How Do CEREC Crowns Stay On? (Reasons Crowns Fall Off)
Do crowns fall off? If you are a patient who has had a CEREC crown placed, you may be wondering how it stays in place.
What type of cement or bonding agent is used? If the crown ever comes off, is there a particular way to re-cement it?
This blog post will answer these questions and provide the top 8 reasons crowns fall off from a dentist’s perspective.
Recommended Reading: CEREC Crowns | The Ultimate Guide
How Long Do CEREC Crowns Last?
CEREC crowns last 10-15 years; however, research is insufficient because it’s a newer restoration compared to gold or PFM (porcelain-fused-to-metal) crowns.
Need Dental Advice? It’s FREE!
In time we will learn more about longevity and long-term survival rate.
According to a recent study, the survival rate of CEREC CAD/CAM crowns after five years was 94.7%, and the survival rate after ten years was 85.7%.
The study results confirm that the long-term survival rate of CEREC restorations is comparable to gold crowns, considered the “gold standard” for dental crowns.

Increasing Crown Longevity
- Maintain oral health
- Brush twice per day
- Floss regularly
- Frequent dental check-ups
- Minimize sugar consumption
- Avoid sticky foods
- Wear occlusal guard at night
Recommended Reading: What Are CEREC Crowns? (Advantages & Disadvantages)
How Do Crowns Stay On?
Crowns are made from many materials, including gold, porcelain, metal, and zirconia. These materials interact differently with dental cement and other tooth bonding agents.
For example, gold and other metals cannot chemically bond to most bonding agents, so these crowns must rely on mechanical bonds.
Chemical Bond in Dentistry
Chemical bonds make crowns stick well.
When fixing a crown, we treat both the tooth and the crown. This way, they stick together using special cement.
This bond is strong and lasts long. But, doing it right needs skill.
We use this method for different crowns like CEREC, zirconia, or porcelain. It’s great for short teeth, like molars. Plus, it makes the crown stronger.
Even weaker crowns get tougher, reducing the risk of breaks.
Types
- Self-cured: Sets without light.
- Light-cured: Uses blue light to set.
Mechanical Bond in Dentistry
Mechanical bonds rely on tooth shape. Here, we focus on the tooth’s size and how it’s shaped.
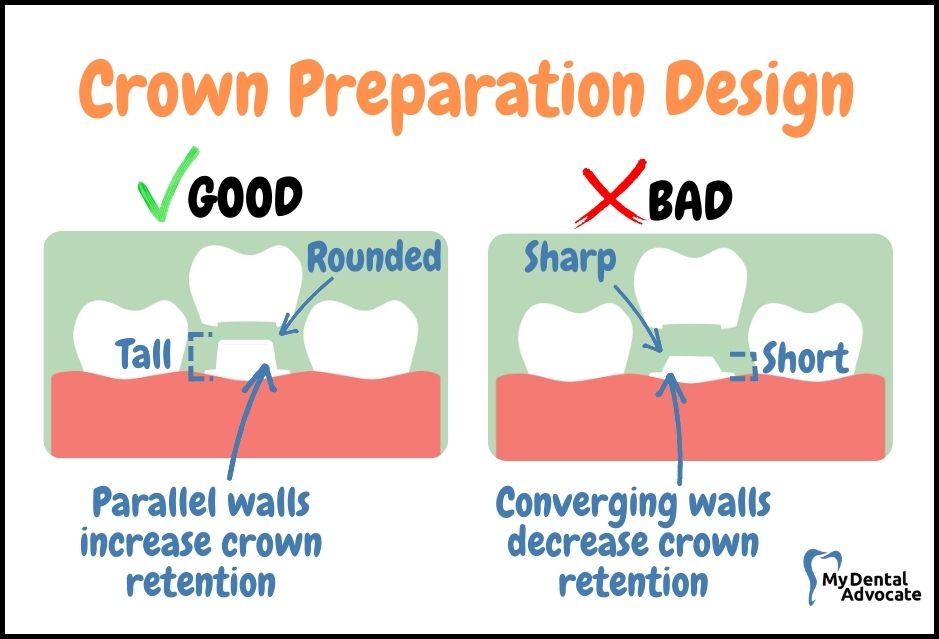
The tooth needs to be prepared so its walls are straight and tall. This stops the crown from moving or falling off. Gold and PFM crowns use this method because they can’t chemically bond to the tooth.
