What Does Gingivitis/Gum Disease Look Like? (20 Pictures)
Gingivitis is uncomfortable; your gums bleed, your breath smells, and your teeth hurt.
But did you know that 94% of Americans have gingivitis? That’s an alarming statistic!
However, what’s more alarming is that gingivitis can progress to gum disease if left untreated. What does gingivitis look like?
If you believe you have gingivitis or gum disease check out the pictures and schedule an appointment with your dentist ASAP.
Need Dental Advice? It’s FREE!
Recommended Reading: Gingivitis | The Ultimate Guide
What Is Gingivitis?
Gingivitis is inflammation of the gums caused by harmful bacteria.
If your dentist or hygienist does not remove harmful bacteria, the bacteria will congregate and multiply into advanced gum disease (periodontal disease).
The bacteria that infects the gums lead to swollen, red and puffy gums. Gingivitis is a common gum issue.
However, oral hygiene improvements can help prevent this ailment. According to the American Dental Association, gingivitis and periodontitis cause tooth loss in adults.
Recommended Reading: What is Gingivitis? Causes, Symptoms & Treatment 2026
What Causes Gingivitis?
- Poor Oral Hygiene: Neglecting regular brushing and flossing can lead to dental plaque, causing gum inflammation. Routine dental cleanings help remove plaque and prevent severe gum diseases like periodontal disease.
- Poor Nutrition: Harmful oral bacteria thrive on sugars and carbs, leading to their growth. Proper oral care, including brushing, flossing, and cleanings, prevents harmful bacteria caused by sugary foods.
- Dental Plaque: Plaque forms when food debris isn’t removed, typically along tooth and gum margins. Regular brushing and nightly flossing limit plaque and prevent gum inflammation due to the bacteria it contains.
- Tartar (Calculus): If plaque isn’t removed, it hardens into tartar under the gumline, shielding bacteria and causing gum irritation. Professional dental cleaning is needed to eliminate tartar, unlike plaque that can be managed with regular care.
Recommended Reading: Pregnancy Gingivitis: Causes, Symptoms & Treatment 2026
What Are the Signs & Symptoms?
It’s possible to have gingivitis without any symptoms.
However, there may be no discomfort or noticeable symptoms in mild cases of gingivitis. Often, it remains undetected for quite some time. The symptoms of gingivitis are somewhat non-specific.
The pink-salmon coloring and stippling in the gum tissue will often disappear. Also, the gums may appear shiny as the gum tissue becomes inflamed and stretched over the tissue surface.
Common Signs
- Red & purple gums
- Swollen & puffy gums
- Gum inflammation & discoloration
- Gum separation & recession
- Bleeding gums
- Halitosis (bad breath)
Common Symptoms
- Tender gums
- Pain when chewing
- Sensitive teeth & gums
Recommended Reading: Gingivitis vs Periodontitis (Gum Disease) Overview
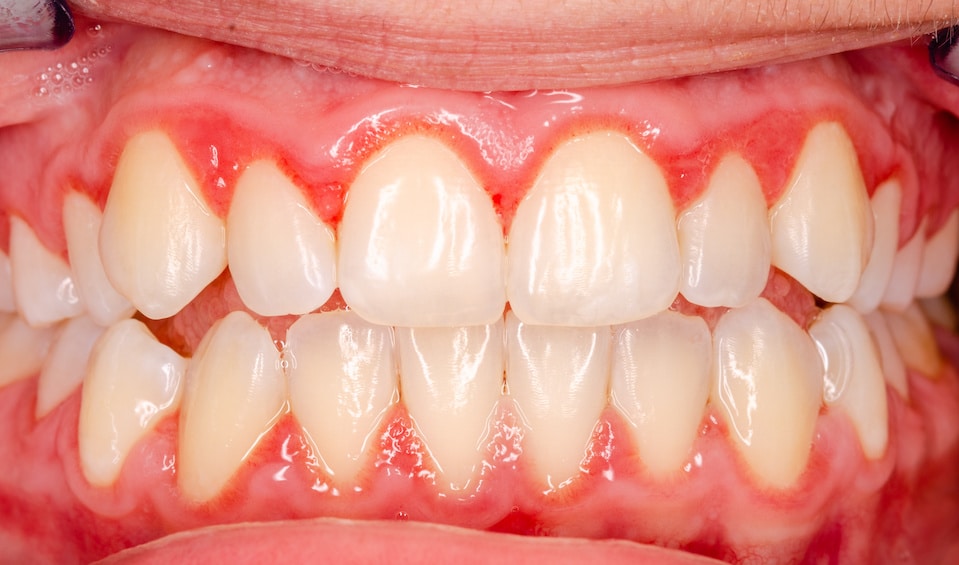
When the gums are swollen, the lining becomes ulcerated, and the gums are prone to bleed even with gentle brushing and flossing.
In addition, if the gums are inflamed, they may start pulling away from the neck of the tooth.
This causes gaps between the teeth and the gums, known as gum pockets (or periodontal pockets).
Recommended Reading: 14 Gingivitis Home Remedies That Work! (Dentist Recommended)
Similarly, many people aren’t aware that they have gum disease (periodontal disease). Periodontal disease, also known as periodontitis, can cause teeth to shift position, wobble or hurt when you chew. In addition, periodontal disease will lead to irreversible bone loss.
Periodontal disease is treated with scaling and root planing, also known as deep cleaning. If gum disease is not controlled, your dentist will refer you to a gum specialist known as a periodontist.
Gum Disease Classifications
- Gingivitis: Neglecting regular brushing and flossing leads to dental plaque formation, causing gum inflammation and gingivitis. Gingivitis features swollen, red, and puffy gums without bone loss. It’s reversible but progresses to gum disease (periodontitis) if untreated.
- Early Periodontitis: Harmful bacteria localized deep under the gums cause further inflammation and infection. These bacteria move downward along the tooth root, initiating bone loss.
