Wisdom Teeth Removal Sedation Options

Wisdom teeth removal can be intimidating, especially if you’ve never been sedated.
With many anesthesia options available, how do you know what method is best?
Understanding the differences between each option will empower you to make a wise choice so you are comfortable on the day of the surgery.
Recommended Reading: Wisdom Teeth | The Ultimate Guide
Need Dental Advice? It’s FREE!
What Is Dental Sedation?
Sedation is a form of anesthesia and is often used interchangeably.
Sedation dentistry involves an anesthetic, gas or drug used to alter mental awareness. Sedation is commonly classified into three categories mild (minimal), moderate and heavy (deep).
Each category depicts how “asleep” you will be during the procedure.
Sedation dentistry is a great way to alleviate stress and anxiety during the procedure.
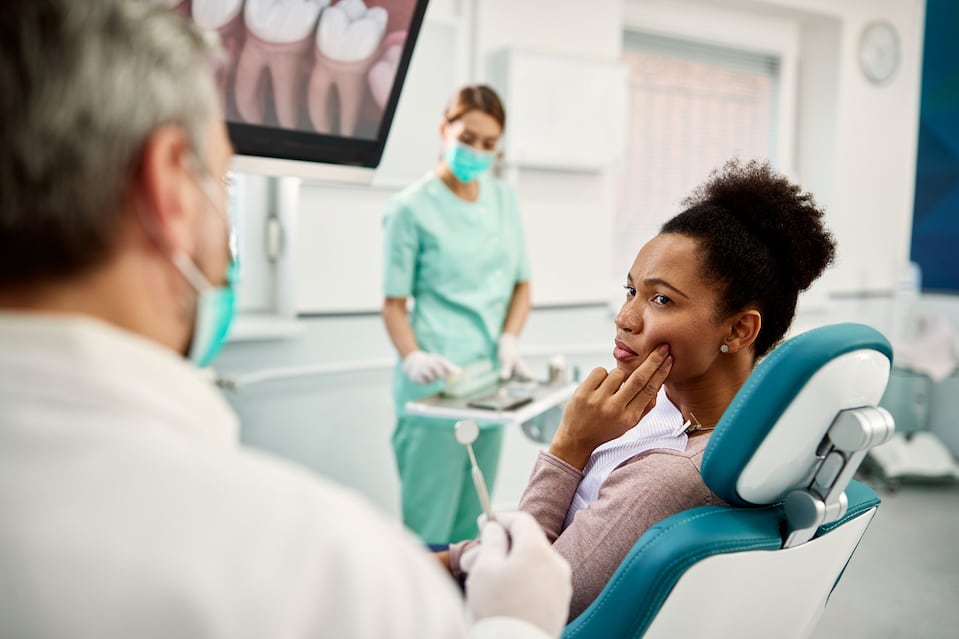
Many patients dread the dentist, let alone having their wisdom teeth extracted. Sedation dentistry is a great solution.
If the patient is comfortable, the dentist can be efficient and timely, making it a win-win for the patient and clinician.
The type of dental sedative depends on the patient’s and the dentist’s specific needs.
The dentist will inquire about the patient’s comfort level and review their medical history to confirm sedation is safe for the patient.
For example, the dentist will check if the patient has had any adverse reactions to anesthesia or if the patient takes any medications that may interfere with the anesthesia.
Sedation Dentistry Considerations
- Patient’s anxiety level
- Procedure length
- Treatment plan
- Medical history
- Clinicians sedation expertise
Recommended Reading: Wisdom Teeth Removal (What’s Involved?)
Is Sedation Dentistry Safe?
Millions of dental patients are safely treated each year using sedation dentistry treatments.
However, it’s important to remember that all types of sedation come with a slight level of risk.
Therefore, the American Dental Association urges patients to always take an active role in their oral healthcare, including discussing questions and concerns with their dentist and oral surgeon before the procedure.
Sedation dentistry is typically very safe if you are healthy and treated by a professionally trained dentist or oral surgeon.
Anesthesia complications commonly occur if the patient is obese, struggles with sleep apnea or has cardiovascular (lung or heart) issues. Consult with your primary care doctor (PCP) to better understand any risk of complications.
Although rare, death can occur during dental anesthesia.
According to a recent study, 3 deaths occur per 1,000,000 persons based on research from 20 studies dating back to 1955. Hypoxia (lack of oxygen) was the most common cause of death.
Therefore, case selection is essential regarding a patient’s general health status to diminish the risk of death.

Sedation Dentistry Considerations
- Confirm that your dentist/oral surgeon is qualified
- Review medical/dental history with your clinician
- Ask questions & clarify concerns
- Understand the risks of sedation
- Confirm your clinician will monitor your vitals
Recommended Reading: Wisdom Teeth Removal Cost 2026 (With & Without Insurance)
Is Dental Sedation Necessary for Wisdom Teeth Extractions?
