What Does a Cavity Look Like? (20 Pictures)
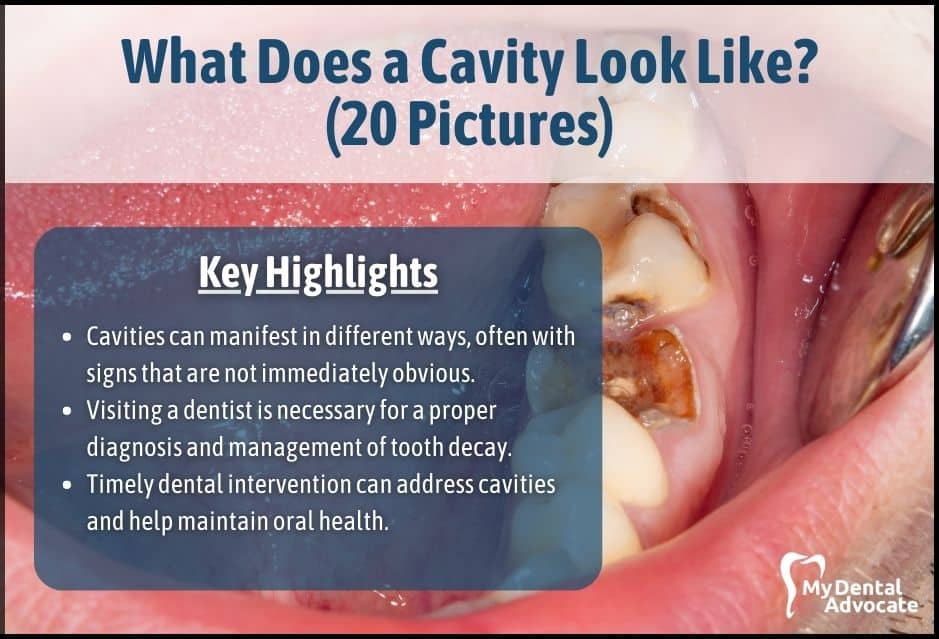
Understanding cavities might seem straightforward, but there’s a lot more to them than meets the eye.
Cavities vary in appearance and aren’t always as simple as a dark spot on a tooth or an obvious hole.
Indeed, tooth decay has many faces, sometimes showing more subtle signs that aren’t as easy to recognize. Knowing when to suspect a cavity is key.
Key Highlights
- Cavities can manifest in different ways, often with signs that are not immediately obvious.
- Visiting a dentist is necessary for a proper diagnosis and management of tooth decay.
- Timely dental intervention can address cavities and help maintain oral health.
Recommended Reading: Cavities | The Ultimate Guide
Need Dental Advice? It’s FREE!
What Is Tooth Decay
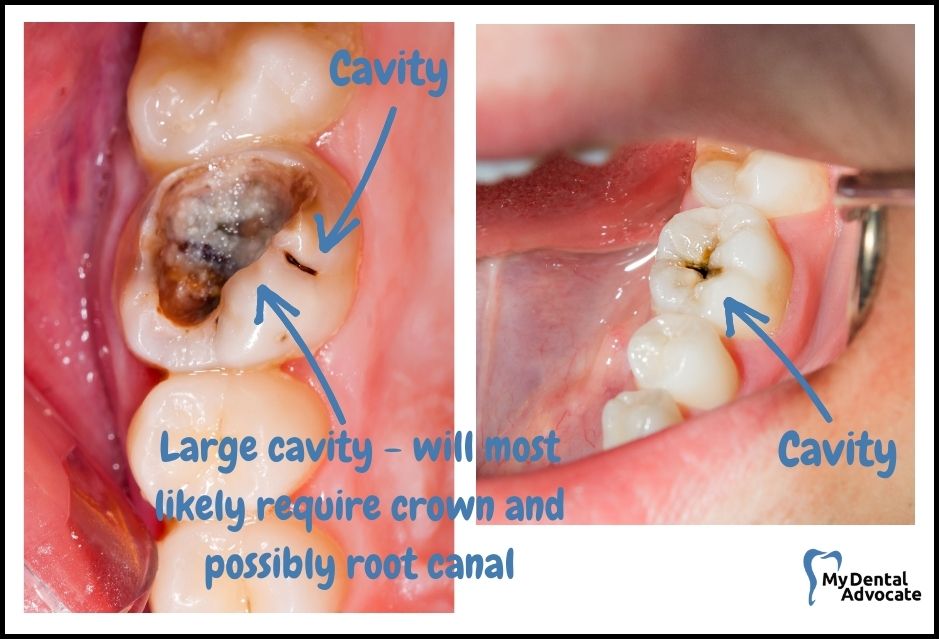
When you inspect your teeth, you may spot a cavity as a dark yellow, brown or even black dot or fissure.
These cavities frequently develop on your molars’ biting surfaces, near the gums, or nestled between teeth, though they can appear on any part of a tooth.
Here’s how to identify the different stages of tooth decay:
- Early Enamel Weakening: You might notice a frosted or white spot, typically along the gumline where plaque accumulates.