We use a special cement that locks in place.
The straighter and taller the tooth, the better the crown stays put.
Some cements can even absorb fluoride to protect against cavities around the crown’s edge.
Key Points
- Tooth Preparation: Tall, straight walls are crucial.
- Cement Type: Some can absorb fluoride for extra protection.
Both methods have their unique benefits. The choice depends on the tooth’s condition and the type of crown used.
CEREC Crowns & Tooth Decay
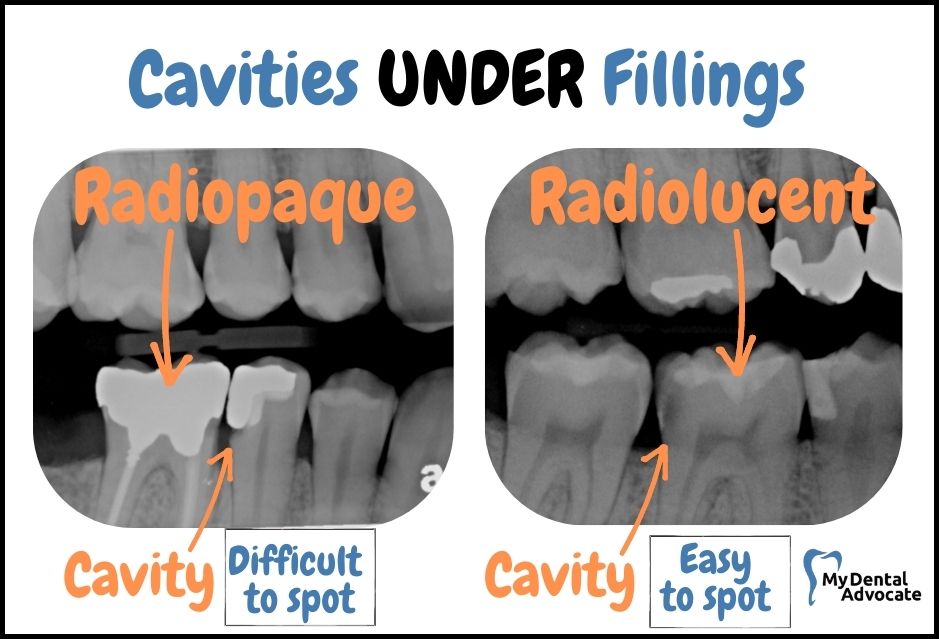
Aside from exceptional esthetics, same-day crown delivery, and durability, CEREC crowns are radiolucent. Radiolucent means that the material is transparent on an x-ray.
This feature is helpful for dentists because it allows the dentist to visualize any abnormality or cavity forming under existing crowns.
CEREC materials will enable the x-ray beam to pass through the crown and visualize structures under the restoration.
As a dentist, I greatly appreciate the ability to see a small cavity forming under an existing crown and manage it before the cavity progresses and requires further treatment, such as a root canal.
Unlike CEREC or other porcelain/ceramic crowns, gold, PFM, Zirconia, and metal crowns are radiopaque.
Radioopaque means that you can’t visualize anything under the material. Another way to describe it is the inability of the x-ray beam to travel through the metal crown, so it appears white on an x-ray.
Recommended Reading: When Are CEREC Crowns NOT Recommended (Top 6 Reasons)
Small cavities that form under the crown can be difficult to detect radiographically (with x-ray) until it’s too late and the cavity has caused extensive damage.
Dentists rely on instruments and tactile sensation to poke under metal crowns to feel for cavities.
