth to prevent cavity-causing bacteria from forming.
Untreated, impacted wisdom teeth will harbor harmful bacteria. Oral bacteria can travel from your mouth through the gum tissue and into the bloodstream leading to systemic infections affecting the heart, kidneys, and other organs.
Diabetes, heart disease, and kidney disease are common systemic health conditions associated with oral bacteria invasion. In addition, problems can occur when the roots are fully grown and cause difficulties for the oral surgeon during the procedure.
Problems Associated with Impacted Wisdom Teeth
- Risk of Infection: Inadequate space for wisdom teeth can lead to gum irritation, pain, and infection (pericoronitis), especially in smokers. A study found 72.4% of 20-25-year-olds experienced pericoronitis before removal.
- Crowding: There’s debate about wisdom teeth causing crowding. While they might contribute, other factors like gum health and tooth size also play a role.
- Tooth Decay: Crooked wisdom teeth are hard to clean, promoting bacteria growth and deep cavities that are tough to treat.
- Cyst Formation: Impacted wisdom teeth can lead to jaw cysts, damaging nearby teeth, gums, and bone, and potentially affecting nerves and blood vessels.
- Damage to Adjacent Teeth: Wisdom teeth growing towards other teeth can cause tooth resorption, damaging both teeth and often requiring extraction.
- Bone Loss/Periodontal Disease: Impacted wisdom teeth can lead to bone loss around adjacent teeth, sometimes necessitating removal if bone support is insufficient.
Studies have found that periodontal disease in expectant mothers may be associated with a greater likelihood of preterm and low birthrate babies.
Impacted Wisdom Tooth Removal
Impacted wisdom teeth are removed while the patient is sedated. On the day of your surgery, it’s essential that you don’t eat or drink 8 hours before the procedure.
However, the dentist will advise you to take the medication you generally take (unless it interferes with the procedure – your surgeon will discuss this with you).
Recommended Reading: Sedation Options for Wisdom Teeth Removal (Read this FIRST)
Generally, wisdom teeth can be extracted with little to no pain, and the procedure will take 30-60 minutes to complete. Plan accordingly, as you and your driver will be in the office for approximately 90 minutes.
Wisdom teeth extractions are considered an outpatient procedure, so you will be able to go home afterward.
Recommended Reading: Wisdom Teeth Removal (What’s Involved?)
Procedure Steps
- Anesthesia/Sedation: An oral surgeon or anesthesiologist administers anesthesia, typically general anesthesia for “sleep” during the procedure. Your vitals like blood pressure and heart rate are monitored.
- Local Anesthesia: Numbs your teeth area. Dental assistants will support your head and neck during the procedure.
- Incision: A cut is made behind the second molars for access to the wisdom teeth and bone.
- Bone Removal: Surgical tools remove bone around the tooth, carefully avoiding nerves and vital structures.
- Tooth Sectioning: The wisdom tooth is split into pieces for easier removal in the tight space.
- Extraction: The tooth is gently rocked and removed.
- Cleaning the Socket: The area is rinsed with sterile saline to clear any debris.
- Stitches: Sutures are placed to help form a blood clot and protect the area. These dissolve in 3-5 days.
- Recovery from Anesthesia: Medication is given to reverse anesthesia. You’ll be sleepy, so rest is important.
- Gauze Packs: These are applied to aid blood clot formation and should be kept in place for 30-60 minutes.
Common Complications After Wisdom Tooth Removal
Although every effort is made to minimize complications, 4.3% to 9.1% of cases result in some degree of complications.
According to a recent study, the most frequent complication was alveolar osteitis (dry socket), occurring in 3.9% of cases.
The second most common complication in 1.5% of cases was a post-operative temporary or permanent sensation disorder.
Managing post-operative complications becomes more challenging if immediate care is not taken. When in doubt, call your dentist if you have any questions or concerns.
Managing Surgical Complications
- Dry Socket: Commonly occurs when a blood clot dislodges, exposing bone, causing severe pain around days 3-4. Treatment includes special paste or saline irrigation to form a new clot.
- Numbness (Paresthesia): Can result from damage to the nerve near lower wisdom teeth, occurring in 0.35% to 8.4% of cases.
- Excessive Bleeding: Normal up to 24 hours post-surgery, but if it continues, contact your dentist. Those on blood thinners may be more prone to this.
- Adjacent Teeth Damage: Force used during surgery might harm nearby teeth, like crowns or fillings. Most such damages are fixable by your dentist.