- Before the Hole Forms: As decay progresses deeper into the enamel, the surface remains intact. At this stage, using higher fluoride treatments might repair the damage.
- Established Decay: Once the decay reaches the dentin beneath the enamel, a cavity forms. Treatment such as fillings or crowns usually becomes necessary at this point.
Regular dental check-ups are essential for catching these early signs and preventing the progression of decay. Remember, early intervention might save the tooth without the need for more extensive treatments.
Identifying Early Tooth Decay
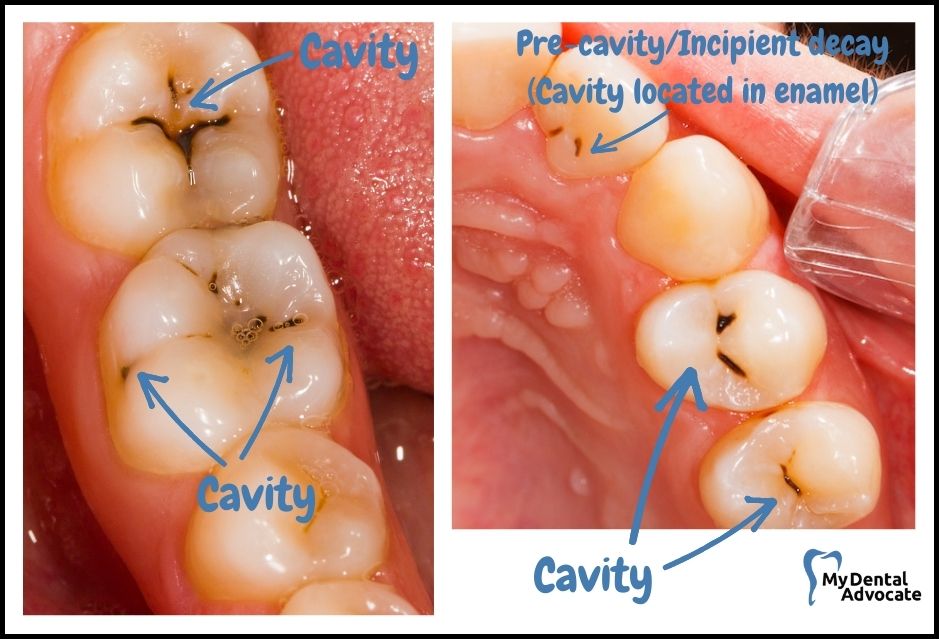
Early stages of tooth decay, not yet full-blown cavities, may present as a white or frosty-looking discoloration near your gum line.
This is due to the acids from bacteria attacking the enamel, causing a loss of minerals—a process known as demineralization.
If this early decay is not addressed, the outer layer may give way to more significant damage. Keep an eye out for these subtle changes in enamel to catch decay before it progresses.
Signs of Initial Tooth Decay
- Your tooth may exhibit a frosty or chalky appearance when decay is starting.
- Look out for light brown or dark yellow spots, a sign that the decay is progressing.
- When decay advances, areas may darken due to food stains.
- A sense of softness or stickiness on the tooth indicates deeper damage into the dentin.
Recommended Reading: What Is a Cavity? What Causes Rotten Teeth?
Signs of Cavities on Anterior Teeth
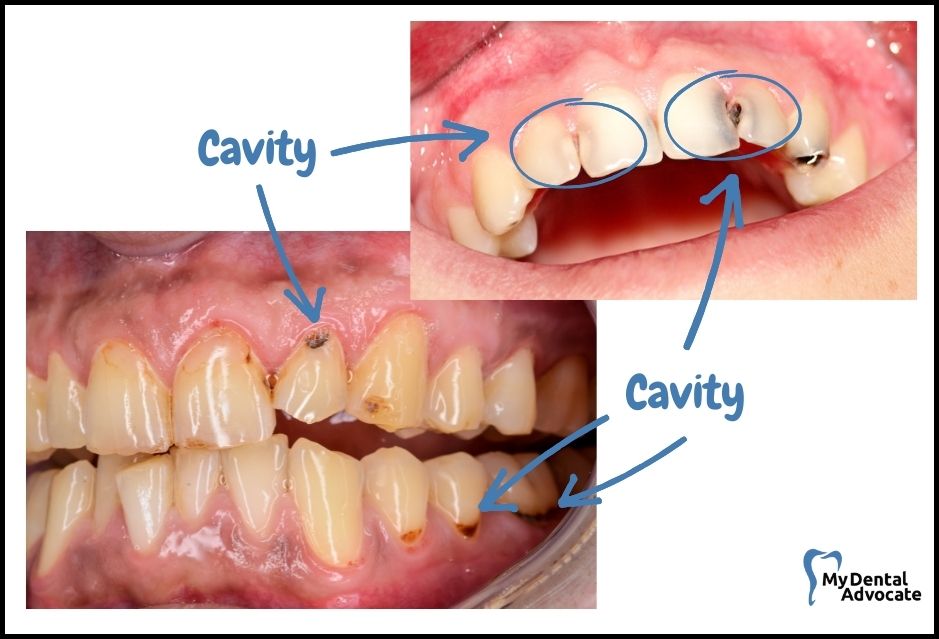
When examining your front teeth, you may notice:
- A grayish shadow below the enamel, possibly signifying a cavity between teeth.