Radiolucent Restorations
- Composite (tooth-colored) fillings
- CEREC crowns
- Inlays/Onlays
- Crown cement
- Sealants
Radiopaque Restorations
- Amalgam (silver-colored) fillings
- Gold crowns
- PFM crowns
- Zirconia crowns
- Titanium implants
Why Did My Crown Fall Off?
Dental crowns are cemented with traditional cement or bonding cement, and as mentioned, these two methods rely on chemical or mechanical bonds.
Chemical bonds are powerful and lasting.
However, the process is technique-sensitive, and the bond strength is greatly minimized if any contamination occurs.
On the other hand, mechanical bonds are less technique-sensitive for the dentist and have been around for hundreds of years—this process relies on the tooth’s shape and other physical properties.
According to a recent study, dentists were more likely to use bonding cement if there was excessive tooth reduction, anterior crowns were being cemented, or cementing a CEREC or other porcelain/ceramic crown.
The results clarified that 202 dentists cemented about 3,500 crowns; 38.1% bonded the crowns while 61.9% used traditional cement.
Recommended Reading: Help! My CEREC Crown Fell Off (BEST Recement Guide)
Common Reasons Crowns Fall Off
Crown failures can occur due to many issues.
Tooth Decay and Crowns
Cavities Under Crowns: Cavities can form under CEREC crowns and are visible on X-rays. If caught early, replacing the crown can avoid a root canal. Traditional crowns like gold, PFM, and Zirconia can hide cavities for years. Decay under failed crowns appears as a soft, discolored area. Large decay often means the tooth can’t be saved, leading to extraction and replacement options like bridges or implants.

Sticky Foods and Crowns
Foods That Dislodge Crowns: Beware of sticky foods! Bread and sweets like caramel or gummies can pull crowns off, especially energy gummies. Crowns bonded chemically are less likely to come off.
Short Teeth and Crown Issues
Challenges with Short Teeth: Short teeth, like lower molars, often lose crowns due to insufficient height. Chemically bonding crowns on short teeth improves their lifespan. Zirconia crowns are thin, strong, and ideal for molars, especially for those who grind their teeth.
Importance of Proper Tooth Preparation
Tooth Shaping for Crowns: Correct tooth shaping is key. The tooth must be trimmed to fit the crown and bite properly. Over-trimming leads to weak retention and an increased risk of crown loss. A mechanical fit needs tall, straight-tooth walls.
Cement Failure in Crowns
Choosing the Right Cement: Dentists must pick the right cement. Traditional cements need precise mixing. Errors in mixing can lead to crown failure. It’s best to use clinically proven cements for durability.

Dentist’s Skill in Crown Placement
Avoiding Dentist Errors: Proper use of dental cement is crucial. Bonding cements are sensitive to technique. Mistakes in application or contamination can weaken the bond. The entire process, from start to finish, requires teamwork for success.
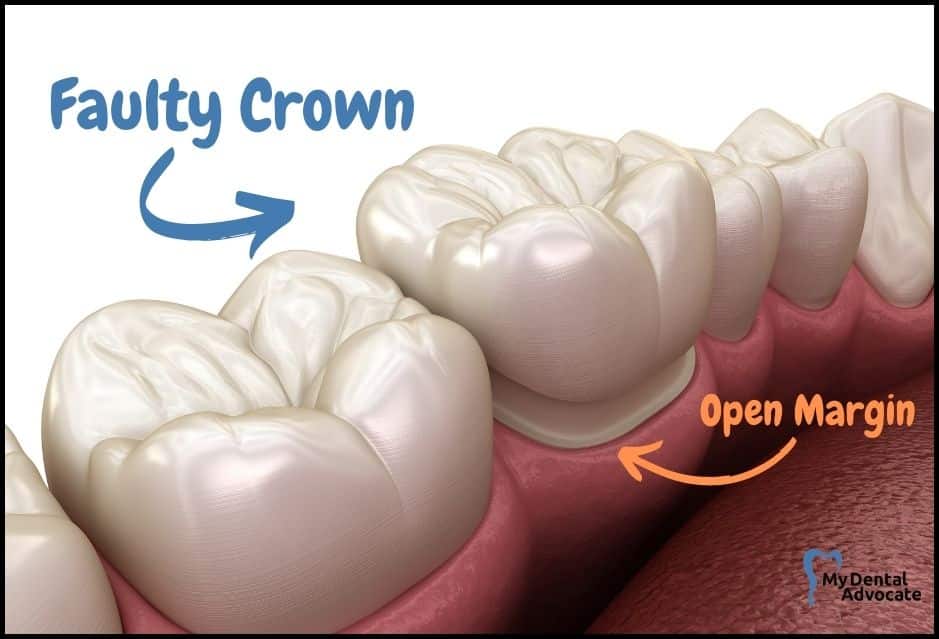
Risks of Faulty Crowns
Problems with Poorly Fitted Crowns: A loose-fitting crown won’t stay on. Open margins, where the crown doesn’t meet the tooth tightly, allow bacteria in, leading to decay and crown failure. An X-ray check before cementing is essential.
