Gingivitis vs Healthy Gums

Harmful bacteria that cause gingivitis can progress into severe gum disease or creep into your bloodstream (yuck!).
Most patients with gingivitis or gum disease are unaware because they don’t have pain.
Understanding the differences between gingivitis and healthy gums will help you evaluate your oral and systemic health. Let’s take a closer look from a dentist’s perspective.
Recommended Reading: Gingivitis | The Ultimate Guide
Need Dental Advice? It’s FREE!
Gingivitis vs. Healthy Gums (What’s the Difference)
Healthy gums appear firm and coral pink. It’s not uncommon to have a stippling surface resembling an orange peel.
In addition, the architecture of the jaw bone below the gums is readily visible and variable. Signs of unhealthy gums include redness, swelling and puffiness. In addition, harmful bacteria cause your gums to bleed when you brush or floss.
Gum disease will continue to advance if the bacteria are not removed, leading to the gums appearing to pull away from the teeth and generalized bone loss.
Recommended Reading: 5 Best Mouthwash for Bleeding Gums 2026 (Dentist Recommended)
Factors undermining healthy gums include tobacco use, malnutrition, poor oral hygiene, and poor immune response. In addition, certain medications, including antihistamines, decongestants, and painkillers, can cause dry mouth and promote gum disease.
Gum disease and cavity-causing bacteria thrive in dry, acidic environments. If you struggle with dry mouth, consider reading our dry mouth product and oral rinse reviews.
As a dentist, I remind my patients that healthy gums aren’t just essential for oral health.
Maintaining healthy gums has a direct impact on your overall health. According to a recent study, bacteria that cause gum disease (periodontitis) are directly linked to chronic health conditions, including Alzheimer’s, diabetes and heart disease.
Recommended Reading: What is Gingivitis? Causes, Symptoms & Treatment 2026