Dental sedation is strongly advised for most patient as it allows the patient to be comfortable, and the clinician can work efficiently without distractions.
In addition, sedation dentistry is safer for the patient’s health.
Without sedation, the patient could move unexpectedly or become stressed, leaving the dentist unable to complete the procedure as planned. In addition, a stress response could dangerously increase blood pressure and induce a stroke or heart attack.
Did you know that wisdom teeth can be extracted without sedation? For example, erupted wisdom teeth may only require local anesthesia as the extraction is less invasive.
Local anesthesia is used to numb the area of the mouth that will be affected by the procedure. Keep in mind that a patient that is fully aware and awake during the procedure runs a higher risk of experiencing anxiety or discomfort while the wisdom teeth are extracted.
Recommended Reading: Impacted Wisdom Teeth: Symptoms, Causes, Removal & Recovery
Talk to your dentist or oral surgeon before the procedure to discuss how complicated your surgery will be.
In addition, consider your own anxiety level and personal coping mechanisms during dental work. Your clinician can use this knowledge and professional experience to determine the necessary sedation level.
Before making any decision, all sedation methods should be discussed with your dental professional to fully understand the risks of each technique and the side effects you may experience from the sedation.
Levels of Sedation Dentistry
Several medications are available to patients, making them comfortable and relaxed during the procedure.
While some medicines are used to reduce pain, others are used to relax the patient. In addition, some drugs induce a light “twilight” sleep while others induce deep sleep.
The patient and the dentist should consider all factors when deciding the best sedation option.
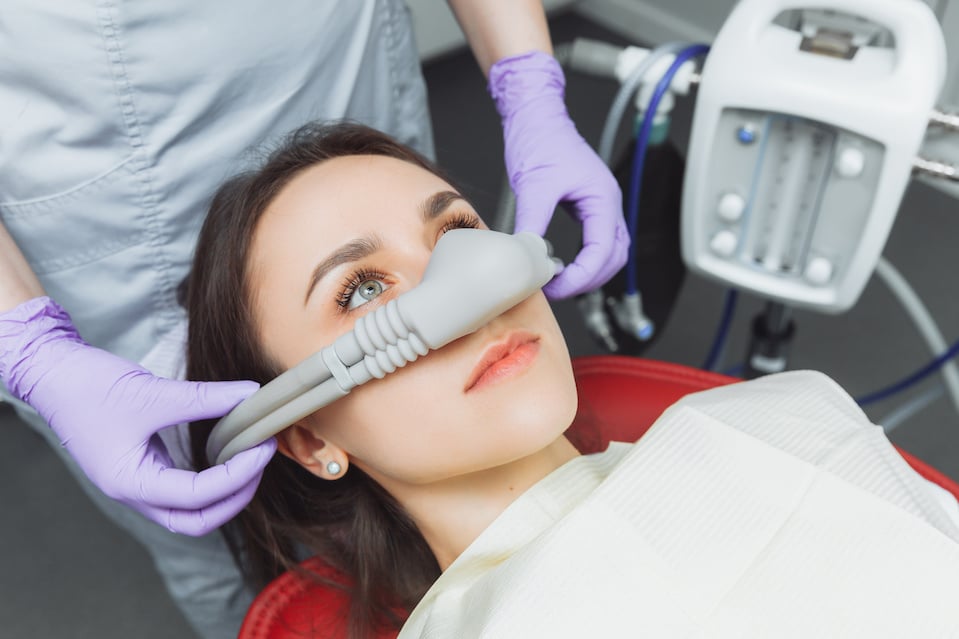
Minimal Sedation
Your dentist may recommend minimal sedation, such as nitrous oxide (laughing gas), to help you relax during the procedure.
This tasteless and colorless gas is administered through a tight-fitting mask that fits over your nose.
Immediately after inhaling the gas, you’ll feel relaxed and comfortable. Laughing gas enters and exits your system quickly and safely.
Nitrous oxide is considered safe and effective for minimal sedation; however, some potential side effects are associated with nitrous oxide use.
For example, nausea, vomiting, dizziness, drowsiness, headache, dry mouth, difficulty breathing, and fatigue can occur.
After the procedure, the clinician will have you inhale 100% oxygen for 5-10 minutes to regain your senses. Tell your dentist or physician immediately if you experience any symptoms during minimal sedation.
Moderate/Deep Sedation
Moderate or deep sedation can be achieved using IV or oral medication.
IV sedation involves using intravenously administered medication to induce a “twilight” state between waking and sleeping awareness. You’ll be able to respond to questions, but you won’t feel any discomfort and will have no recollection of what happened during the procedure.