- Moderate Periodontitis: Continued bone loss and gum inflammation occur. Tooth mobility begins, along with bone loss between tooth roots.
- Advanced Periodontitis: Tooth mobility and pus formation characterize this stage. Gum disease is irreversible, compromising tooth stability once bone loss occurs. Immediate professional care is necessary to prevent generalized tooth loss.
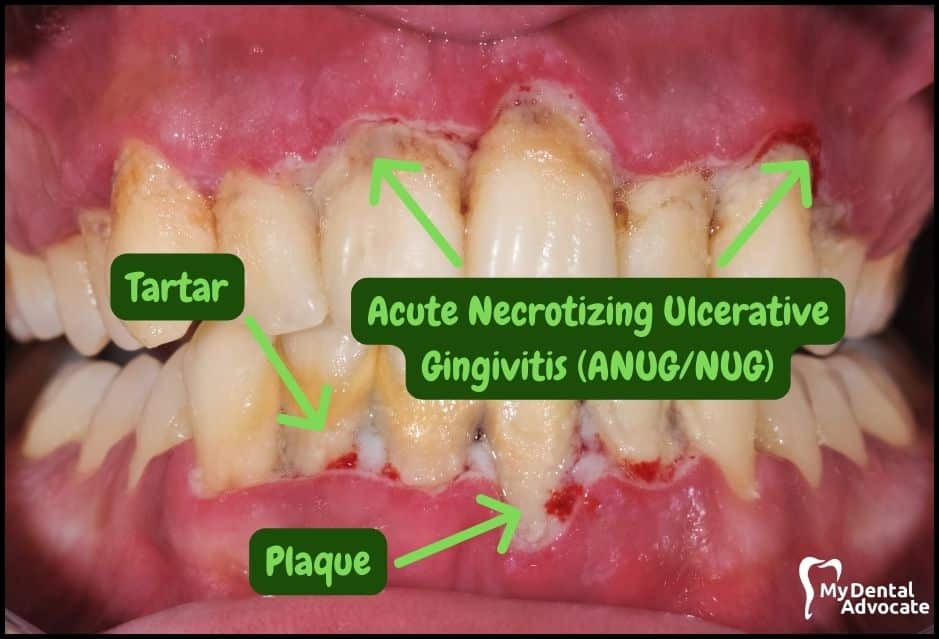
- Acute Necrotizing Ulcerative Gingivitis (ANUG/NUG): This is a severe condition beyond advanced periodontitis. More damaging bacteria cause sudden inflammation, pain, and “punched-out” crater-like lesions on the gums. It commonly occurs in young adults.
Recommended Reading: Acute Necrotizing Ulcerative Gingivitis (ANUG) “Trench Mouth”