What Is Gingivitis?
Gingivitis is inflammation of the gums caused by harmful bacteria.
If your dentist or hygienist does not remove harmful bacteria, the bacteria will congregate and multiply into advanced gum disease. The bacteria that infects the gums lead to swollen, red and puffy gums.
Gingivitis is a common gum issue and a clear warning sign that we must be more proactive about our oral health; however, oral hygiene improvements can help prevent this ailment.
Recommended Reading: 14 Gingivitis Home Remedies That Work! (Dentist Recommended)
What Does Gingivitis Look Like?
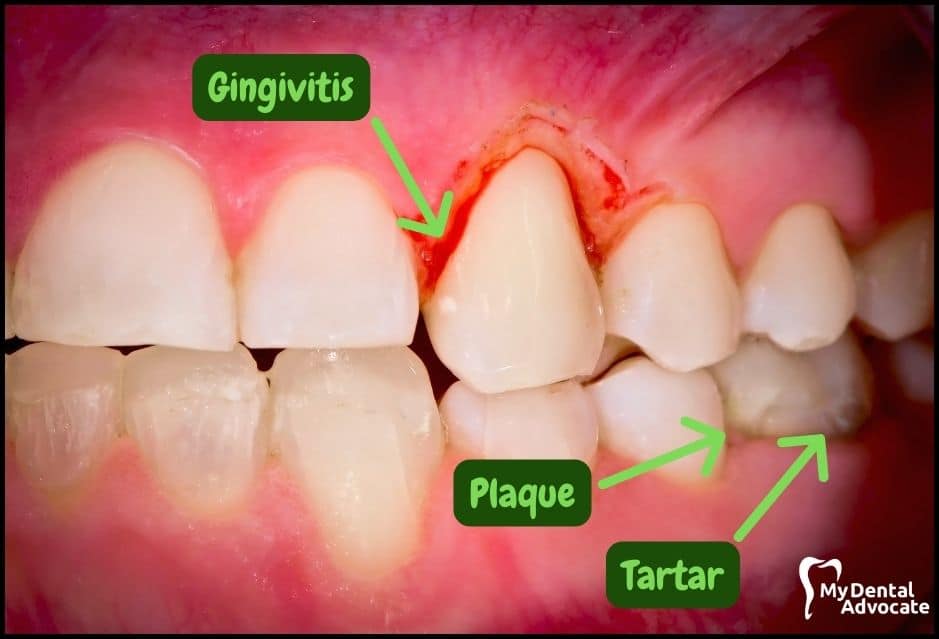
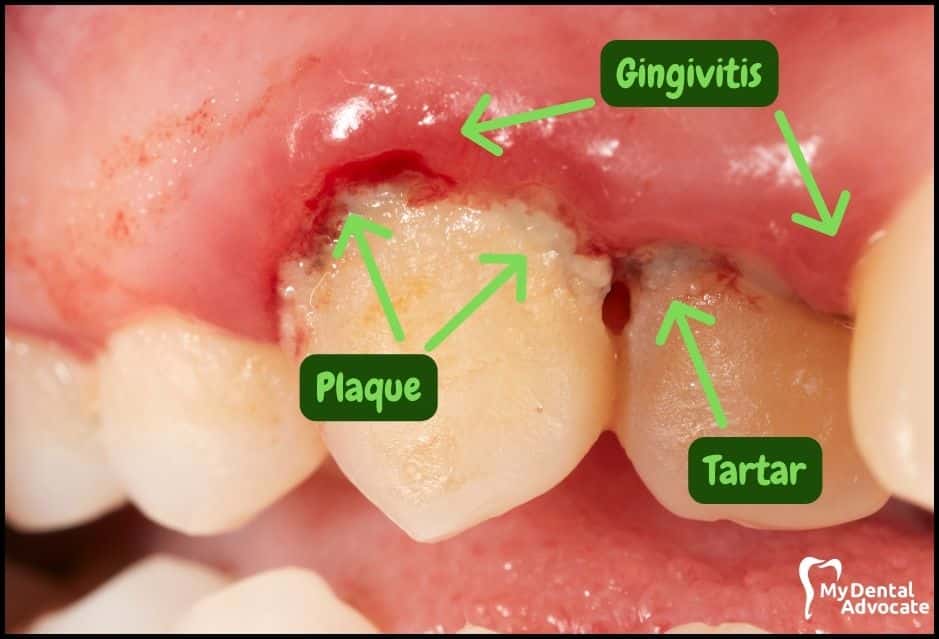
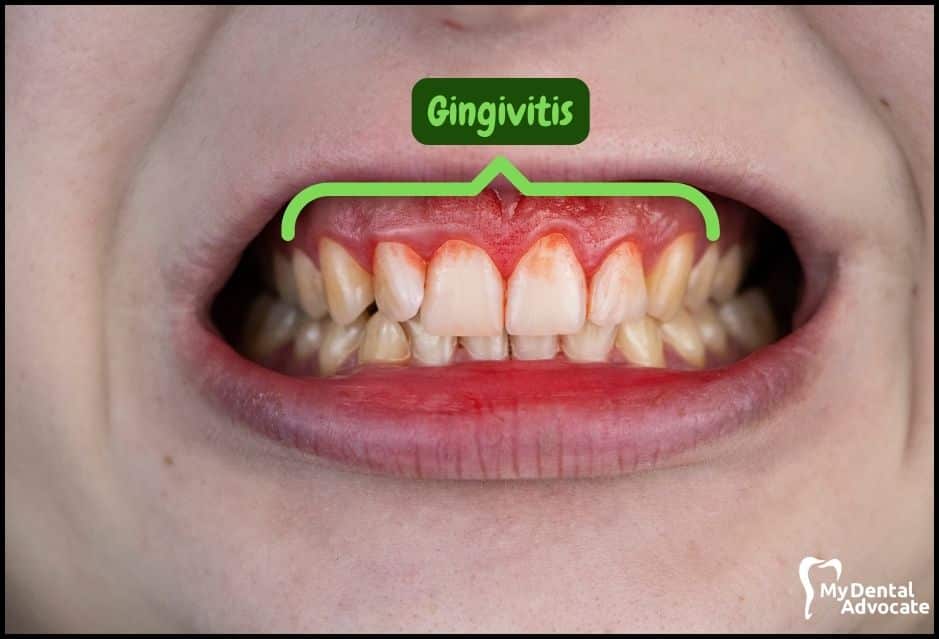
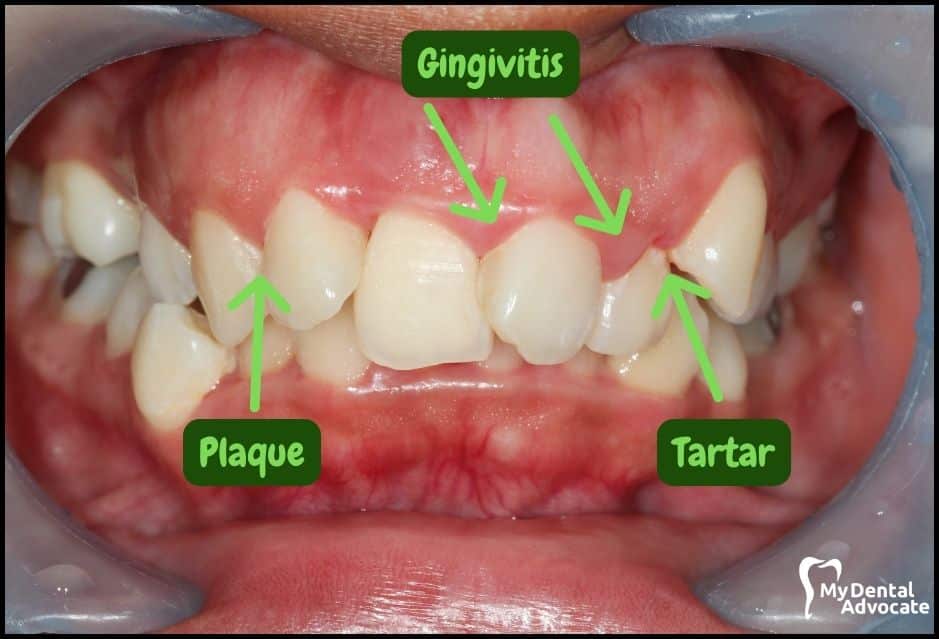
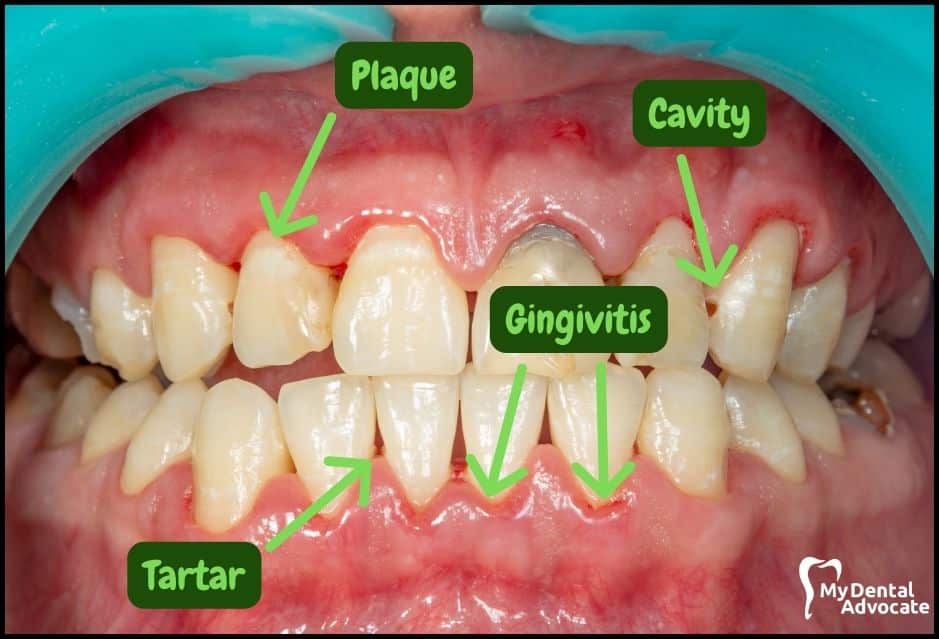
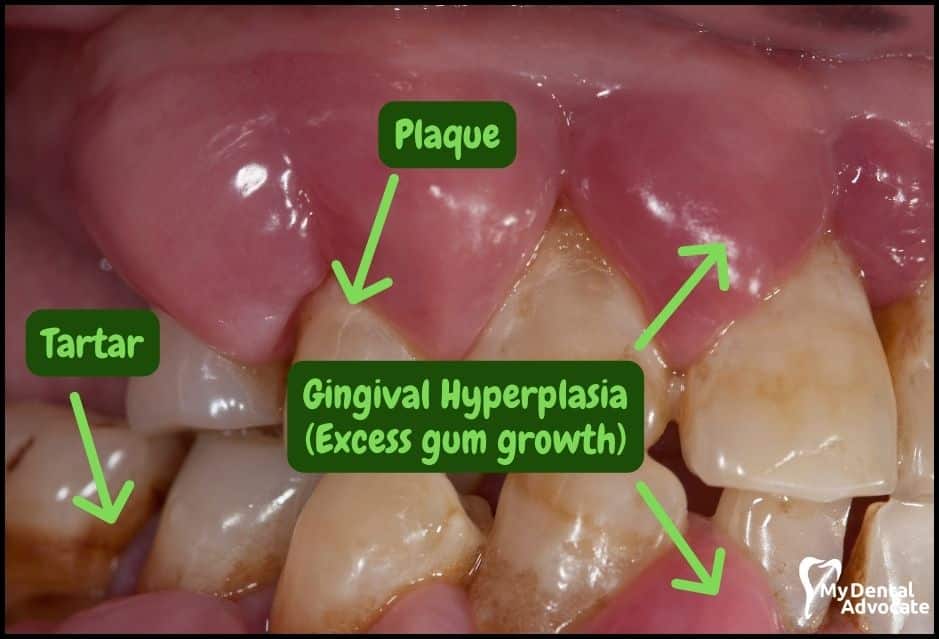
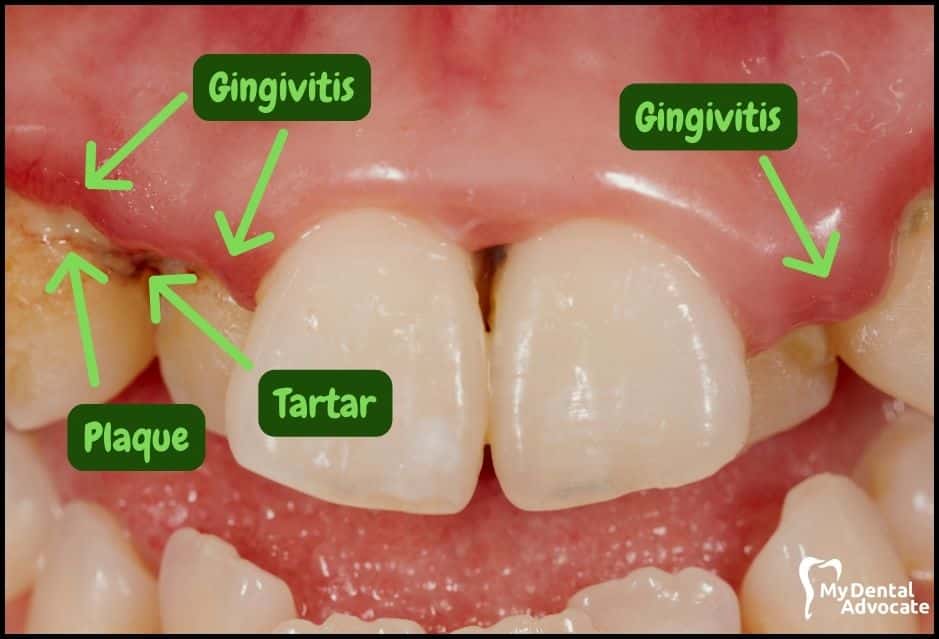
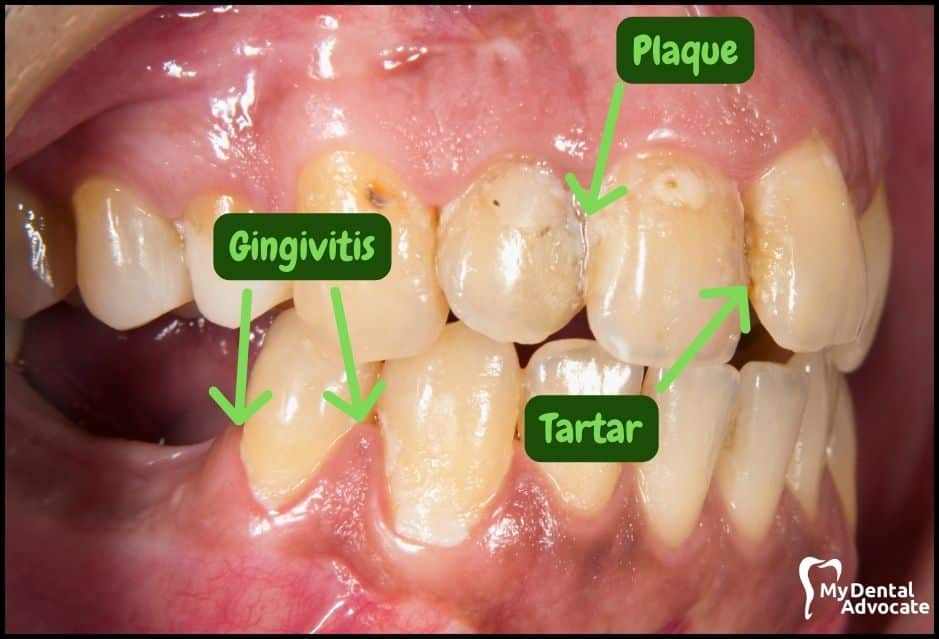
Let’s take a closer look at what gingivitis and gum disease looks like in the mouth.