- White spots on the surface indicate early enamel demineralization.
- As the condition progresses, spots may darken to yellow or light brown.
- Without intervention, a deeper cavity might reach the nerve, necessitating a root canal treatment.
Remember that early detection can save you from more complicated procedures.
Recommended Reading: Can You Reverse a Cavity? (5 Simple Steps)
Identifying Cavities in Molars
Cavities nestled between molars can manifest as dark areas. The robust enamel of your rear teeth means visible signs only emerge once the decay advances significantly.
When a cavity grows, it can lead to chipping as the enamel weakens from the decay’s interior expansion.
If you have any suspicions that you may have a cavity, please visit your dentist for a proper diagnosis.
Recognizing Molar Cavities
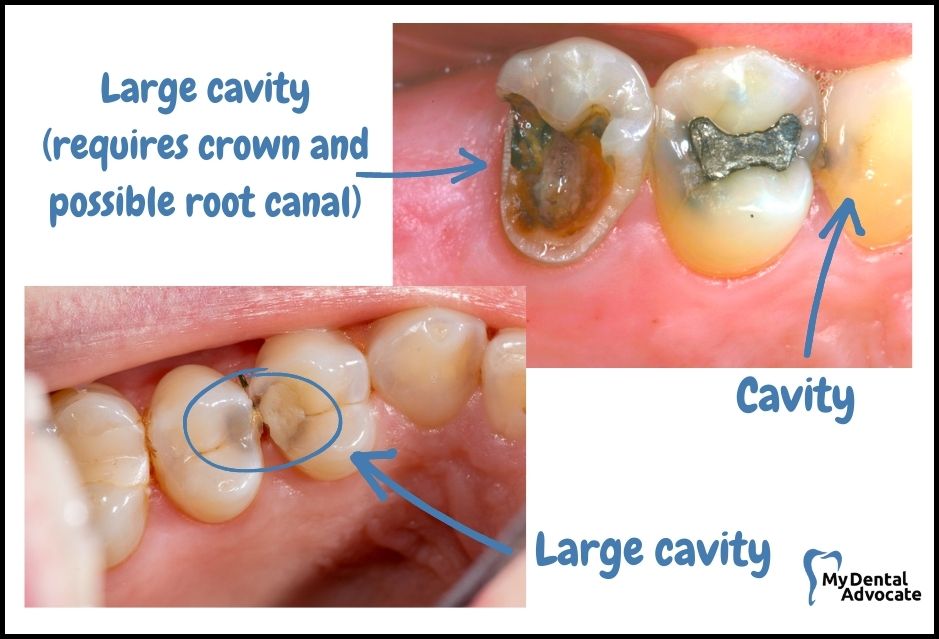
Molar cavities might begin as small discolored spots—usually black or brown—on your teeth.
At first, they can be hard to spot, but as the cavity enlarges, it becomes more evident.
Look for these changes on the chewing surfaces, where cavities often form within the deep crevices.
Adolescents may benefit from dental sealants; these protective coatings are applied to the grooves of molars to thwart cavity development.
If there’s any concern about potential cavities, it’s important to consult your dentist for an accurate assessment.
Identifying Cavities in Children’s Teeth
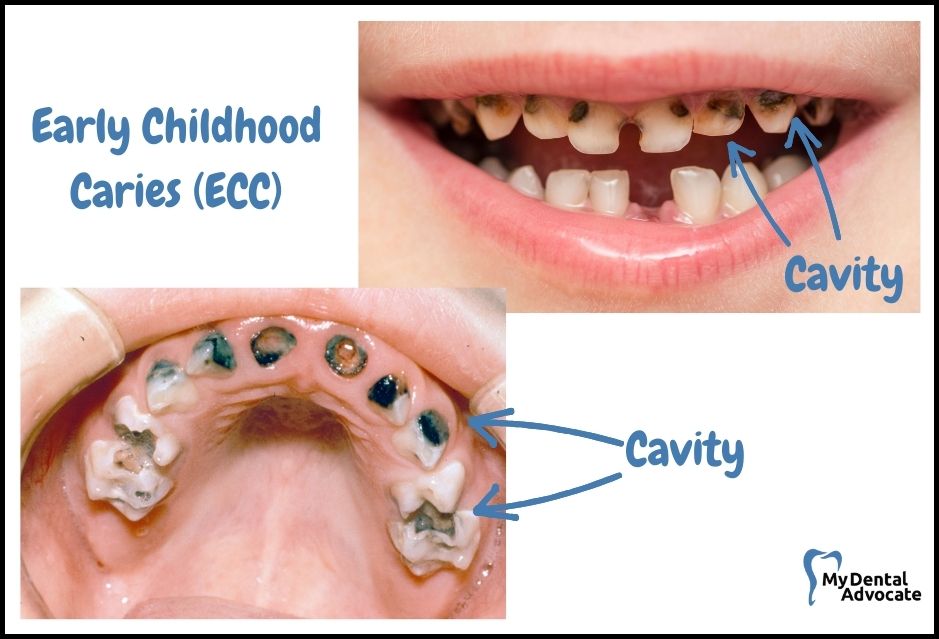
When checking your child’s teeth for signs of decay, you might notice that cavities in their milk teeth appear as small openings. Baby teeth often develop these tiny holes because their teeth are not as large as those in grown-ups and might not show as many signs of trouble.