Gum Disease Pictures (20 Total)
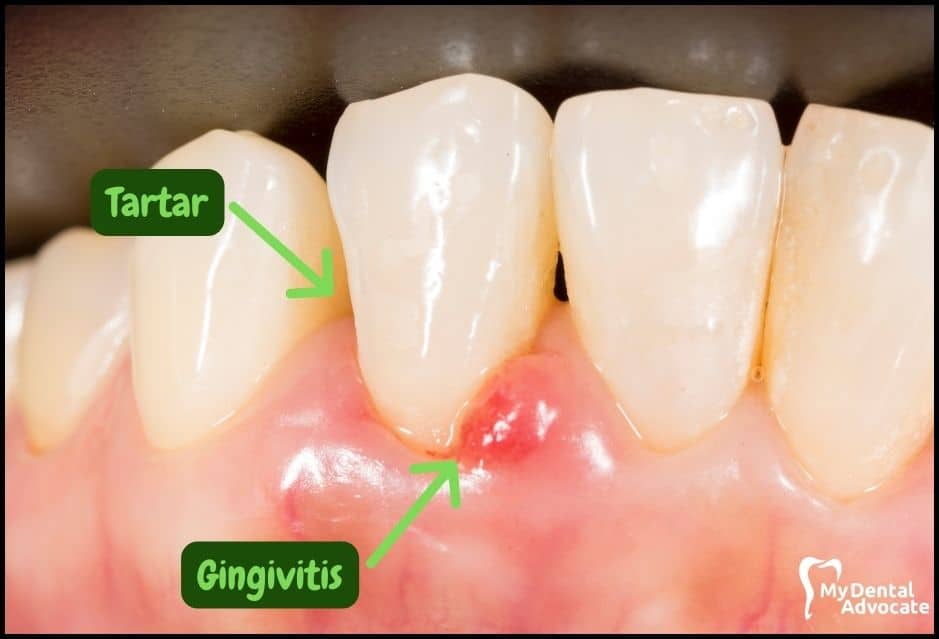
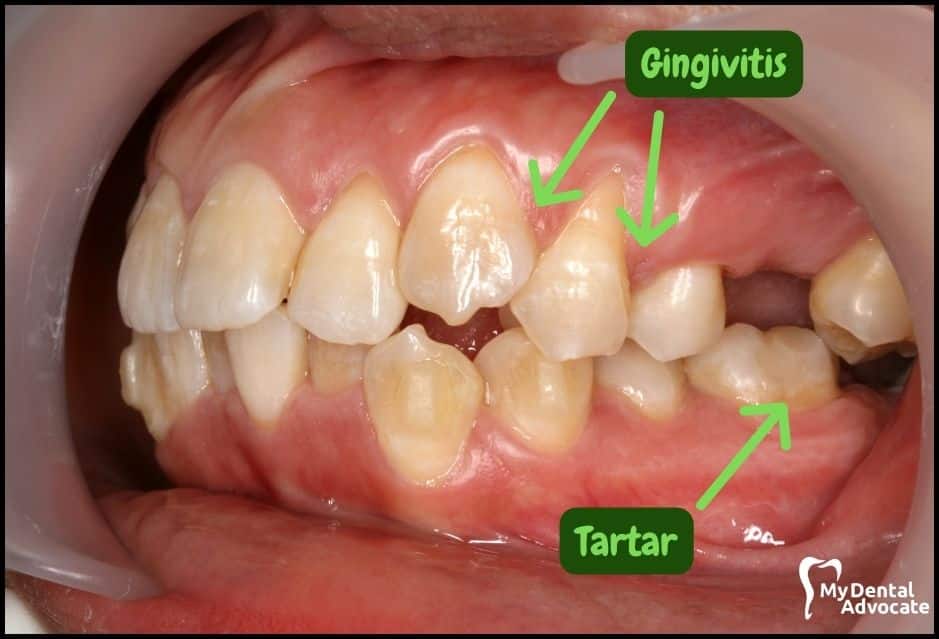
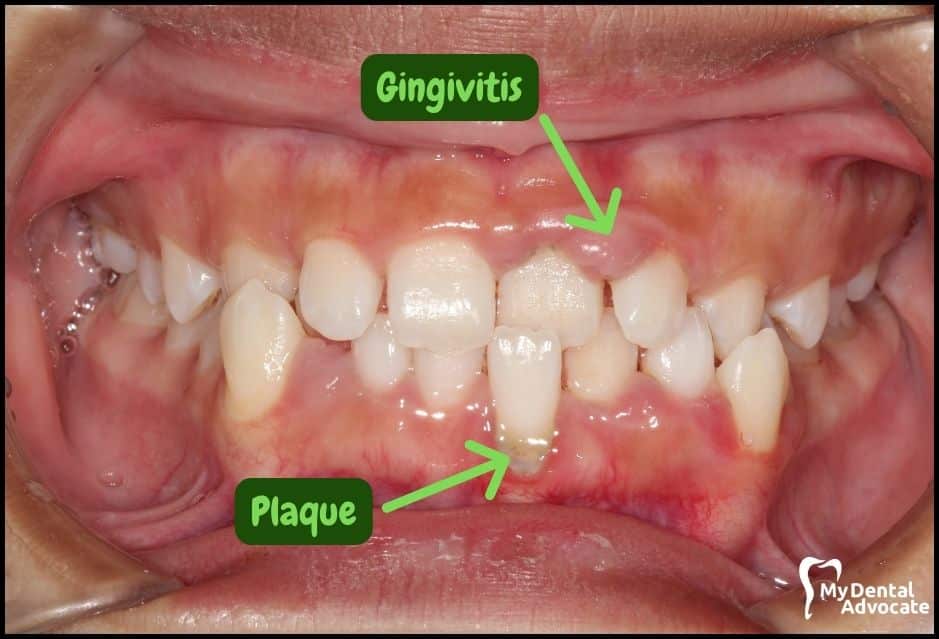
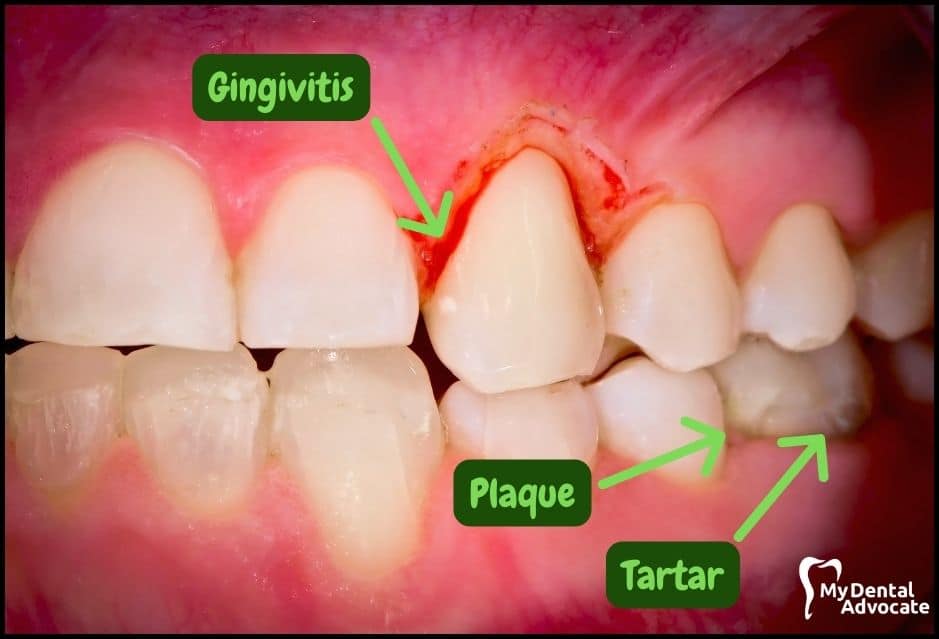
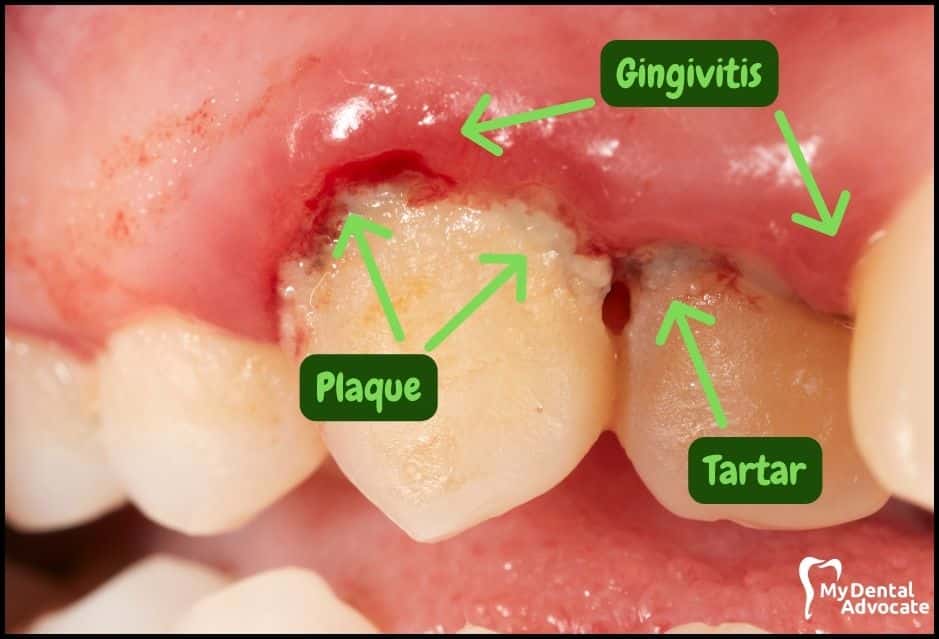
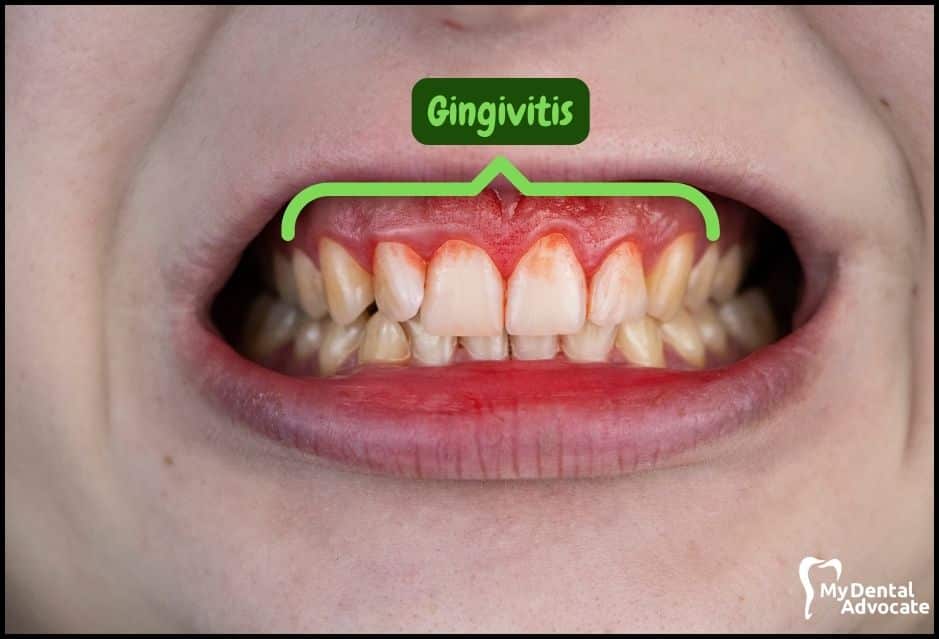
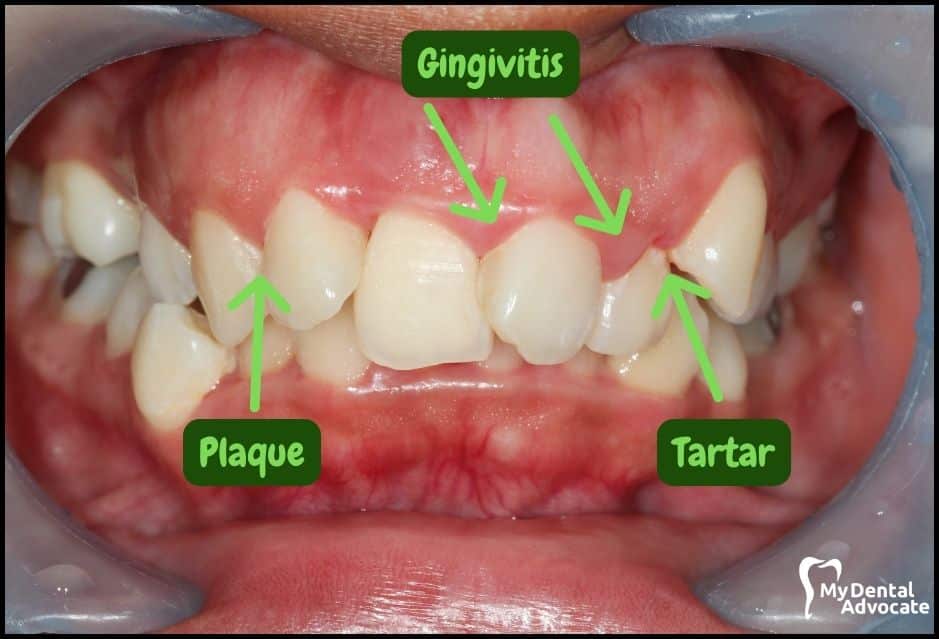
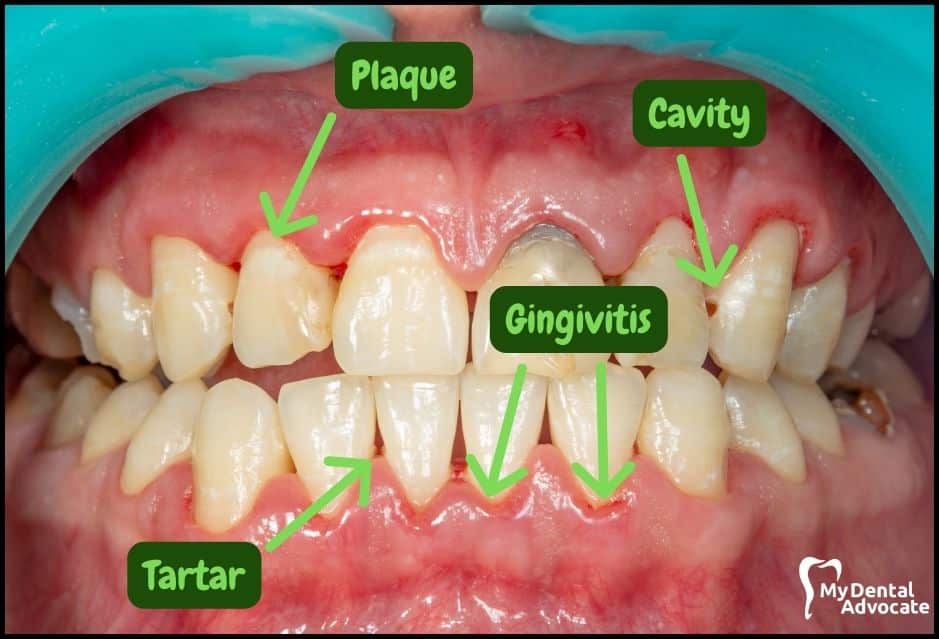
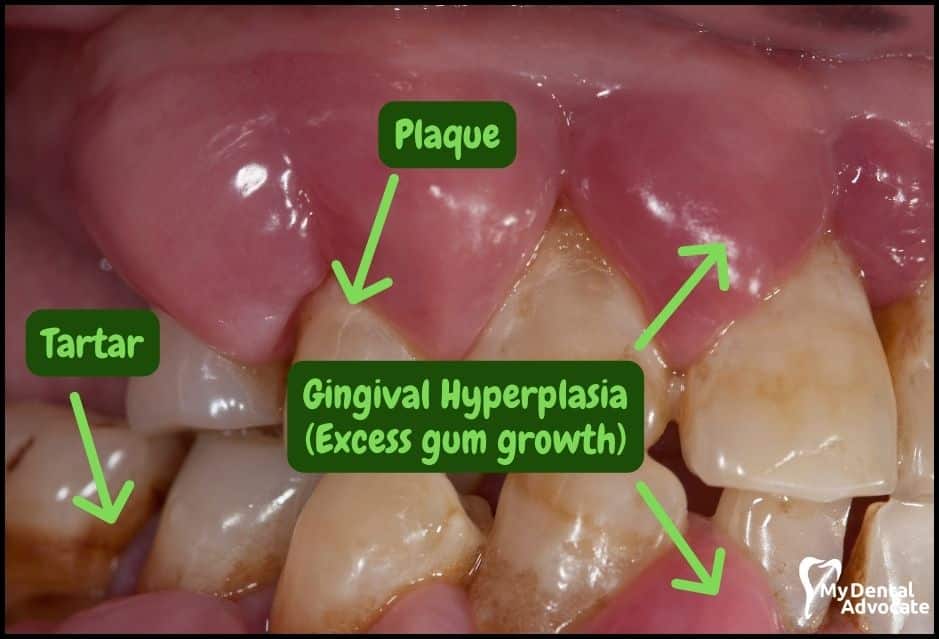
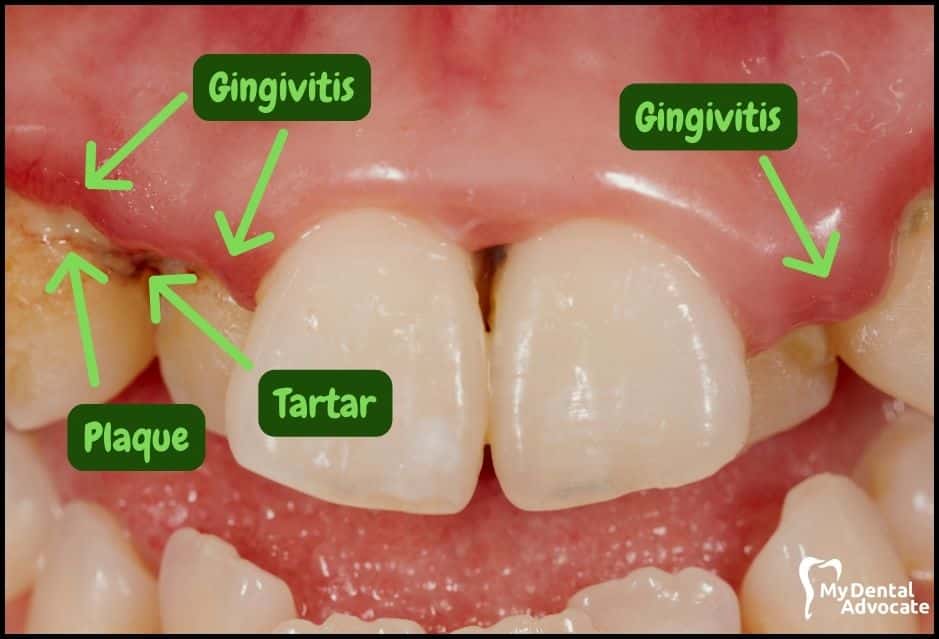
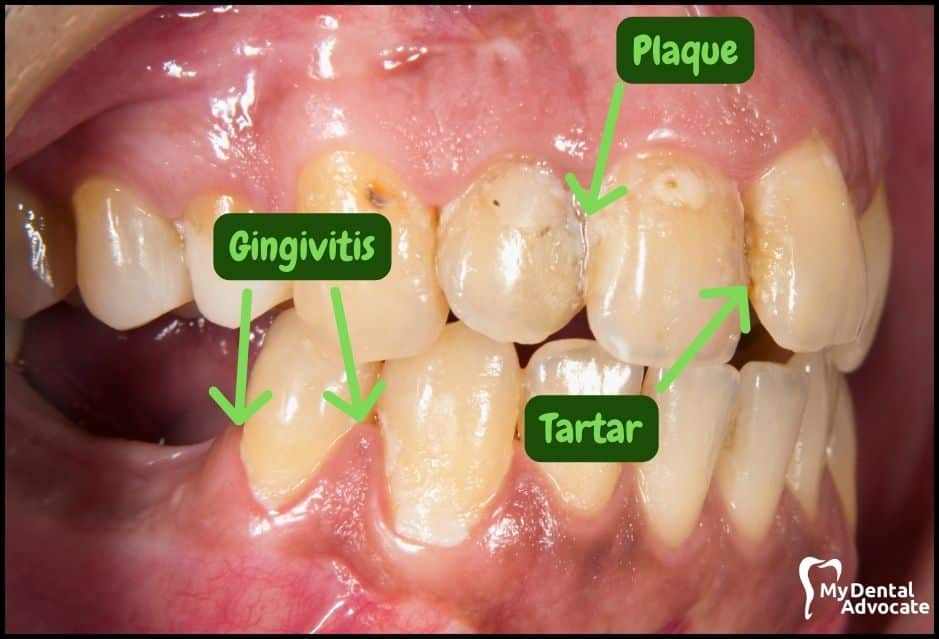
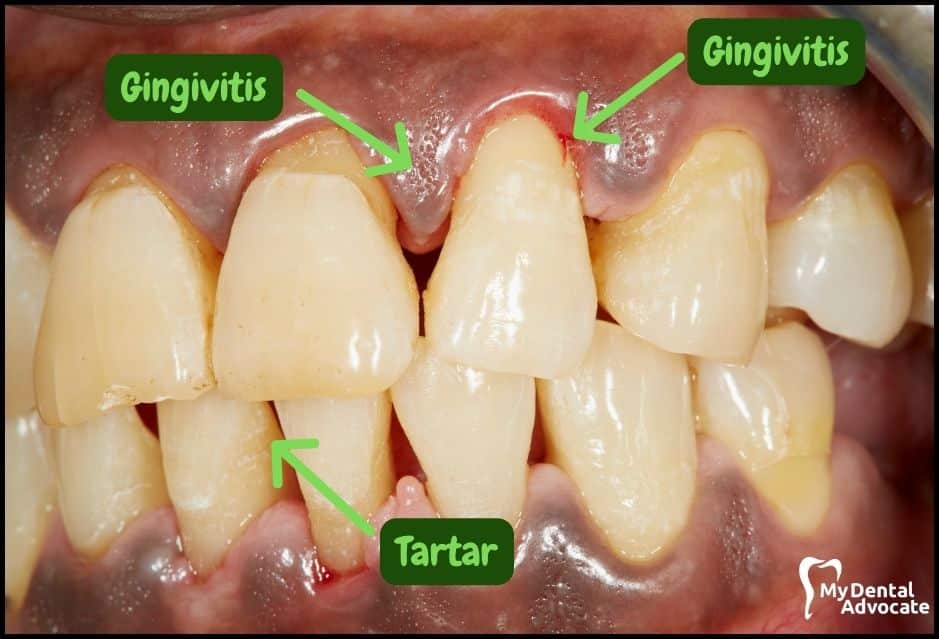
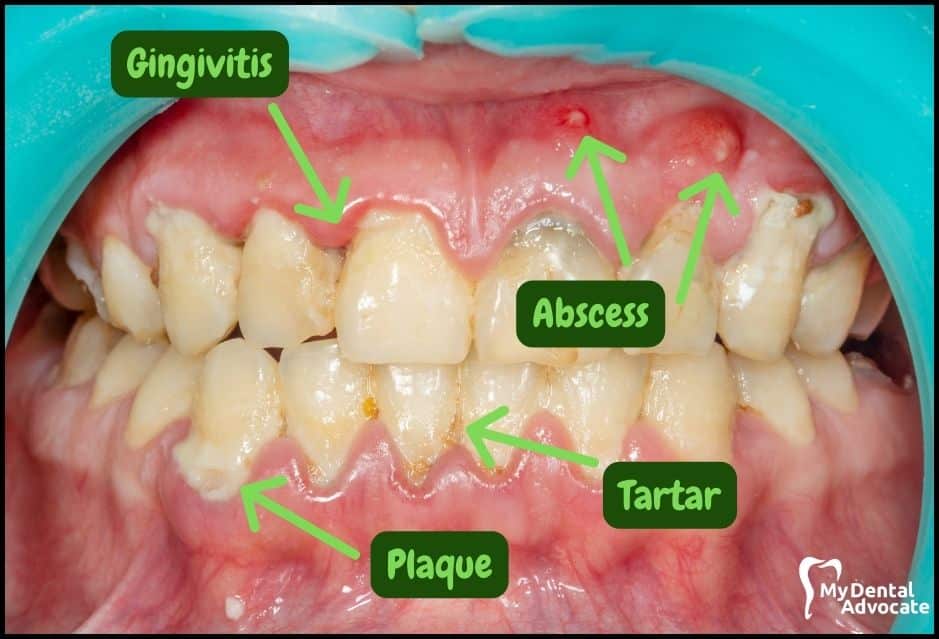
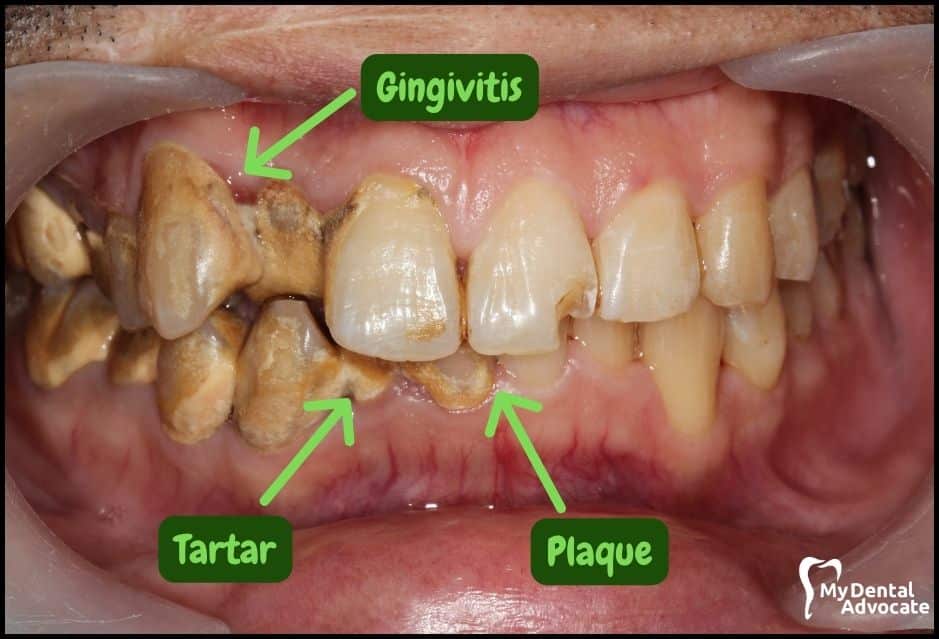
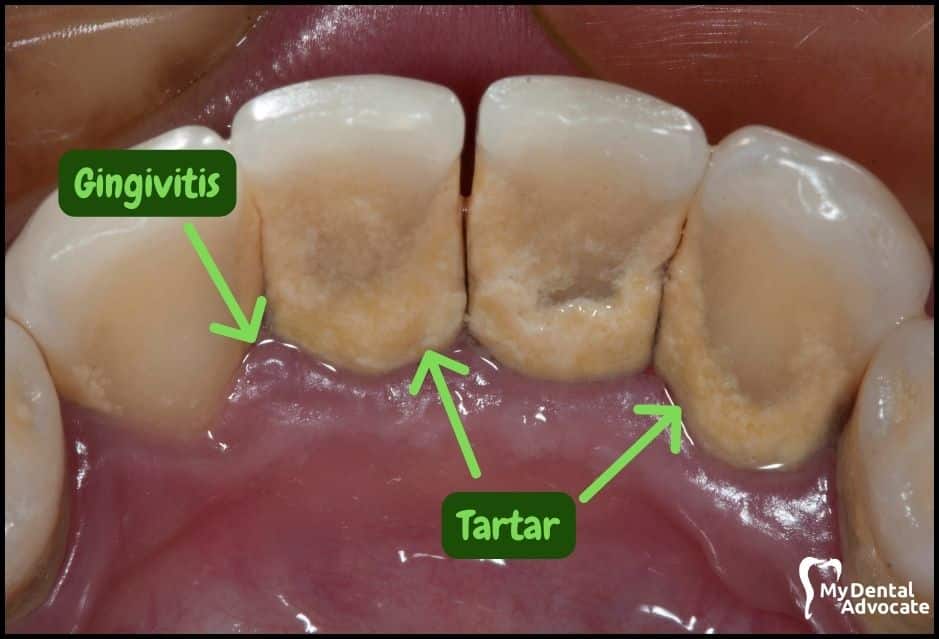
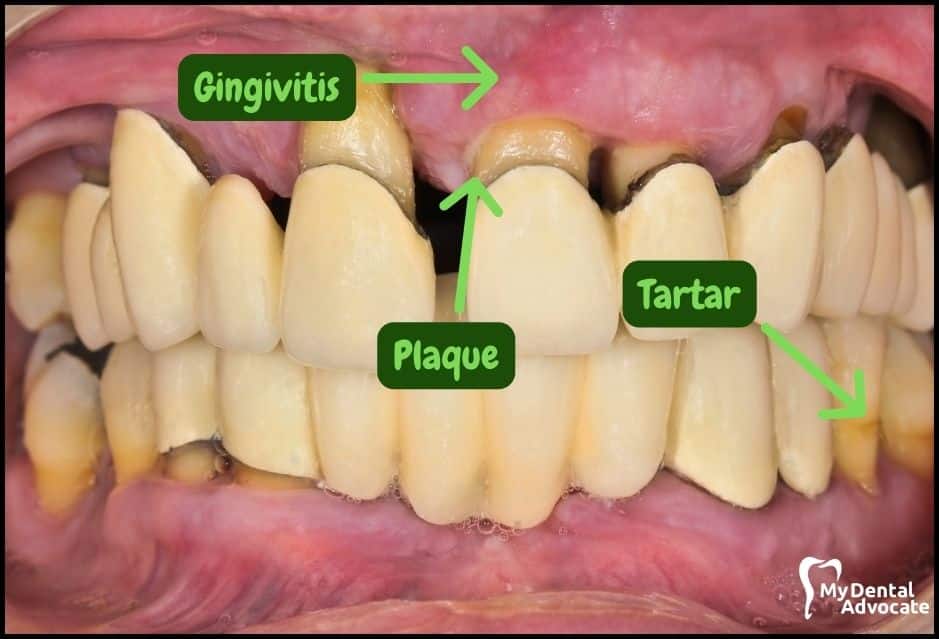
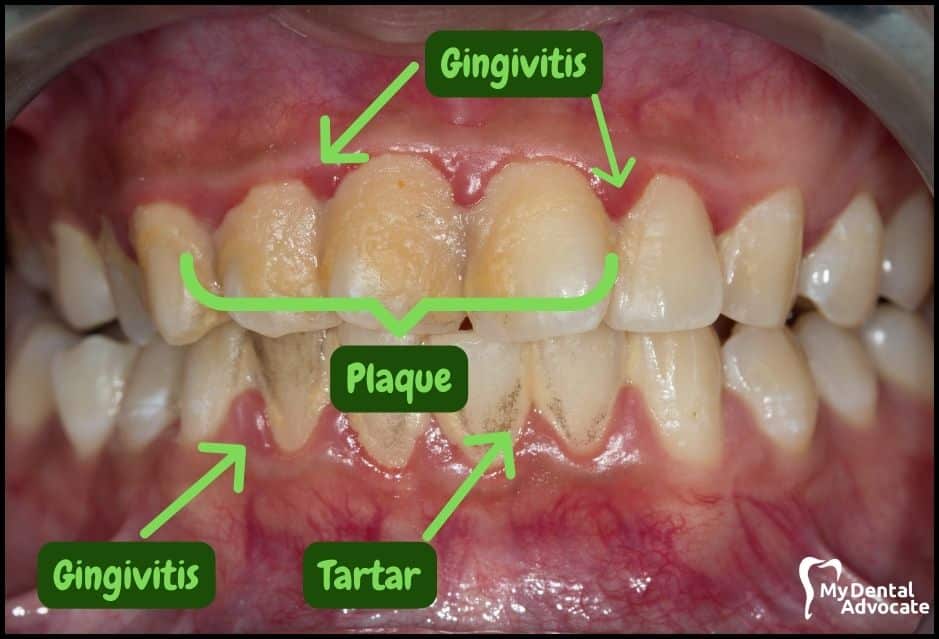