We’ll order them from least to most severe so you can see a distinct transition from health to harm. Take note of the colors of the gum, inflammation, plaque and tartar present.
Although we have great pictures available, an accurate diagnosis is incomplete without gum measurements, dental x-rays and medical/dental information.
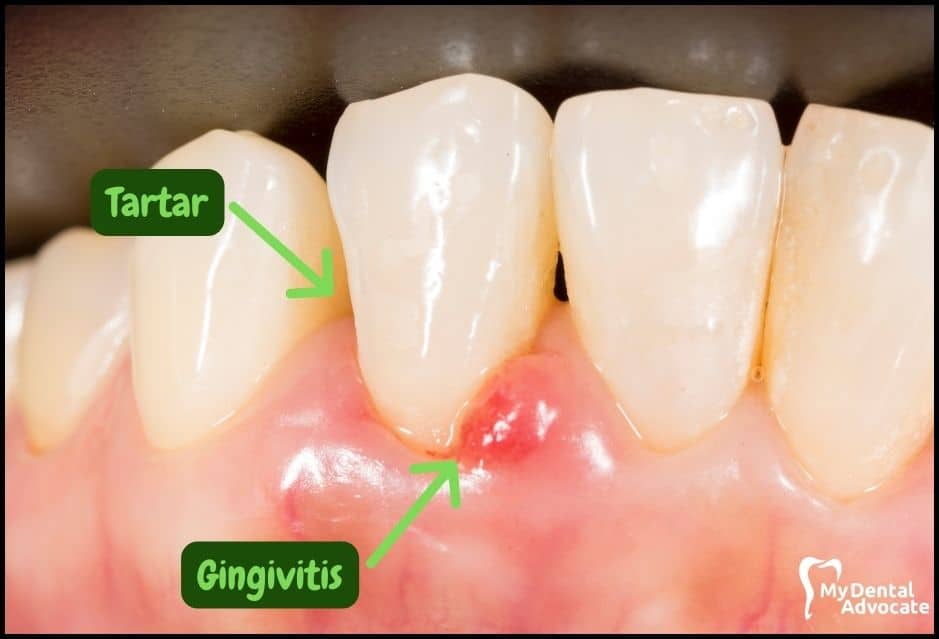
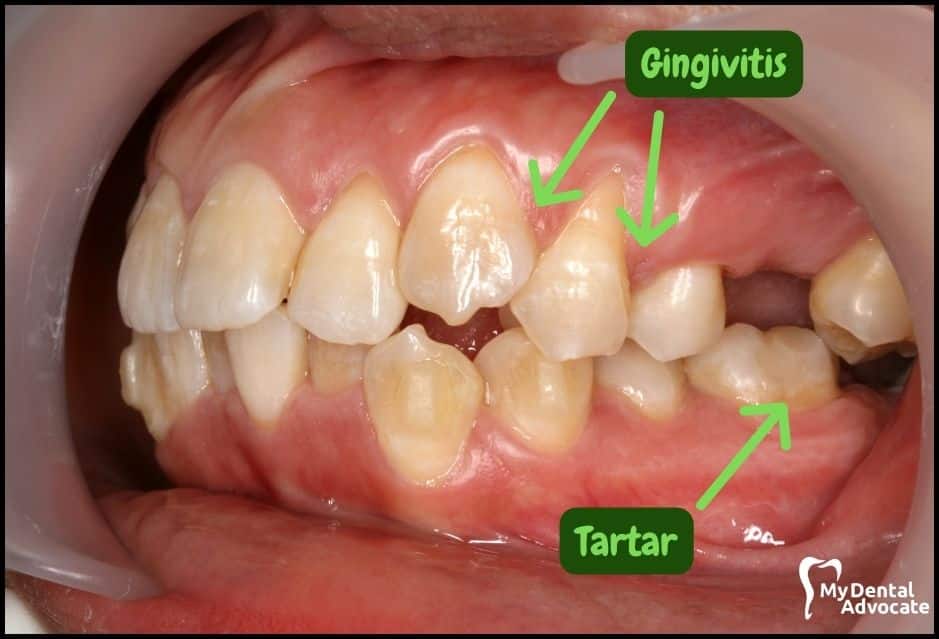
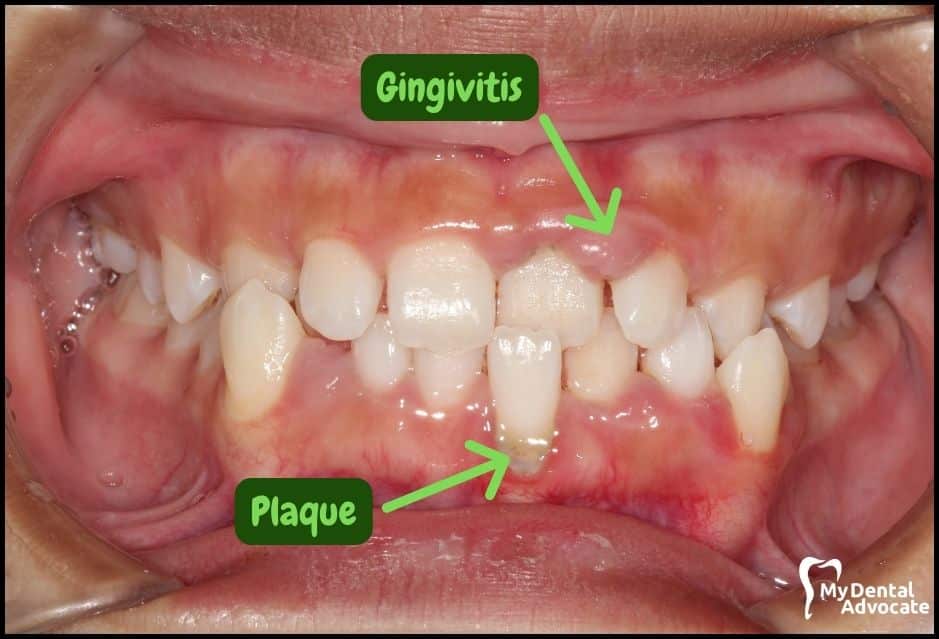
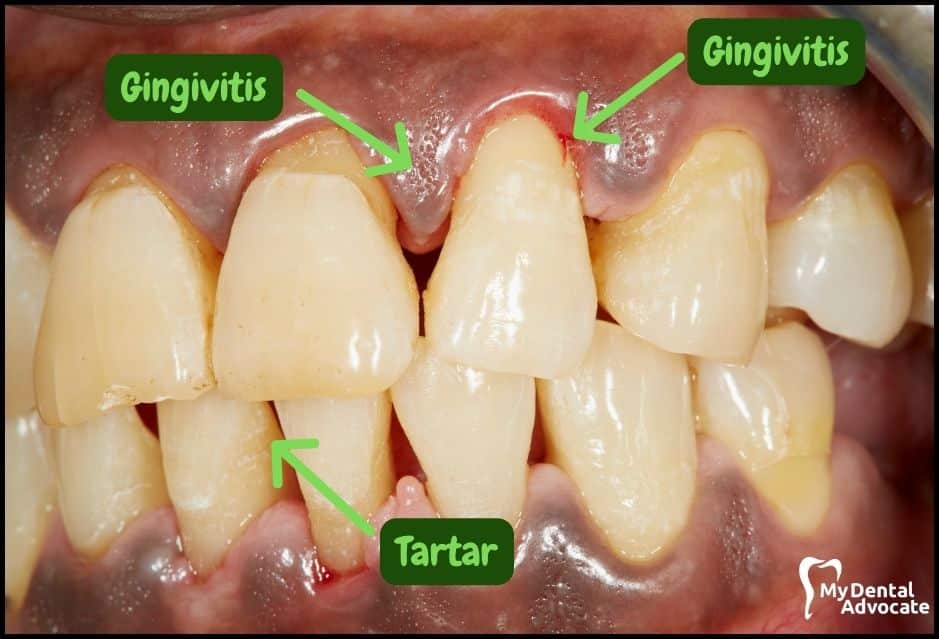
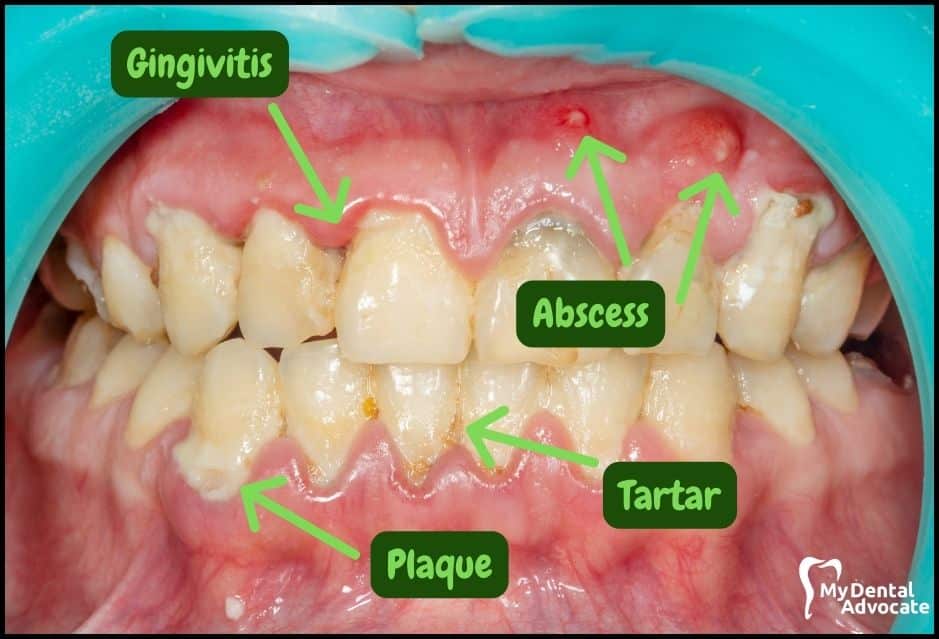
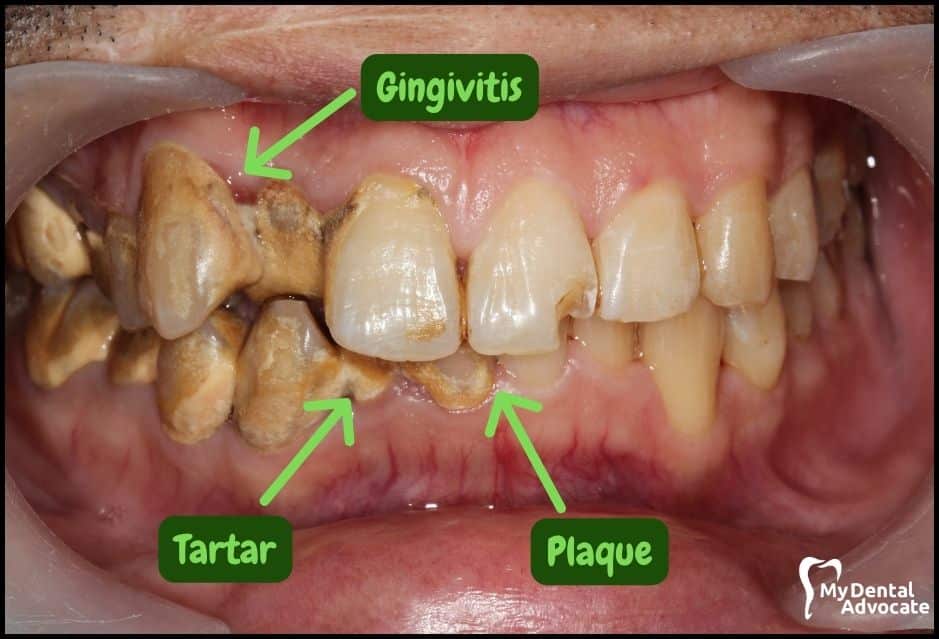
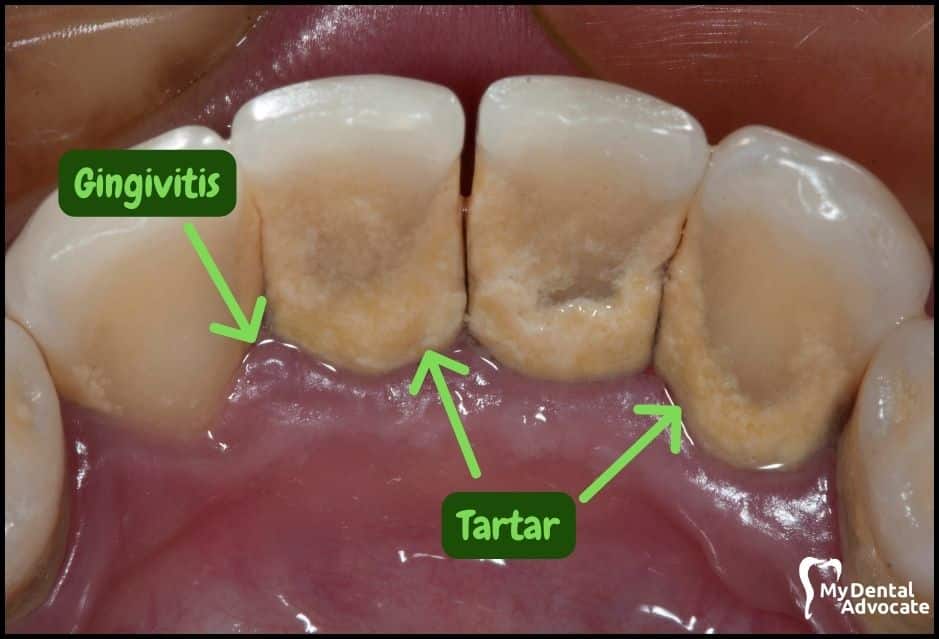
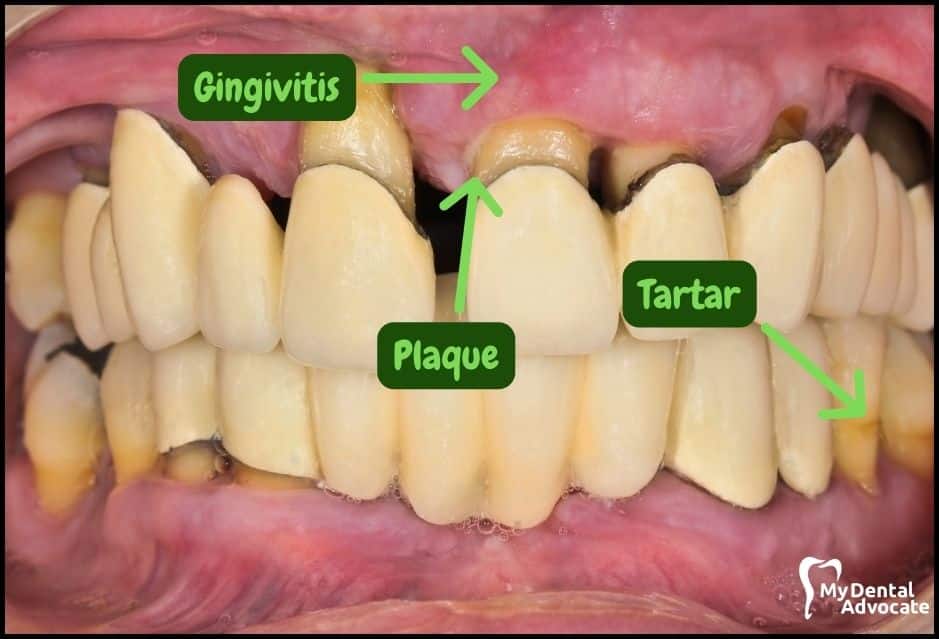
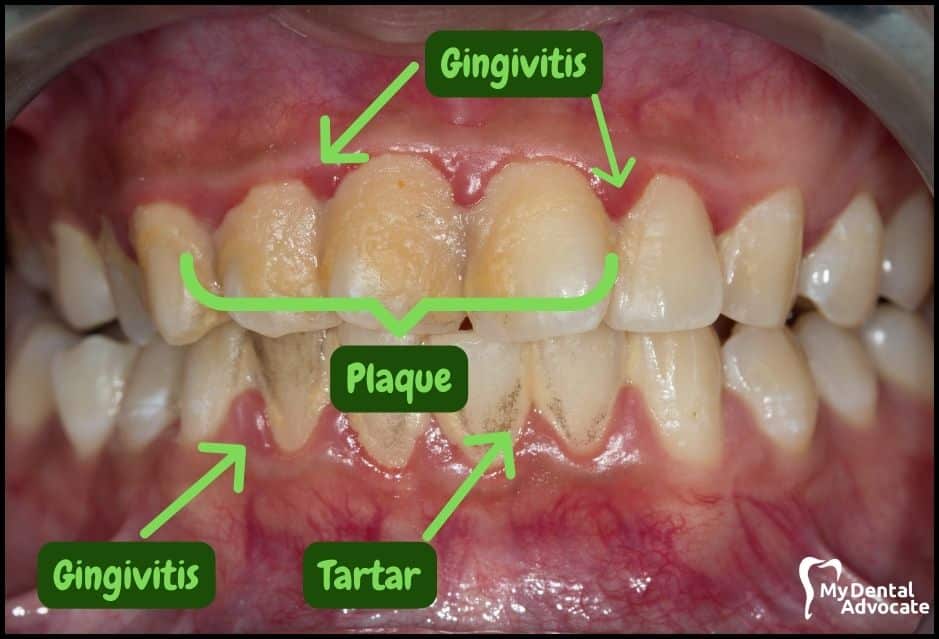