For little ones under six, Early Childhood Caries (ECC) can happen if even one tooth surface is found decayed, missing due to decay, or filled.
If your child has ECC, they’re more prone to experience additional dental issues, including a susceptibility to future cavities and weaker teeth structure overall. Keep an eye out for these changes to catch any problems early.
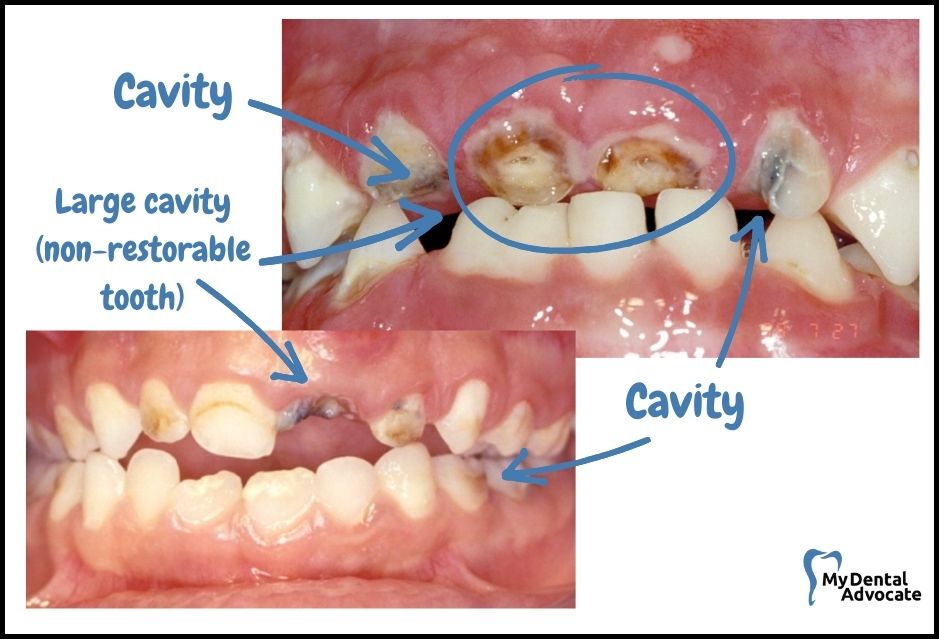
Recognizing Advanced Tooth Decay
- Cavities: They can affect several of your teeth and may reach an irreversible point.
- Progression: Decay can develop either slowly or quickly, depending on the tooth area.
- Discomfort: You might feel pain or even face an infection due to deep cavities in molars.
- Extraction: In some cases, the affected teeth may require removal.
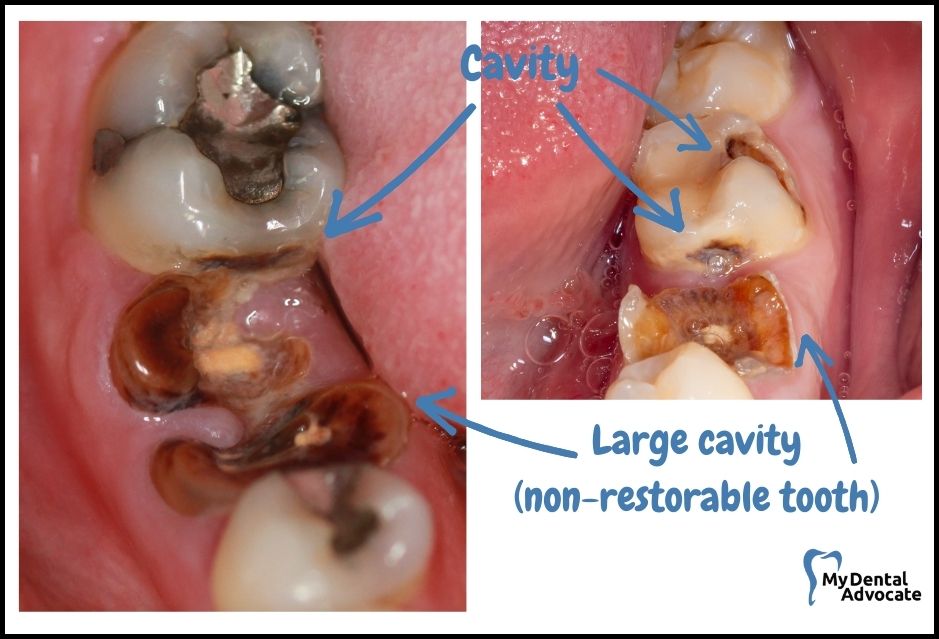
Severe tooth decay occurs when multiple permanent teeth have cavities that progress to a non-restorable state.