Conscious sedation involves taking medication 30-60 minutes before the procedure when you arrive at the office. Conscious sedation is effective.
However, it’s more challenging to regulate the sedation as it’s digested into your stomach.
During moderate sedation, you may hear voices, see images, feel pressure or vibrations, smell odors, taste flavors, or even feel sensations like warmth or coldness.
You may also hear sounds such as music or laughter. Although it’s possible to fall asleep during moderate sedation, it’s unlikely, and the clinician will monitor your vitals.
The level of sedation you receive depends on how much medicine is needed to achieve the desired effect.
If too little medicine is injected, you could wake up feeling groggy or disoriented. Too much medicine could cause drowsiness or dizziness. Depending on your specific needs, you may receive one or more injections containing sedatives and analgesics (pain medication).
General Anesthesia
General anesthesia involves using IV medications to induce deep sleep.
This level of sedation is used to treat people suffering from severe anxiety and depression or for more invasive procedures. Patients receiving general anesthesia will “fall asleep” during the procedure.
As a result, they will not remember anything about the procedure and will wake up feeling refreshed and calm.
During general anesthesia, your gag reflex is eliminated, so your clinician will be sure to keep your airway clear so you can breathe and monitor your vitals.
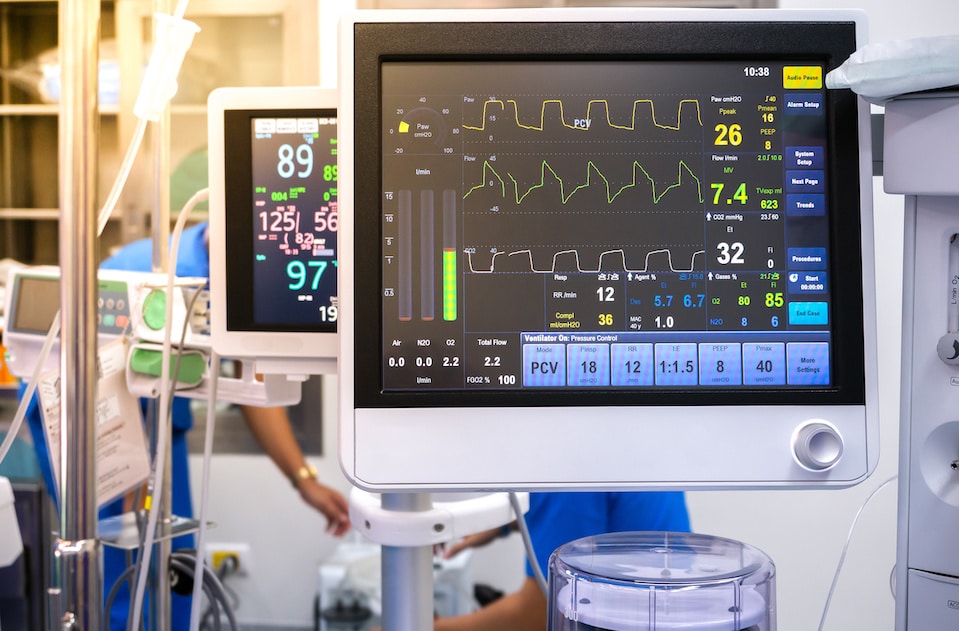
Sedation Dentistry Methods
According to a study in the Journal of Dental Hygiene, approximately 19% of people report moderate to high dental anxiety.
This statistic aligns with previous research, which suggests that 10-20% of adults suffer severe anxiety during routine dental procedures.
In comparison, 50-80% of patients report mild anxiety.
The consequences of dental anxiety are far-ranging and have real effects. For example, 9-15% of anxious patients avoid seeking dental care, including wisdom tooth extractions — which can lead to long-term dental and health issues.
So let’s take a closer look at the different sedation options.
Local Anesthesia
Local anesthesia is the most commonly used sedative.
Although it doesn’t alter the mental state, it eliminates the pain response. The most common local anesthetic medication is Lidocaine (Xylocaine); however, others include Carbocaine (Mepivacaine) and Marcaine (Bupivacaine).
The drug is injected into the target area to temporarily prevent nerves from transmitting pain. Local anesthetic can eliminate pain on its own, but it is also frequently used in conjunction with other sedation techniques to reduce cognitive awareness during the procedure.
Laughing Gas (Nitrous Oxide)
Laughing gas (nitrous oxide) is an odorless gas administered through a mask, which the dentist places over the patient’s nose. It’s considered a minimal sedative, and the clinician can adjust the dosage of the laughing gas according to the patient’s needs.
Laughing gas and oxygen flow simultaneously in varying amounts depending on the dosage. It makes the patient feel happy and cheerful. The effects wear off quickly, so patients don’t need someone to drive them home.
In addition, laughing gas is affordable, effective and safe to use.