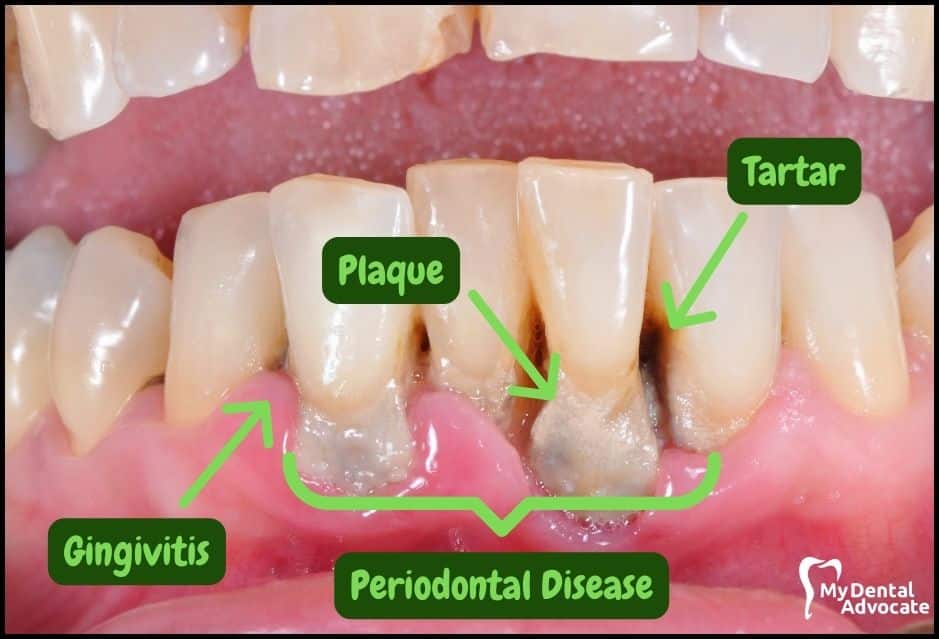
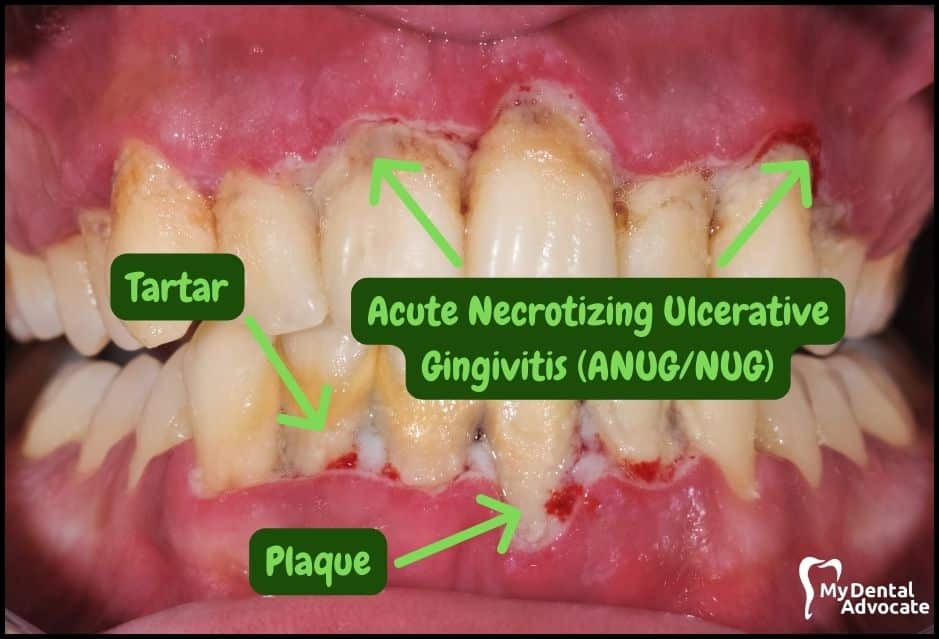

Causes of Gingivitis
Harmful bacteria in the mouth infect gum tissue surrounding the tooth.
Soft and hard tissue (bone) become inflamed, leading to periodontal disease. When bacteria stay on the teeth for an extended period, they form a sticky film called plaque, which eventually hardens to tartar, also called calculus.
Tartar build-up typically occurs above the gums; however, it can spread below the gum line, which makes the teeth more challenging to clean. When the bacteria progress below the gum line it invades sensitive space around the teeth.