Severe tooth decay may occur slowly over time, rapidly on chewing surfaces, or between teeth.
Deep cavities on back teeth may cause pain or infection. When severe tooth decay is present, multiple teeth may need to be extracted.
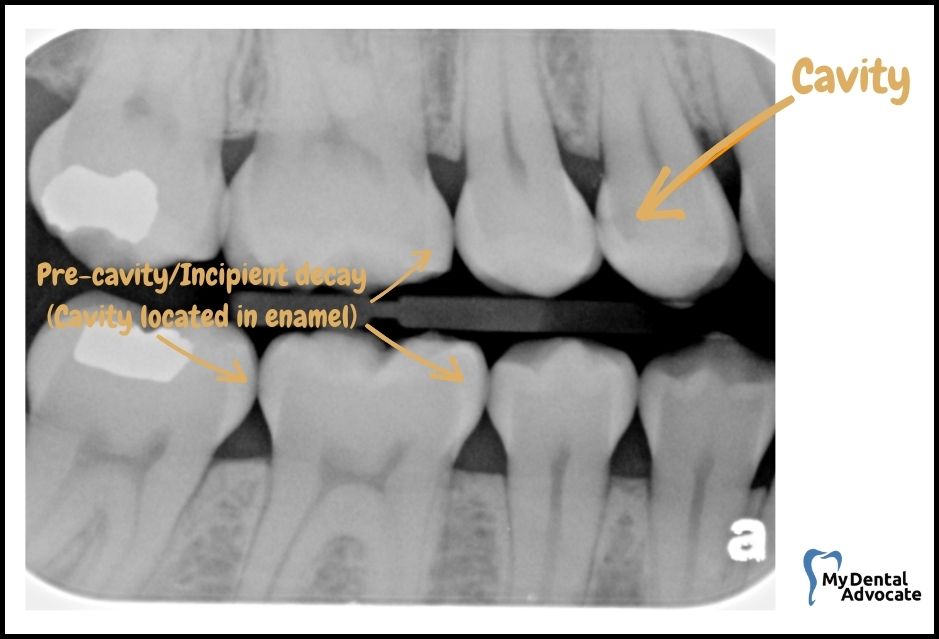
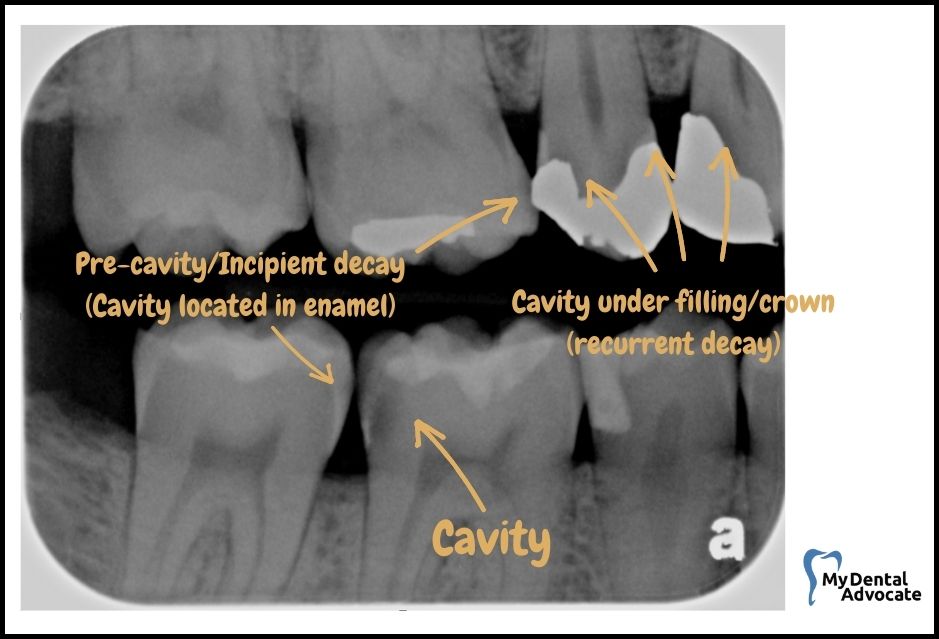
Identifying Dental Decay in Radiographs
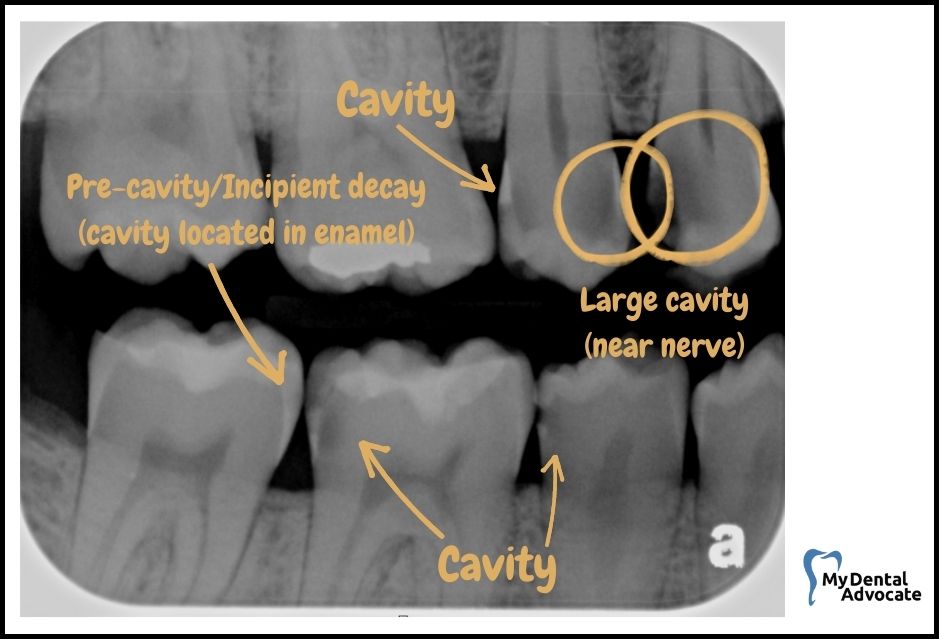
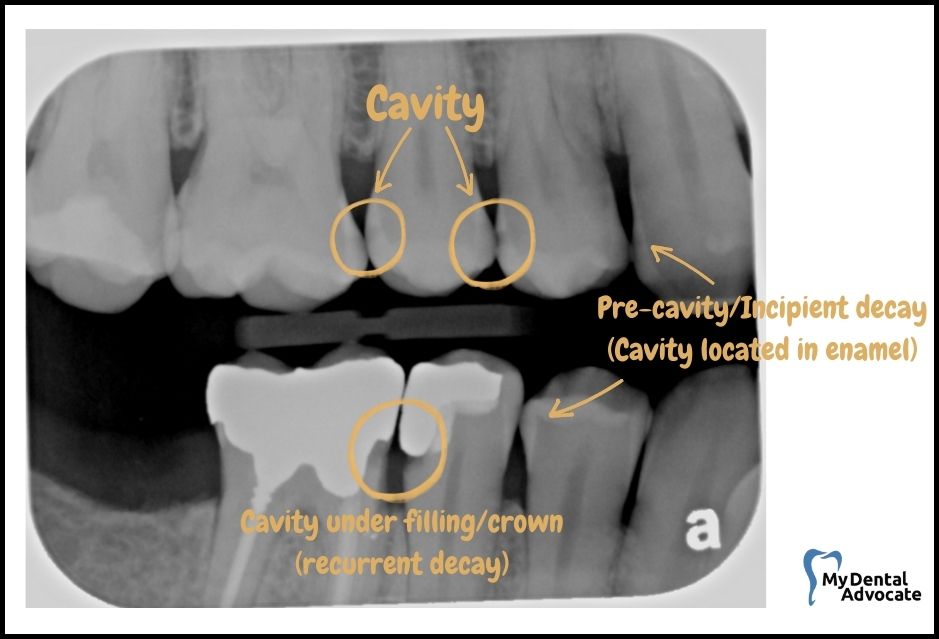
When you glance at dental X-rays, look out for these markings that signify the presence of cavities:
- Dark spots: These indicate where the tooth’s hard surface has been compromised, and decay has set in.
- Location: Frequently seen between teeth and beneath the point of contact.
Remember, these shadowy areas on the X-ray image are where the enamel and dentin have been affected by decay, making them less dense and allowing the X-ray to shine through more clearly, resulting in a contrasting dark appearance against the lighter, healthier parts of the tooth.
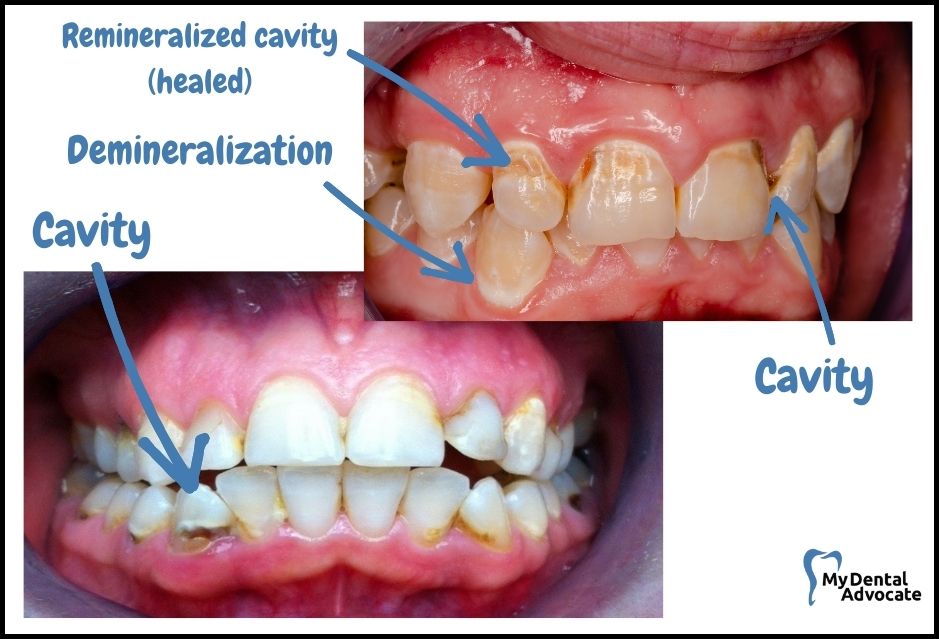
Healing Early Stage Tooth Decay
- Early Intervention:
- Superficial cavities in the enamel can undergo remineralization.