Recommended Reading: 101 Foods to Eat After Dental Surgery, Implants or Wisdom Teeth Removal
Conscious sedation
This type of sedation ranges from minimal to moderate. Conscious sedation is taken by pill (Valium, Halcion, Ativan, etc.) 30-60 minutes before the appointment. The effectiveness of the medication is variable, so patients will need someone to drive them home after the procedure.
A handful of patients become groggy and fall asleep during the procedure but they can be woken up with a gentle shrug.
In addition, The clinician will monitor your vitals, so you are not overly sedated during the wisdom tooth extraction. Conscious sedation is more effective than laughing gas but less desirable than IV sedation because the effectiveness is unpredictable.
IV Sedation
IV sedation is the most effective option for moderate to deep sedation.
Sometimes referred to as “twilight sedation,” IV sedation reduces the patient’s awareness level and anxiety. Although patients are technically awake, most report that they “slept through the procedure.”
Patients are relaxed and comfortable during the treatment and wake up with no recollection of the surgical procedure. IV sedation is administered intravenously and is predictable and controllable.
IV sedation is an excellent solution for lengthy, complicated procedures such as multiple wisdom teeth extractions.
After the procedure, patients will need someone to drive them home as it takes a while to regain their senses. In addition, you will need to fast for 8 hours before the procedure.
General Anesthesia
As the deepest level of sedation, general anesthesia will induce “deep sleep.”
Like IV sedation, you will be required to fast 8 hours before the procedure. In addition, your vitals will be monitored, and oxygen will be administered during the process.
You will have no recollection of the treatment and will not respond to any questions or stimulation during the procedure.
Naloxone is commonly used to reverse the effects of general anesthesia after the procedure is completed.
General anesthesia is preferred for individuals with severe anxiety as the clinician can work efficiently without distractions, and the patient wakes up without memory of the dental procedure.
Sedation Dentistry Expectations
Before the procedure, you can expect a thorough medical and dental evaluation.
In addition, before sedation is administered, the clinician will inform you if you need to fast before the procedure. Next, your dental team will discuss the recovery process and ensure you have somebody present to drive you home afterward.
Mild sedation, such as local anesthesia and laughing gas (nitrous oxide), do not require a designated driver.
If you have complex medical issues, you may need a medical clearance from your physician before the procedure. For example, your primary care physician may want to be aware if you have a condition such as hypertension, heart disease, high blood pressure, or diabetes.
My Experience & Expertise
I strongly recommend sedation during wisdom teeth removal because it protects your health, calms your body and allows the clinician to work without distractions.
Understanding the best sedation method is key to a safe and successful procedure. Talk to your clinician if you have any questions or concerns.
Need a second opinion? We can help! Learn more. Knowledge is power when cultivating healthy dental habits. The more informed you are, the better positioned you’ll be to prevent avoidable and potentially costly dental procedures for you and your family. Watch for future blog posts, where we’ll continue sharing important information, product reviews and practical advice!

About the Author
Dr. Matthew Hannan, also known as “Dr. Advocate,” is a board-certified dentist on a mission to provide accurate dental patient education. He attended Baylor University before completing dental school at UT Health San Antonio School of Dentistry. He now lives in Arizona with his beautiful wife and 4 kids. Dr. Hannan believes everyone should access easy-to-read dental resources with relevant, up-to-date dental research and insight to improve their oral health.

Connect with Dr. Hannan!
-
Prescription Fluoride Toothpaste (Expert Advice)
Whether or not you should use prescription fluoride toothpaste depends on your cavity-risk potential and the determination by your dentist. For example, if you are at high risk for tooth decay, have sensitive teeth…
-
Sonicare 5100 vs. 6100 Electric Toothbrush (Full Review)
Brushing your teeth is a daily ritual you can’t overlook, but all toothbrushes are not created equal. If you’re in the market for an electric toothbrush that elevates your oral care routine, you’ve probably heard of Philips Sonicare’s two titans: the 5100 and the 6100.
-
Gingivitis vs Healthy Gums
You may have gingivitis and not even know it! Harmful bacteria that cause gingivitis can progress into severe gum disease or creep into your bloodstream (yuck!). Most patients with gingivitis or gum disease are unaware because…
Gain Clarity with Our FREE Second Opinion Guide
FREE online second opinion within 48 hours. No joke!
Product Reviews
Our 300+ dental product reviews (and counting), curated by an experienced dentist, are the most comprehensive online.
Toothbrush Genie
State-of-the-art chatbot designed to help you discover your perfect toothbrush in just a few simple steps!
Cavity Risk Assessment
Cutting-edge digital tool designed to evaluate your individual cavity risk based on your responses to a series of questions.
Gum Disease Assessment
Discover your gum disease risk with our quick and engaging 6-question assessment!