- TMJ Issues: Surgery might stretch the TMJ, leading to temporary clicking or popping. If there’s no pain, it’s usually not a concern.
- Jaw Muscle Strain: The jaw muscles are stretched during the procedure, causing soreness or stiffness for 1-2 weeks. Use cold compresses initially, then alternate with warm packs. Limited jaw opening post-surgery is common.
- Swelling & Infection: Swelling and bruising are typical, but signs of infection like fever need immediate attention. Use over-the-counter anti-inflammatories for pain and inflammation.
- Nutrition and Recovery: Stay hydrated and eat a soft diet rich in carbs, protein, and vitamins (like mac & cheese, applesauce, protein shakes). Proper nutrition and sleep are crucial for healing.
Methods to Recover Faster
Wisdom teeth removal is a standard outpatient procedure for patients between 15 and 25.
Recovery after wisdom teeth removal takes 3-4 days, but symptoms can take 1-2 weeks to subside.
Your oral surgeon will provide detailed post-op instructions, including contact information. In addition, you must follow the at-home care instructions that your surgeon gives you to prevent complications and improve healing.
Recommended Reading: What to Eat After Wisdom Teeth Removal? (BEST & WORST Foods)
Your mouth is designed for optimal healing and regeneration; however, expect the tooth socket to heal completely in 3-6 months.
Recommendations
- Take prescribed medication before the local anesthesia wears off
- Rest and recover for the first 3-4 days to allow the mouth to heal
- Avoid sucking, spitting, smoking or vigorously swishing to prevent dry socket.
- Use cold compress up to 36 hours after surgery to reduce inflammation, pain and swelling
- Alternate between hot and cold packs after that to stimulate healing
- Gently rinse mouth out with warm salt water 2-3x/day
- Gently massage TMJ and jaw muscles to decrease soreness
- Keep head elevated up to 72 hours after surgery to minimize pain and swelling
- Sleep often and stay off of your feet
- Avoid physical activity for 3-4 days
- Consume adequate amounts of fluid and electrolytes (Gatorade)
- Consume sufficient amounts of nutrients (soft-food diet)
My Experience & Expertise
Wisdom teeth extractions can be a daunting experience, especially if they are impacted.
Patient education is key to understanding what’s involved and how to recover faster. Take it easy after surgery and give yourself plenty of time to heal.
Need a second opinion? We can help! Learn more. Knowledge is power when cultivating healthy dental habits. The more informed you are, the better positioned you’ll be to prevent avoidable and potentially costly dental procedures for you and your family. Watch for future blog posts, where we’ll continue sharing important information, product reviews and practical advice!

About the Author
Dr. Matthew Hannan is a board-certified dentist on a mission to provide accurate dental patient education. He attended Baylor University before completing dental school at UT Health San Antonio School of Dentistry. He now lives in Arizona with his beautiful wife and 4 kids. Dr. Hannan believes everyone should access easy-to-read dental resources with relevant, up-to-date dental research and insight to improve their oral health.

Connect with Dr. Hannan!
-
Braces Cause Teeth Stains? (How to Prevent Them)
As a dentist, one of the most common concerns that patients have is the appearance of their teeth. While braces can help straighten teeth and improve their alignment, they can also cause teeth stains that can be difficult to remove…
-
Best Mouthwash for Ulcers (Full Review)
Mouth ulcers can be a real pain, literally and metaphorically. They interfere with your ability to eat, drink, and even talk comfortably. When dealing with this pesky oral issue, choosing the right mouthwash can make a world of difference.
-
Preventing Dental Misdiagnosis (Identifying Common Errors)
Dental misdiagnosis can significantly impact your oral health and overall well-being. It occurs when a dental professional incorrectly identifies a dental condition or fails to diagnose a condition altogether. This misstep can lead to inappropriate or delayed treatment, causing further complications or even the development of new issues.
Gain Clarity with Our FREE Second Opinion Guide
FREE online second opinion within 48 hours. No joke!
Product Reviews
Our 300+ dental product reviews (and counting), curated by an experienced dentist, are the most comprehensive online.
Toothbrush Genie
State-of-the-art chatbot designed to help you discover your perfect toothbrush in just a few simple steps!
Cavity Risk Assessment
Cutting-edge digital tool designed to evaluate your individual cavity risk based on your responses to a series of questions.
Gum Disease Assessment
Discover your gum disease risk with our quick and engaging 6-question assessment!