- Being proactive can halt and even reverse the process.
- Limitation:
- Once decay reaches the dentin, a permanent hole forms—remineralization is no longer possible.
- Healing Steps:
- Stay Tuned: Further details on the five key steps will guide your efforts in combating early decay.
Tooth Decay Indicators
Indications of Dental Caries
- Tooth Sensitivity: Your tooth may react strongly to hot, cold, or sweet foods and drinks.
- Discomfort During Meals: You might experience pain while chewing due to the affected tooth structure.
- Visible Marks: Keep an eye out for dark-colored spots on your teeth, which can be a telltale sign.
- Toothaches: Look out for unprompted pain or aches that interrupt your sleep—these can be indicators of advancing decay.
Can Brushing Stop a Cavity?
Brushing regularly is crucial for your oral health, but it might not be enough to halt a cavity that has already started.
- Cleaning away harmful bacteria: Brushing with fluoride toothpaste helps clean your teeth of decay-promoting bacteria.
- Strengthening enamel: Fluoride in toothpaste can assist in remineralizing weakened enamel.
Check out products with the American Dental Association Seal of Acceptance for trusted dental care options.
Flossing & Cavity Reduction
Regular flossing plays a crucial role in cleaning the spaces between your teeth, areas where toothbrush bristles might not reach.
By diligently removing plaque and bacteria from these hard-to-reach spots, you’re helping to prevent the buildup that can contribute to cavities.
- Plaque Removal: Flossing dislodges plaque that could otherwise lead to cavities.
- Gum Health: Keeps gums free from food particles, reducing the risk of gum disease.
- Fresh Breath: Contributes to better breath by removing debris that causes odors.
Remember, combining brushing with flossing provides a more comprehensive clean for your oral health.
Recommended Reading:
Why Does a Cavity Hurt? (5 BEST Toothache Home Remedies)
Signs & Symptoms
- Pain when you bite down
- Pain when you eat hot, cold, or sweet foods
- Dark spots on your tooth
- Sensitive teeth
- Spontaneous pain
- Pain that wakes you up during the night
Natural Methods for Cavity Repair
Evening Fluoride Treatment Using Custom Trays
Your dentist can create tailored fluoride application trays for you. These trays are used with a high-strength fluoride gel, which you’ll apply to your teeth each night.
This method helps replenish lost minerals directly where your teeth need it most.
Dentist-Prescribed High-Fluoride Toothpaste
Another step is to brush with a high-fluoride toothpaste provided by your dentist.
It’s most effective when used before bedtime, and remember, just a small dollop is enough. Don’t rinse after brushing—let the fluoride work its magic overnight.
Professional Fluoride Coating Application
During a dental visit, your dentist can apply a concentrated fluoride varnish to your teeth.
This substance hardens quickly and provides a prolonged release of fluoride to support enamel repair, especially in areas where decay has started.
Choosing the Right Toothpaste
For your daily routine, use a toothpaste containing fluoride or calcium phosphate.
These ingredients are essential for strengthening your enamel and are typically found in products with the ADA Seal of Acceptance.
Enhancing Your Daily Dental Routine
To enhance your oral health, maintain regular dental check-ups, brush at least twice a day, and don’t forget to floss every night.
Using an antibacterial mouthwash can help clear out residual food and deter harmful bacteria.
Recommended Reading: 10 Simple Steps to Prevent Cavities (Dentist’s Perspective)
Potential Issues of Untreated Tooth Decay
- Early Stages: You might not notice discomfort initially.
- Progressing Symptoms: Increased tooth sensitivity and pain may develop.
- Advanced Effects: Potential for tooth loss if decay continues.
Neglecting to treat a developing cavity can lead to discomfort and more serious dental issues. It’s essential to visit your dentist as soon as possible for proper care and to halt further deterioration.
Dental Filling Indicators
- Visible damage: Check for holes or dark spots on your teeth.
- Sensitivity or pain: Be aware if you experience discomfort when eating hot, cold, or sweet foods.
- Texture changes: Feel your teeth. If they’re rough or you detect holes, it’s time for a check-up.
- Lost fillings: Previously filled teeth might need attention if you notice a filling has fallen out.
Composite resin, a blend of plastic and glass, often repairs the damaged tooth’s structure.