The bone and gums physically move away from the “harmful agent” (bacteria).
Common Causes
- Poor Oral Hygiene: Skipping regular brushing and flossing leads to dental plaque and gum inflammation. Good oral hygiene and dental check-ups can prevent this. Neglect can lead to serious gum disease.
- Poor Nutrition’s Role: Harmful bacteria thrive on sugars and carbs. These bacteria grow and can harm gums. Avoiding sugary, sticky foods helps prevent this.
- Dental Plaque Explained: Plaque forms from food debris, especially along gums and teeth. It feels fuzzy and feeds on sugars, causing gum inflammation. Brush and floss daily to control plaque.
- The Problem with Tartar: Plaque can harden into tartar under the gums, attracting more bacteria. Tartar creates a shield for bacteria and irritates gums. Unlike plaque, tartar must be removed professionally.
Recommended Reading: 6 Best Mouthwashes for Gingivitis & Gum Disease 2026
Symptoms of Gingivitis
It’s possible to have gingivitis and periodontitis without any symptoms.
However, there may be no discomfort or noticeable symptoms in mild cases of gingivitis. Often, it remains undetected for quite some time. The symptoms of gingivitis are somewhat non-specific.
The pink-salmon coloring and stippling in the gum tissue will often disappear. Also, the gums may appear shiny as the gum tissue becomes inflamed and stretched over the tissue surface.