Bruxism and Crown Longevity
Grinding and Crown Loss: Patients who grind their teeth risk popping off their crowns. An occlusal guard can protect against this. Zirconia crowns are recommended for their strength and durability in these cases.
My Experience & Expertise
In my practice, the most common reasons CEREC crowns fall off are sticky foods or cement failure due to contamination during the bonding process.
However, all dental crowns are susceptible to falling off. Understanding why it fell off is the first step to moving forward with treatment. Learn how to temporarily recement your dental crown and visit your dentist as soon as possible for repair.
Need a second opinion? We can help! Learn more. Knowledge is power when cultivating healthy dental habits. The more informed you are, the better positioned you’ll be to prevent avoidable and potentially costly dental procedures for you and your family. Watch for future blog posts, where we’ll continue sharing important information, product reviews and practical advice!

About the Author
Dr. Matthew Hannan is a board-certified dentist on a mission to provide accurate dental patient education. He attended Baylor University before completing dental school at UT Health San Antonio School of Dentistry. He now lives in Arizona with his beautiful wife and 4 kids. Dr. Hannan believes everyone should access easy-to-read dental resources with relevant, up-to-date dental research and insight to improve their oral health.

Connect with Dr. Hannan!
-
Best Alkaline Mouthwash 2026 (Top Picks)
Oral health is not just about pearly whites and fresh breath. The pH level in the mouth plays a crucial role in determining overall dental well-being. With the modern diet often leaning towards the acidic side, an alkaline mouthwash can be a game changer, helping to neutralize excess acid, and providing a protective shield against tooth decay and gum disease.
-
Best Electric Toothbrush for Sensitive Teeth 2026 (Dentist-Recommended)
Looking for the best electric toothbrush for sensitive teeth? As a dentist, I understand the challenge. Let’s explore top picks that combine gentle cleaning with effective oral care. As an experienced dentist with years of experience, I’ve tested and evaluated 250+ dental products. I strive to find the best products for achieving excellent oral hygiene, so let’s take a closer look at the Best Electric Toothbrush for Sensitive Teeth from a dentist’s perspective.
-
Benefits of Dental Second Opinion (Dentist’s Perspective)
Visiting a dentist is stressful enough. If you’re diagnosed with hundreds or thousands of dollars of dental work, your stress goes thru the roof. So do you take the dentist’s word or seek a second opinion? What are the benefits of a second opinion? Second opinions provide clarity for proposed dental treatment…
Gain Clarity with Our FREE Second Opinion Guide
FREE online second opinion within 48 hours. No joke!
Product Reviews
Our 300+ dental product reviews (and counting), curated by an experienced dentist, are the most comprehensive online.
Toothbrush Genie
State-of-the-art chatbot designed to help you discover your perfect toothbrush in just a few simple steps!
Cavity Risk Assessment
Cutting-edge digital tool designed to evaluate your individual cavity risk based on your responses to a series of questions.
Gum Disease Assessment
Discover your gum disease risk with our quick and engaging 6-question assessment!