Recommendations
Step 1: Nightly Fluoride Trays (Dentist-Required)
Nightly fluoride trays are fabricated at the dentist and require an upper and lower impression of your teeth. Your dentist will also prescribe 1.1% sodium fluoride anti-cavity gel to apply inside the trays.
When you wear them each night, fluoride will directly contact your teeth to remineralize cavities.
Step 2: Prescription Fluoride Toothpaste (Dentist-Required)
Your dentist can also prescribe 1.1% sodium fluoride anti-cavity toothpaste that you should use nightly.
Use a pea-sized amount, and after thoroughly brushing, spit it out and don’t rinse. Rinsing your mouth will inadvertently remove the fluoride minerals and prevent tooth remineralization.
Step 3: Topical Fluoride Varnish (Dentist-Required)
5% fluoride varnish is only available at your dentist and can be directly applied to localized areas of decay. The sticky varnish is gently painted on your teeth and requires no eating or drinking for at least 30 minutes.
The direct application provides a protective barrier for fluoride to take effect.
Step 4: Over-The-Counter Toothpaste
The most effective remineralizing toothpaste contains sodium fluoride, stannous fluoride, or calcium phosphate (hydroxyapatite).
These ingredients bond to weakened enamel, repairing missing tooth structures and preventing future decay. Look for one with the American Dental Association (ADA) Seal of Acceptance.
Recommended Reading: What is the ADA Seal of Acceptance?
Step 5: Oral Health Improvement
Oral health improvement consists of regular dental visits, frequent brushing, and nightly flossing. Antibacterial mouthwash also helps remove food particles while killing cavity-causing bacteria.
However, improving oral health may require mastering new dental habits.
What Happens If You Ignore a Cavity?
Cavities are caused by plaque, a sticky film of bacteria that forms on teeth. Plaque produces acids that eat away at tooth enamel, causing cavities.
If you have a cavity, you may not experience any symptoms at first.
However, as the cavity gets larger, it can cause pain, sensitivity to hot and cold temperatures, and even tooth loss.
If you think you may have a cavity, it’s essential to see your dentist immediately so they can treat it before it worsens.
How Do I Know If I Need a Filling?
If you have a cavity, your dentist will likely recommend a filling to restore the tooth’s function and appearance. A filling is a type of dental restoration that repairs teeth that have lost their original mineral structure and luster.
The most common type of filling material is composite resin, made of plastic and glass particles.
Recommended Reading: 12 Cavity Risk Factors (Best Treatment)
My Experience & Expertise
Cavities come in all shapes and sizes, but they always have one thing in common: they’re a sign that something is wrong with your oral health.
If you notice any of the symptoms discussed in this blog post, it’s time to see a dentist. By catching tooth decay early on, you can avoid bigger problems and keep your smile looking great for years to come.
It’s important to remember that home remedies should not replace professional dental care, as untreated cavities can lead to pain, infection, and tooth loss.
Also, it would be best to use home remedies as temporary pain relief until your dentist can see you. If you notice signs of infection, including fever, difficulty breathing or swallowing, or your eye is beginning to shut, seek immediate emergency care.
Need a second opinion? We can help! Learn more. Knowledge is power when cultivating healthy dental habits. The more informed you are, the better positioned you’ll be to prevent avoidable and potentially costly dental procedures for you and your family. Watch for future blog posts, where we’ll continue sharing important information, product reviews and practical advice!

About the Author
Dr. Matthew Hannan, also known as “Dr. Advocate,” is a board-certified dentist on a mission to provide accurate dental patient education. He attended Baylor University before completing dental school at UT Health San Antonio School of Dentistry. He now lives in Arizona with his beautiful wife and 4 kids. Dr. Hannan believes everyone should access easy-to-read dental resources with relevant, up-to-date dental research and insight to improve their oral health.

Connect with Dr. Hannan!
-
Braces Cause Teeth Stains? (How to Prevent Them)
As a dentist, one of the most common concerns that patients have is the appearance of their teeth. While braces can help straighten teeth and improve their alignment, they can also cause teeth stains that can be difficult to remove…
-
Best Dentist-Recommended Gum (Top Picks)
Chewing gum has long been a popular pastime, but not all gums are created equal regarding oral health. Some can even offer dental benefits when chosen wisely. Dive into our list of the top 5 dentist-recommended gum that not only freshen your breath but also promote a healthier mouth.
-
Best Dental Implant Brands (Full Review)
If you’re missing one or more teeth, you’re not alone. Millions of people worldwide have lost teeth due to injury, decay, or other causes. Thankfully, dental implants can provide a permanent solution to this problem.
Gain Clarity with Our FREE Second Opinion Guide
FREE online second opinion within 48 hours. No joke!
Product Reviews
Our 300+ dental product reviews (and counting), curated by an experienced dentist, are the most comprehensive online.
Toothbrush Genie
State-of-the-art chatbot designed to help you discover your perfect toothbrush in just a few simple steps!
Cavity Risk Assessment
Cutting-edge digital tool designed to evaluate your individual cavity risk based on your responses to a series of questions.
Gum Disease Assessment
Discover your gum disease risk with our quick and engaging 6-question assessment!