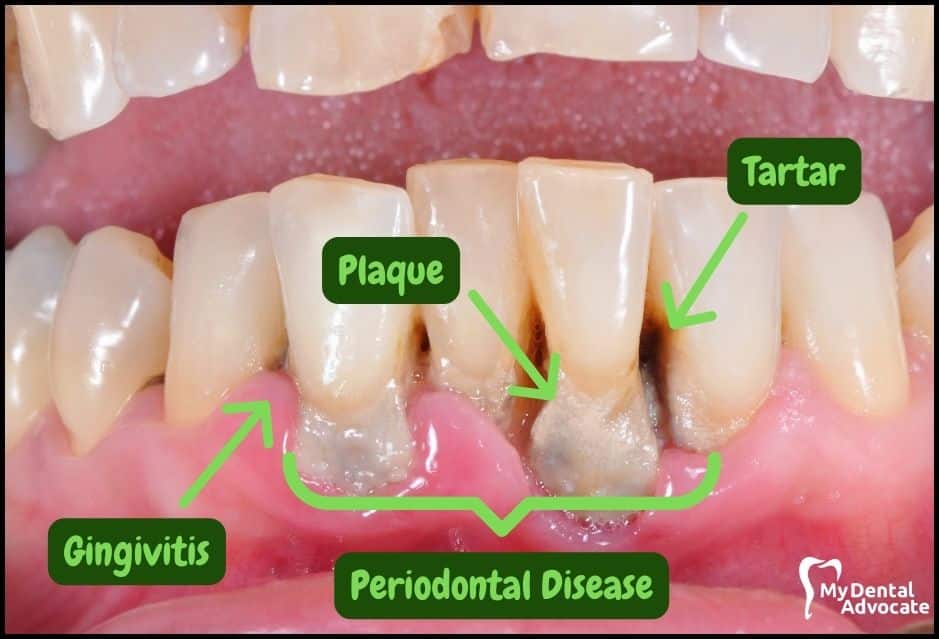
Let’s take a closer look at what gingivitis and gum disease looks like in the mouth. We’ll order them from least to most severe so you can see a distinct transition from health to harm.
Take note of the gum colors, inflammation, plaque and tartar present. Although we have great pictures available, an accurate diagnosis is incomplete without gum measurements, dental x-rays and medical/dental information.

When to See the Dentist
According to the CDC, researchers have uncovered potential links between gum disease and other severe health conditions.
The harmful bacteria in the mouth that enters the bloodstream are usually harmless to individuals with healthy immune systems. But under certain circumstances, these microorganisms are associated with health problems such as stroke and heart disease.