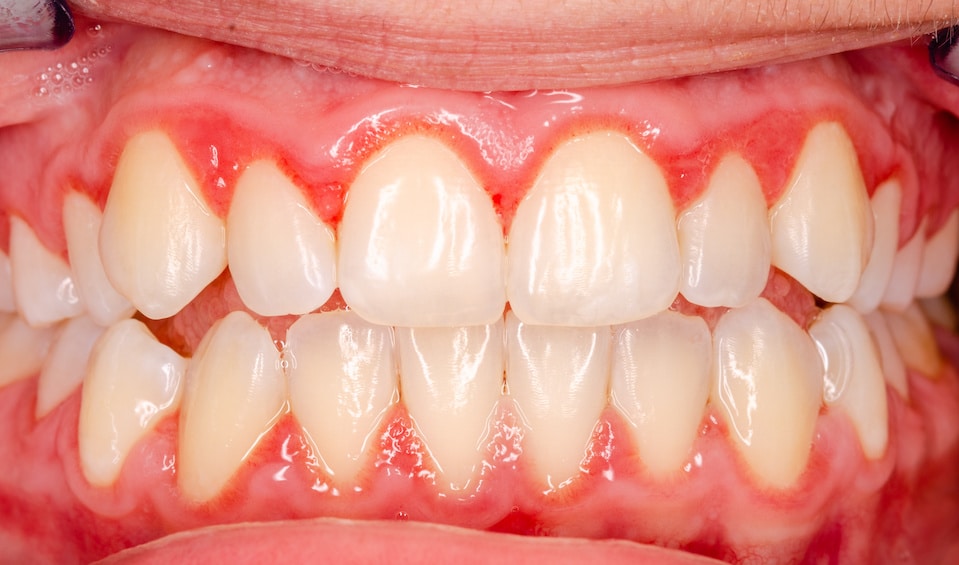
Gingivitis
- Red & purple gums
- Swollen & puffy gums
- Gum inflammation & discoloration
- Gum separation & recession
- Bleeding gums
- Halitosis (bad breath)
- Tender gums
Recommended Reading: Acute Necrotizing Ulcerative Gingivitis (ANUG) “Trench Mouth”
Treatment of Gingivitis
If you’re diagnosed with gingivitis, don’t panic.
Treatment is standard and includes a prophylaxis dental cleaning by your dentist or dental hygienist. In addition, oral health improvements are necessary to prevent harmful bacteria from re-seeding on your teeth.
For example, brush twice daily, floss regularly and use mouthwash nightly. Suppose you have braces or more significant gaps between your teeth. Use a water flosser. I recommend using BURST water flosser because of its portability, large water tank and replacement tips.
Recommended Reading: 5 Best Toothpastes for Gingivitis & Gum Disease 2026
Visit your dentist at least every 6 months for a dental check-up and routine dental cleaning.
Risk Factors
Specific risk factors increase the likelihood of developing gingivitis and periodontitis.
Certain medications, such as antiseizure and immunosuppressants, can lead to gingival hyperplasia (gum overgrowth).
Other Risk Factors
- Smoking or chewing tobacco
- Dry mouth
- Hormones
- Vitamin C deficiency
- Immunosuppressants
- Cardiovascular drugs
- Leukemia & HIV/AIDS
- Suppressed immunity
- Cancer
- Diabetes
- Pregnancy (hormones)
- Genetics (family history)
- Viral & fungal infections
- Orthodontics/braces
- Stress/anxiety
- Depression
- Crooked teeth
- Poor-fitting dental appliance
- Poor-fitting fillings
- Poor oral hygiene
Recommended Reading:Pregnancy Gingivitis: Causes, Symptoms & Treatment 2026
My Experience & Expertise
Gingivitis consists of gum inflammation without bone loss, whereas periodontitis (gum disease) features gum infection with bone loss.
In addition, gingivitis is reversible, whereas periodontal disease is irreversible. Understanding these significant differences will empower you to improve your oral health.
Need a second opinion? We can help! Learn more. Knowledge is power when cultivating healthy dental habits. The more informed you are, the better positioned you’ll be to prevent avoidable and potentially costly dental procedures for you and your family. Watch for future blog posts, where we’ll continue sharing important information, product reviews and practical advice!

About the Author
Dr. Matthew Hannan, also known as “Dr. Advocate,” is a board-certified dentist on a mission to provide accurate dental patient education. He attended Baylor University before completing dental school at UT Health San Antonio School of Dentistry. He now lives in Arizona with his beautiful wife and 4 kids. Dr. Hannan believes everyone should access easy-to-read dental resources with relevant, up-to-date dental research and insight to improve their oral health.

Connect with Dr. Hannan!
-
Sonicare 5300 Electric Toothbrush (Full Review)
Discover the secret to a healthier, brighter smile with the Philips Sonicare ProtectiveClean 5300 electric toothbrush. Expertly engineered for superior oral care, this innovative toothbrush provides an effective and tailored deep cleaning experience…
-
Do Pur Filters Remove Fluoride?
Access to clean and safe drinking water is necessary for human survival, yet many communities worldwide struggle with water contamination. For example, fluoride, a naturally occurring chemical, is often added…
-
What Does Gingivitis/Gum Disease Look Like? (20 Pictures)
Gingivitis is uncomfortable; your gums bleed, your breath smells, and your teeth hurt. But did you know that 94% of Americans have gingivitis? That’s an alarming statistic! However, what’s more alarming, gingivitis can progress…
Gain Clarity with Our FREE Second Opinion Guide
FREE online second opinion within 48 hours. No joke!
Product Reviews
Our 300+ dental product reviews (and counting), curated by an experienced dentist, are the most comprehensive online.
Toothbrush Genie
State-of-the-art chatbot designed to help you discover your perfect toothbrush in just a few simple steps!
Cavity Risk Assessment
Cutting-edge digital tool designed to evaluate your individual cavity risk based on your responses to a series of questions.
Gum Disease Assessment
Discover your gum disease risk with our quick and engaging 6-question assessment!