Call your dentist if you or someone you know has signs and symptoms of gingivitis. Your dentist may examine you at your next checkup or make a special appointment.
Recommended Reading: Is Gingivitis & Gum Disease Contagious? (What the Research Says)
My Experience & Expertise
The prevalence of gingivitis is exceptionally high.
If you’ve been diagnosed with gingivitis, don’t panic. Instead, contact your dentist ASAP for professional care and treatment.
Fortunately, gingivitis is reversible and managed with improved oral care, routine cleanings and proper nutrition.
Don’t delay; contact your dentist today!
Need a second opinion? We can help! Learn more. Knowledge is power when cultivating healthy dental habits. The more informed you are, the better positioned you’ll be to prevent avoidable and potentially costly dental procedures for you and your family. Watch for future blog posts, where we’ll continue sharing important information, product reviews and practical advice!

About the Author
Dr. Matthew Hannan, also known as “Dr. Advocate,” is a board-certified dentist on a mission to provide accurate dental patient education. He attended Baylor University before completing dental school at UT Health San Antonio School of Dentistry. He now lives in Arizona with his beautiful wife and 4 kids. Dr. Hannan believes everyone should access easy-to-read dental resources with relevant, up-to-date dental research and insight to improve their oral health.

Connect with Dr. Hannan!
-
Prescription Fluoride Toothpaste (Expert Advice)
Whether or not you should use prescription fluoride toothpaste depends on your cavity-risk potential and the determination by your dentist. For example, if you are at high risk for tooth decay, have sensitive teeth…
-
Best Natural Mouthwash (Top Review)
Are you tired of the burning sensation from chemical-laden mouthwashes? If so, it’s time to turn a new leaf in your oral care routine. Embrace the power of nature’s ingredients to keep your breath fresh, your teeth sparkling, and your gums healthy.
-
Best Electric Toothbrush for Travel
If you’re always on the go, you know how challenging it can be to maintain your oral hygiene routine. That’s where electric toothbrushes come in handy. They are portable, compact and can help keep your teeth and gums clean and healthy…
Gain Clarity with Our FREE Second Opinion Guide
FREE online second opinion within 48 hours. No joke!
Product Reviews
Our 300+ dental product reviews (and counting), curated by an experienced dentist, are the most comprehensive online.
Toothbrush Genie
State-of-the-art chatbot designed to help you discover your perfect toothbrush in just a few simple steps!
Cavity Risk Assessment
Cutting-edge digital tool designed to evaluate your individual cavity risk based on your responses to a series of questions.
Gum Disease Assessment
Discover your gum disease risk with our quick and engaging 6-question assessment!





